Which assessment information obtained by the nurse when caring for a COPD patient receiving mechanical ventilation indicates the need for suctioning?
The pulse oximeter shows a Sp02 of 90%.
The patient has not been suctioned for the last 6 hours.
The respiratory rate is 32 breaths/min.
The lungs have occasional audible expiratory wheezes.
The Correct Answer is C
In a patient receiving mechanical ventilation, a high respiratory rate can indicate increased work of breathing and potential airway obstruction. COPD patients, in particular, may have excessive mucus production and airway inflammation, leading to mucus plugging and compromised airway clearance. Suctioning may be necessary to remove excessive secretions and maintain a patent airway.
A. The pulse oximeter shows a SpO2 of 90% in (option A) is incorrect because While a SpO2 of 90% is suboptimal and may require intervention, it does not specifically indicate the need for suctioning. Other interventions, such as adjusting oxygen delivery or ventilation settings, may be more appropriate.
B. The patient has not been suctioned for the last 6 hours in (option B) is incorrect because The duration since the last suctioning episode alone does not necessarily indicate the need for suctioning. The need for suctioning should be based on the patient's clinical presentation, such as signs of airway obstruction or excessive secretions.
D. The lungs have occasional audible expiratory wheezes in (option D) which is incorrect because Occasional audible expiratory wheezes may be common in patients with COPD and may not specifically indicate the need for suctioning. Wheezing is more commonly associated with narrowing of the airways, and suctioning is typically performed to clear secretions or maintain airway patency.
C. Therefore, in a COPD patient receiving mechanical ventilation, a high respiratory rate (C) is the assessment information that would indicate the need for suctioning to help remove excessive secretions and ensure a patent airway
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
The increased respiratory rate and pulse rate can be indicators of physiological changes or potential complications in the patient's condition. These changes may suggest alterations in tissue perfusion or other underlying issues that require further assessment.
Assessing the patient's tissue perfusion includes evaluating additional vital signs, such as blood pressure, oxygen saturation, and capillary refill time. Assessing skin color, temperature, and moisture, as well as peripheral pulses, can also provide important information regarding tissue perfusion.
B. Pain medication (option B) is incorrect because the increased respiratory and pulse rates could also indicate other factors that require assessment before administering pain medication.
C. Documenting the findings in the patient's chart (option C) is incorrect because it should not be the primary action at this point. Assessing the patient's condition and determining appropriate interventions take priority.
D. Increasing the rate of the patient's IV infusion (option D) is incorrect because may not be the most appropriate action without further assessment. The patient's increased respiratory and pulse rates may not necessarily be related to hydration status, and it is important to assess the patient comprehensively before making changes to the IV infusion rate.
Therefore, the best action by the nurse in this situation is to further assess the patient's tissue perfusion to gather more information and determine the appropriate course of action.
Correct Answer is D
Explanation
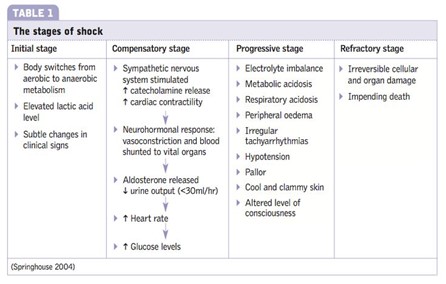
In the compensatory stage of shock, the body initiates various mechanisms to maintain perfusion to vital organs and restore homeostasis. Activation of the renin-angiotensin system is one of the compensatory responses. The decreased blood flow and oxygen delivery to the kidneys stimulate the release of renin from the kidneys. Renin acts on angiotensinogen, converting it into angiotensin I, which is further converted to angiotensin II by the action of angiotensin-converting enzyme (ACE). Angiotensin II is a potent vasoconstrictor and also stimulates the release of aldosterone, leading to sodium and water retention. These mechanisms aim to increase blood pressure and cardiac output and restore fluid balance.
A. The initial stage of shock in (option A) is incorrect because it is characterized by inadequate tissue perfusion and the activation of various compensatory mechanisms, including the release of stress hormones. However, the renin-angiotensin system is not specifically mentioned as activated in this stage.
B. The progressive stage of shock in (option B) is incorrect because it occurs when compensatory mechanisms fail to maintain adequate perfusion, leading to worsening hypoperfusion and organ dysfunction. The renin-angiotensin system continues to be activated during this stage, but it is primarily associated with the compensatory stage.
C. The refractory stage of shock in (option C) is incorrect because it is the stage of severe and prolonged hypoperfusion, where organ failure becomes irreversible. The renin-angiotensin system may still be activated, but it is not the primary focus of this stage.
Therefore, the activation of the renin-angiotensin system occurs during the compensatory stage of shock.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
