Ati Lpn maternal exam 1
Ati Lpn maternal exam 1
Total Questions : 49
Showing 10 questions Sign up for moreA nurse in the antepartum unit is assisting with the care of a client who is at 36 weeks of gestation and reports continuous abdominal pain and vaginal bleeding.
The nurse should identify that the client is likely experiencing which of the following complications?
Explanation
The correct answer is choice C, Abruptio placentae.
Choice A rationale:
A prolapsed cord is an obstetric emergency where the umbilical cord drops (prolapses) through the open cervix into the vagina ahead of the baby. It’s a rare condition but can occur during labor if the baby is not yet engaged, and the water breaks. The main concern is that the cord can become compressed, cutting off the baby’s oxygen supply. However, it does not typically present with continuous abdominal pain and vaginal bleeding without labor.
Choice B rationale:
Premature rupture of membranes (PROM) refers to a patient whose membranes have ruptured before the onset of labor. While PROM can lead to complications, it is not typically associated with continuous abdominal pain and vaginal bleeding. PROM is more often characterized by the sudden release of fluid from the vagina.
Choice C rationale:
Abruptio placentae, also known as placental abruption, is the premature separation of the placenta from the uterus. It is a serious condition that can occur in the third trimester and is associated with continuous abdominal pain and vaginal bleeding, which are the symptoms described in the question. This condition poses significant risks to both the mother and the fetus, including fetal distress, preterm birth, and maternal hemorrhage.
Choice D rationale:
Placenta previa is a condition where the placenta covers the cervix either completely or partially. It can cause painless, bright red vaginal bleeding but is not typically associated with abdominal pain. The bleeding with placenta previa is usually not continuous but rather occurs in episodes.
In this scenario, the continuous abdominal pain and vaginal bleeding are classic signs of abruptio placentae, making Choice C the most likely diagnosis.
A nurse should include which of the following information?
Explanation
The correct answer is choice b. Quickening occurs between the fourth and fifth months of pregnancy.
Choice A rationale:
Quickening does not start soon after implantation. Implantation occurs around 6-10 days after fertilization, but quickening, which is the first feeling of fetal movements, typically happens much later in pregnancy.
Choice B rationale:
This is the correct answer. Quickening usually occurs between 16 to 20 weeks of pregnancy, which corresponds to the fourth and fifth months.
Choice C rationale:
Quickening does not start during the last trimester. By the last trimester, fetal movements are usually strong and frequent, and the mother has been feeling them for several months.
Choice D rationale:
Quickening does not occur between the second and third month of pregnancy. At this stage, the fetus is still too small for its movements to be felt by the mother.
A nurse is caring for a client who is pregnant in a provider’s office.
Relevant vital signs to help answer the questions are as follows: Medical History: 0830 Gravida 3 Para 2, 32 weeks of gestation, Allergies: Penicillin, Height: 163 cm, Weight: 78 kg, BMI: 30.6, 6 lb weight gain over the last 2 weeks.
The client reports “I have had a headache for 5 days, blurred vision, and dizziness. Tylenol does not relieve it.” The client reports swelling of their feet and fingers.
2+ pitting edema of the lower extremities noted bilaterally. Swelling of the fingers and hands noted.
Deep tendon reflexes 3+, absent clonus.
Fetal heart tones (FHT) 1. Which of the following findings should the nurse report to the provider? Select all that apply.
Explanation
Rationale for Choice A: Visual disturbances
Preeclampsia: Visual disturbances, such as blurred vision or seeing spots, can be a sign of preeclampsia, a serious pregnancy complication characterized by high blood pressure and protein in the urine. It typically develops after 20 weeks of gestation and can progress rapidly.
Potential complications: If left untreated, preeclampsia can lead to seizures (eclampsia), stroke, liver and kidney failure, premature birth, and even death of the mother or baby.
Prompt reporting: Early recognition and management of preeclampsia are crucial for preventing adverse outcomes. Therefore, visual disturbances should be reported to the provider immediately to initiate further assessment and potential interventions.
Rationale for Choice B: Fetal heart rate
No indication for reporting: While monitoring fetal heart rate is essential during pregnancy, the promptness of reporting it to the provider depends on specific concerns. In this case, the fetal heart tones are documented as 1, suggesting a normal rate and rhythm. There's no immediate indication for reporting it as a concerning finding.
