Which of the following ECG rhythm interval measures is considered abnormal?
QTc interval 0.33 to 0.47 seconds
QT interval that varies with HR
QRS interval <0.12 seconds
PR interval 0.12 to 0.24 seconds
The Correct Answer is A
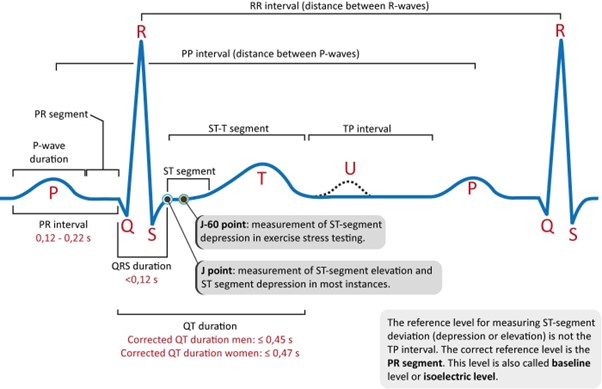
The QTc (corrected QT) interval is a measure of the time it takes for the ventricles to depolarize and repolarize during a cardiac cycle. It is corrected for heart rate (HR) to account for variations in the cardiac cycle length.
The normal range for the QTc interval varies depending on the calculation method used but generally falls within 0.36 to 0.44 seconds. In the given options, the range of 0.33 to 0.47 seconds for the QTc interval is wider than the normal range, suggesting a prolonged QTc interval, which can be indicative of a potential risk for arrhythmias, including ventricular tachycardia and torsades de pointes.
B. QT interval that varies with HR in (option B) is normal because The QT interval alone can vary with heart rate, and this is considered a normal physiological adaptation.
C. QRS interval <0.12 seconds in (option C) is normal because The QRS interval represents the time it takes for ventricular depolarization and is normally less than 0.12 seconds.
D. PR interval 0.12 to 0.24 seconds in (option D) is normal because The PR interval represents the time it takes for atrial depolarization and conduction through the AV node. The normal range is typically 0.12 to 0.20 seconds.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
A. Oxygen saturation of 92% in (option A) is incorrect because While an oxygen saturation of 92% is suboptimal and may require intervention, it may not have the same immediate implications as low blood pressure. The healthcare provider should be informed, but addressing the blood pressure takes priority.
B. Skin cool and clammy in (option B) is correct because Cool and clammy skin is often associated with inadequate peripheral perfusion, which is a characteristic of septic shock.
C. Septic shock is characterized by systemic inflammation, vasodilation, and hypotension. Inadequate blood pressure is a significant concern in septic shock as it indicates poor tissue perfusion and compromised organ function. However, the mean arterial pressure is till acceptable.
D. Heart rate of 118 beats/minute in (option D) is incorrect because: Tachycardia is a common finding in septic shock and reflects the body's compensatory response to maintain cardiac output. While it is a significant finding, low blood pressure takes precedence in terms of urgency.
Correct Answer is C
Explanation
Septic shock is characterized by inadequate tissue perfusion and hypotension, which can lead to organ dysfunction and failure. The administration of intravenous fluids, such as a normal saline bolus, is the initial priority in the management of septic shock to restore intravascular volume and improve perfusion.
A. Draw an arterial blood gas (ABG) in (option A) is incorrect because: ABG may be ordered to assess the patient's acid-base status and oxygenation, but addressing hypotension and restoring perfusion through fluid administration takes priority.
B. Start insulin drip to maintain blood glucose at 150 mg/dl or lower in (option B) is incorrect because: Hyperglycaemia is commonly observed in critically ill patients, including those with septic shock. While controlling blood glucose is important, it is not the immediate priority compared to addressing hypotension and restoring intravascular volume.
D. Titrate norepinephrine (Levophed) to keep mean arterial pressure (MAP) greater than 65 mm Hg in (option D) is incorrect because: Norepinephrine is a vasopressor medication used to increase blood pressure and perfusion in septic shock. While it may be necessary for the management of septic shock, fluid resuscitation should be initiated first to optimize intravascular volume before starting vasopressors.
Therefore, the first order that the nurse should accomplish in this scenario is to give a normal saline bolus IV of 30 mL/kg to address the hypotension and restore intravascular volume.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