Rationale for Choice C: Blood pressure
Hypertension: High blood pressure is a key feature of preeclampsia. Although blood pressure readings are not provided in the scenario, the nurse should measure and report them to the provider, as hypertension is a critical finding that could necessitate further evaluation and treatment.
Rationale for Choice D: Deep tendon reflexes
Hyperreflexia: The client's deep tendon reflexes are 3+, which is considered hyperreflexia. Hyperreflexia can be a neurological sign of preeclampsia, indicating increased excitability of the nervous system. It's important to report this finding to the provider for further assessment and monitoring.
A nurse is reinforcing nutrition teaching with a client during the first prenatal visit. Which of the following statements by the client indicates understanding of the teaching?
Explanation
Choice A rationale:
Consuming any amount of alcohol during pregnancy is not recommended. Alcohol can cross the placenta and harm the developing fetus, potentially leading to fetal alcohol spectrum disorders (FASDs). FASDs can cause a range of physical, mental, and behavioral problems, including intellectual disabilities, learning disabilities, and physical abnormalities. Even small amounts of alcohol can increase the risk of FASDs, and there is no known safe amount of alcohol to consume during pregnancy.
Choice B rationale:
Switching to whole milk during pregnancy can be a beneficial choice for several reasons:
Increased calcium and vitamin D: Whole milk is a rich source of calcium and vitamin D, which are essential for the development of the baby's bones, teeth, and muscles. Calcium also supports the mother's bone health and helps prevent pregnancy-related osteoporosis.
Healthy fats: Whole milk contains healthy fats that are important for fetal brain development and the mother's overall health. These fats also contribute to satiety and can help manage weight gain during pregnancy.
Essential nutrients: Whole milk provides a variety of other essential nutrients, including protein, vitamins A and B12, riboflavin, and zinc. These nutrients support overall health and well-being during pregnancy.
Choice C rationale:
Weight loss during pregnancy is generally not recommended unless specifically advised by a healthcare provider. Pregnancy is a time for growth and nourishment of the baby, and restricting calories or attempting to lose weight can potentially harm the developing fetus. It's important to focus on consuming a healthy, balanced diet and gaining a healthy amount of weight during pregnancy.
Choice D rationale:
Consuming high amounts of caffeine during pregnancy is not recommended. Caffeine can cross the placenta and potentially affect the baby's heart rate and sleep patterns. It's generally advised to limit caffeine intake to less than 200 milligrams per day during pregnancy.
A nurse is assisting with a community program to educate adolescents about contraception. After the class, a 15-year-old girl asks the nurse which method is best for her to use.
Which of the following statements is an appropriate nursing response?
Explanation
Rationale for Choice A:
Judgmental and shaming: The statement "You are so young. Are you sure you are ready for the responsibilities of a sexual relationship?" conveys judgment and may make the adolescent feel ashamed or embarrassed. This can create a barrier to open communication and discourage the teen from seeking further guidance.
Dismisses the teen's concerns: It does not directly address the teen's question about contraception, suggesting that her concerns are not valid or important.
Does not provide helpful information: It does not offer any guidance or education about contraception, leaving the teen without the information she needs to make informed decisions about her sexual health.
Rationale for Choice B:
Erects barriers to access: Requiring parental consent for an examination can delay or prevent the teen from obtaining contraception, even if she is legally allowed to do so without parental consent.
Discourages open communication: It may make the teen feel like she cannot trust the nurse or that her privacy will not be respected, leading her to withhold information or avoid seeking further help.
Rationale for Choice C:
Defers responsibility: It shifts the responsibility for providing contraception counseling to the doctor, potentially delaying the teen's access to information and services.
May not be necessary: A physical examination is not always required before prescribing contraception, and in some cases, a nurse practitioner or other qualified health professional can provide this service.
Rationale for Choice D:
Open and non-judgmental: It invites the teen to share information about her sexual activity without judgment or pressure. Gathers essential information: It allows the nurse to assess the teen's individual needs and preferences, which is crucial for recommending the most appropriate contraceptive method.
Promotes informed decision-making: It empowers the teen to make informed choices about her sexual health by providing her with accurate and comprehensive information about contraception.
A nurse is caring for a 22-year-old female client who is experiencing lower abdominal pelvic pain. The client is at risk of developing a condition due to a finding.
Explanation
Choice A rationale:
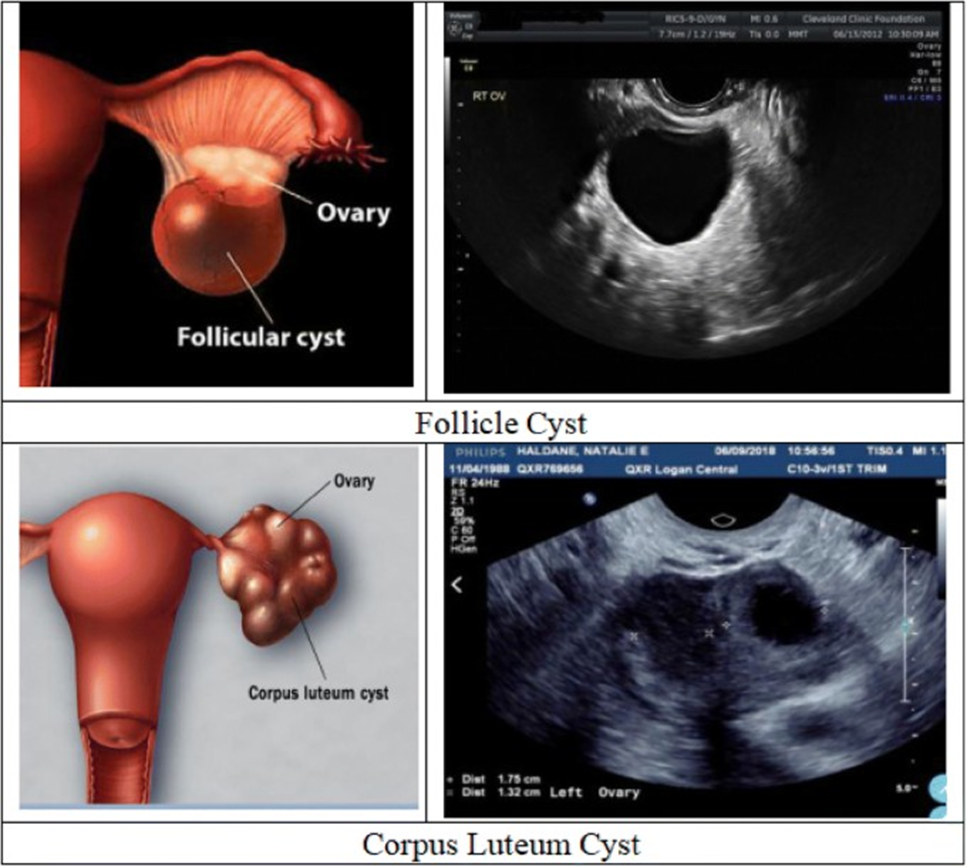
Ovarian cysts are fluid-filled sacs that form on or within an ovary. They are a common condition, affecting up to 1 in 5 women at some point in their lives. While most ovarian cysts are benign (non-cancerous), they can sometimes cause symptoms, including pelvic pain.
Ultrasound is a common imaging test that uses sound waves to create pictures of internal organs. It can be used to detect ovarian cysts, which often appear as fluid-filled sacs on the ovary.
The presence of an ovarian cyst on ultrasound, combined with the patient's symptoms of lower abdominal pelvic pain, suggests that the patient is at risk of developing complications from the cyst. These complications can include: Rupture: A ruptured ovarian cyst can cause sudden, severe pain and bleeding.
Torsion: This is when a cyst twists on its stalk, cutting off its blood supply. Torsion can also cause severe pain and may require emergency surgery.
Choice B rationale:
Appendicitis is an inflammation of the appendix, a small, finger-shaped organ located in the lower right abdomen. It is a common cause of abdominal pain, especially in young adults.
However, the patient in this scenario is experiencing pain in the lower abdominal pelvic region, not specifically in the lower right quadrant. This makes appendicitis less likely.
Additionally, the patient does not have any other symptoms that are typically associated with appendicitis, such as fever, nausea, or vomiting.
Choice C rationale:
Endometriosis is a condition in which tissue that normally lines the uterus grows outside of the uterus. It can cause pain, especially during menstruation.
However, the patient in this scenario does not report cyclical pain, which is a hallmark symptom of endometriosis. Additionally, endometriosis is not typically associated with the presence of fluid-filled sacs on the ovaries.
Choice D rationale:
Pelvic inflammatory disease (PID) is an infection of the upper genital tract, including the uterus, fallopian tubes, and ovaries. It is often caused by sexually transmitted infections (STIs).
PID can cause pelvic pain, but it is also typically associated with other symptoms, such as fever, vaginal discharge, and irregular bleeding.
The patient in this scenario does not have any of these other symptoms, and her white blood cell count is not elevated, which makes PID less likely.
A nurse is admitting a client who is at 36 weeks gestation and has pain, bright red vaginal bleeding. The nurse recognizes this finding as an indication of which of the following conditions? Choice Options:
Explanation
The correct answer is choice b. Placenta previa.
Choice A rationale:
Threatened abortion typically occurs in the first trimester and involves vaginal bleeding with or without abdominal pain. It is not associated with late pregnancy bleeding.
Choice B rationale:
Placenta previa is characterized by painless, bright red vaginal bleeding in the third trimester. It occurs when the placenta covers the cervix, leading to bleeding as the cervix begins to dilate.
Choice C rationale:
Preterm labor involves uterine contractions leading to cervical changes before 37 weeks of gestation. While it can cause bleeding, it is usually accompanied by regular contractions and not typically described as bright red bleeding.
Choice D rationale:
Abruptio placentae involves the premature separation of the placenta from the uterine wall, leading to painful, dark red vaginal bleeding. It is often associated with abdominal pain and uterine tenderness, which differentiates it from placenta previa.
A nurse is teaching a client who is scheduled for a non-stress test. Which of the following information should the nurse include? Choice Options:
Explanation
Rationale for Choice A:
An IV is not routinely initiated prior to a non-stress test. It may be started if a biophysical profile (BPP), which includes an ultrasound, is also being performed, or if there is a risk of complications that may necessitate immediate intervention. However, it is not a standard part of the non-stress test itself.
Rationale for Choice B:
Nipple stimulation is not a standard component of a non-stress test. It may be used in some cases to try to induce fetal movement if the fetus is not moving actively enough during the test. However, it is not a routine part of the procedure.
Rationale for Choice C:
An ultrasound is not typically performed prior to a non-stress test. It may be done as part of a BPP, but it is not necessary for the non-stress test itself.
Rationale for Choice D:
An external fetal monitor is essential for conducting a non-stress test. This monitor uses two belts that are placed around the mother's abdomen. One belt measures the fetal heart rate, and the other belt measures uterine contractions. The monitor records the fetal heart rate and any contractions for a period of 20 to 40 minutes. The test is considered reactive (normal) if the fetal heart rate increases by at least 15 beats per minute for at least 15 seconds twice during the test. This acceleration in heart rate is typically in response to fetal movement.
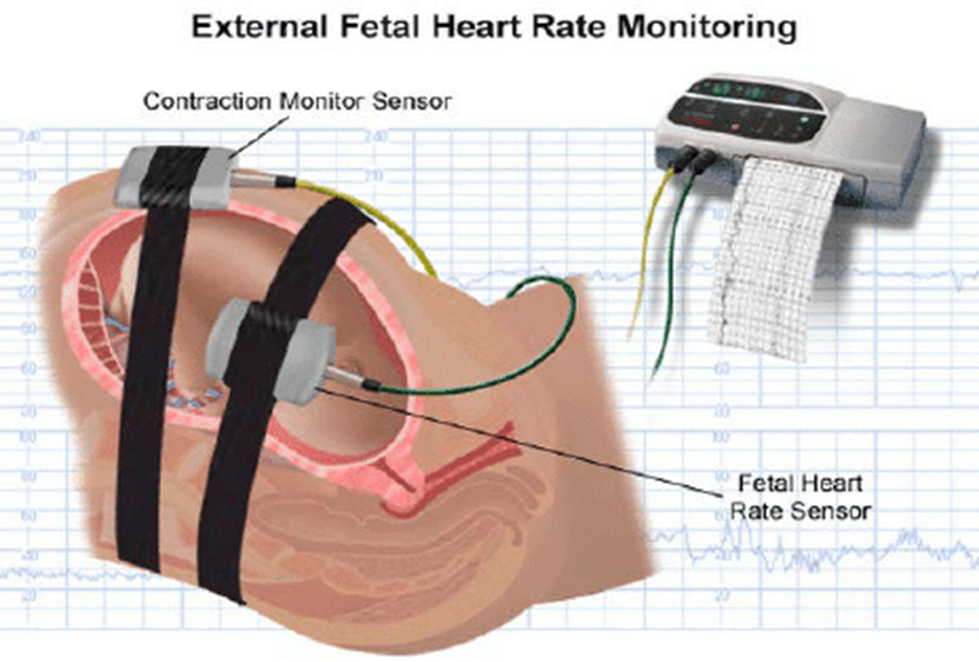
A nurse in a provider’s office is reinforcing teaching about home care to a client who has mild preeclampsia. Which of the following information should the nurse include in the teaching? Choice Options:
Explanation
Choice A rationale:
Fetal movement counts are a simple yet effective tool to monitor fetal well-being in women with preeclampsia. They provide valuable insights into the baby's activity level and can alert the healthcare team to potential concerns early on.
Preeclampsia can compromise placental blood flow, which can lead to decreased fetal movement. By tracking fetal movements daily, the mother can detect any significant changes or reductions in activity, prompting further assessment and intervention if necessary.
Research has shown that regular fetal movement counts can reduce the risk of stillbirth in women with preeclampsia. This is because prompt recognition of decreased fetal movements allows for timely interventions, such as closer monitoring, induction of labor, or delivery, to prevent adverse outcomes.
Daily fetal movement counts empower women to take an active role in their pregnancy care and contribute to a sense of control in a condition that can often feel unpredictable. This increased involvement can promote maternal-fetal bonding and reduce anxiety.
Choice B rationale:
While fluid restriction has been a traditional recommendation for preeclampsia, current evidence does not support limiting fluid intake to 1,000 ml/day. In fact, excessive fluid restriction can lead to dehydration, which can worsen placental perfusion and compromise fetal well-being.
It's essential for women with preeclampsia to maintain adequate hydration to support essential bodily functions and fetal growth. Adequate fluid intake also helps to prevent urinary tract infections, which are more common in women with preeclampsia.
Choice C rationale:
Although reducing sodium intake can be beneficial for overall blood pressure control, there's insufficient evidence to support a strict sodium restriction of 2,000 mg/day specifically for managing mild preeclampsia. Individual needs may vary, and a more moderate approach to sodium reduction is often recommended.
Focusing on a balanced, healthy diet with appropriate sodium intake is generally more effective than strict limitations. This approach promotes overall well-being and supports healthy blood pressure levels without compromising nutritional needs. Choice D rationale:
Rest is often recommended for women with preeclampsia to reduce stress on the cardiovascular system and promote placental blood flow. However, the supine position (lying on the back) is not ideal, as it can further compress the large blood vessels in the abdomen and potentially reduce blood flow to the placenta.
Side-lying positions, particularly the left lateral position, are preferred for women with preeclampsia. These positions help to alleviate pressure on the major blood vessels, enhance blood flow, and improve uteroplacental circulation, which benefits both the mother and the baby.
The nurse is caring for a client who might have a hydatidiform mole. The nurse should monitor the client for which of the following findings? Choice Options:
Explanation
Rationale for Choice A: Whitish vaginal discharge
While whitish vaginal discharge can occur in some cases of hydatidiform mole, it's not a specific or sensitive finding for this condition.
It can also be present in various other gynecological conditions, including normal pregnancy, infections, and hormonal imbalances.
Therefore, relying on whitish vaginal discharge alone for monitoring a potential hydatidiform mole could lead to misdiagnosis or delayed diagnosis.
Rationale for Choice B: Excessive uterine enlargement
Excessive uterine enlargement is a common sign of hydatidiform mole, but it's not always present and might not be detected early in the condition.
The uterus might not be significantly enlarged in early stages, and other factors like multiple pregnancies or uterine fibroids could also contribute to uterine enlargement.
Solely relying on uterine enlargement could miss cases of hydatidiform mole that haven't progressed to a noticeable degree.
Rationale for Choice C: Fetal heart rate irregularities
Fetal heart rate irregularities are not relevant in hydatidiform mole because there is no viable fetus present. Hydatidiform moles are characterized by abnormal growth of placental tissue without a normal fetus developing. Monitoring for fetal heart rate would be inappropriate and misleading in this context.
Rationale for Choice D: Rapidly changing hCG levels
This is the most accurate and reliable finding to monitor for in a suspected hydatidiform mole.
hCG is a hormone produced by the placenta, and it's typically elevated in pregnancy. However, in hydatidiform mole, hCG levels are often abnormally high and rise rapidly.
Serial hCG measurements can accurately detect and track the progression of a hydatidiform mole, even in its early stages. It's considered the gold standard for diagnosis and monitoring of this condition.
You just viewed 10 questions out of the 49 questions on the Ati Lpn maternal exam 1 Exam. Subscribe to our Premium Package to obtain access on all the questions and have unlimited access on all Exams. Subscribe Now



