A 78-kg patient with septic shock has a urine output of 30 mL/hr for the past 3 hours. The pulse rate is 120/minute and the central venous pressure and pulmonary artery wed pressure are low. Which order by the health care provider will the nurse question?
Administer hydrocortisone (Solu-Cortef) 100 mg IV.
Give PRN furosemide (Lasix) 40 mg IV.
Increase normal saline infusion to 250 mL/hr.
Titrate norepinephrine (Levophed) to keep systolic BP >90 mm Hg.
The Correct Answer is C
In septic shock, one of the key goals of management is to restore and maintain adequate intravascular volume. However, in this case, the patient's urine output is low (30 mL/hr for the past 3 hours), suggesting inadequate renal perfusion and potential fluid overload.
Administering additional normal saline at an increased rate (250 mL/hr) without addressing the low urine output could potentially exacerbate fluid overload and further compromise the patient's condition.
A. Administer hydrocortisone (Solu-Cortef) 100 mg IV in (option A) is incorrect because: Hydrocortisone is commonly used in septic shock to help stabilize blood pressure and modulate the inflammatory response.
B. Giving PRN furosemide (Lasix) 40 mg IV in (option B) is incorrect because Furosemide, a loop diuretic, can be administered as needed to address fluid overload or to increase urine output if there is evidence of volume overload.
D. Titrate norepinephrine (Levophed) to keep systolic BP >90 mm Hg in (option D) is incorrect because: Norepinephrine is a vasopressor commonly used in septic shock to increase systemic vascular resistance and maintain adequate blood pressure.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
Systemic vascular resistance represents the resistance to blood flow in the systemic circulation. It is an important indicator of afterload, which is the force against which the left ventricle must pump to eject blood into the systemic circulation. By monitoring the changes in SVR, the nurse can assess the impact of medications aimed at reducing left ventricular afterload.
A. Pulmonary artery wedge pressure (PAWP) in (option A) is incorrect because: PAWP is a measure of left ventricular preload and reflects the pressure within the left atrium and left ventricle at end-diastole. It is not specifically related to afterload reduction.
C. Pulmonary vascular resistance (PVR) in (option C) is incorrect because: PVR represents the resistance to blood flow in the pulmonary circulation. It is not directly related to left ventricular afterload.
D. Central venous pressure (CVP) in (option D) is incorrect because: CVP reflects the pressure in the right atrium and is an indicator of right-sided cardiac function. It is not specifically related to left ventricular afterload reduction.
Therefore, to assess the effectiveness of medications in reducing left ventricular afterload, the nurse should monitor the systemic vascular resistance (SVR).
Correct Answer is D
Explanation
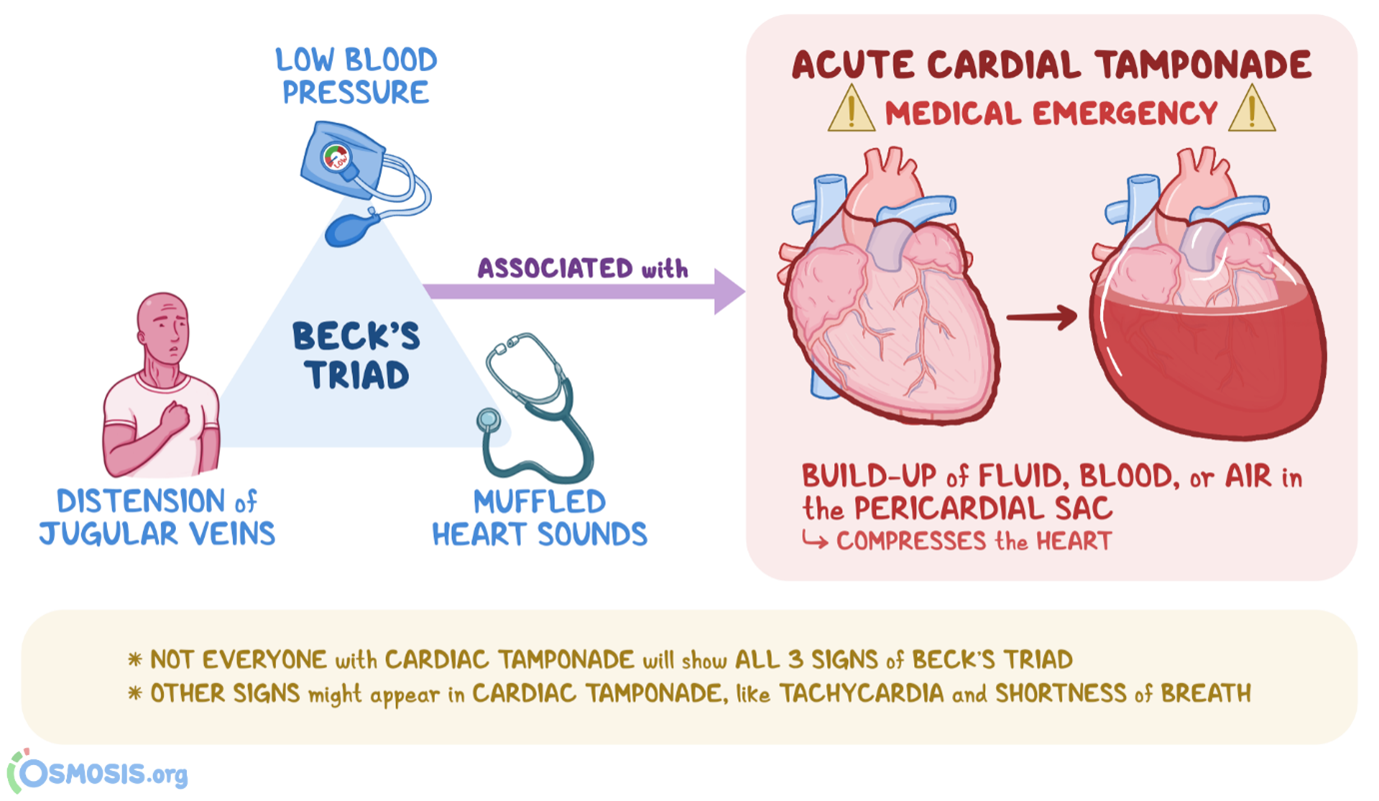
Beck's triad consists of three classic clinical manifestations that are suggestive of cardiac tamponade, which is the compression of the heart by accumulated fluid or blood within the pericardial sac. The three components of Beck's triad include:
A. Muffled heart tones in (option A) are incorrect because Cardiac tamponade can dampen or muffle heart sounds due to the presence of fluid or blood around the heart, which can impair sound transmission.
B. Marked hypotension in (option B) is incorrect because Cardiac tamponade can cause decreased cardiac output, leading to hypotension, which is characterized by low blood pressure.
C. Distended jugular veins in (option C) is incorrect because Elevated venous pressure resulting from impaired filling and elevated right-sided heart pressures can lead to jugular vein distension, which is commonly seen in cardiac tamponade.
However, widening pulse pressure (the difference between systolic and diastolic blood pressure) is not typically part of Beck's triad. Widening pulse pressure is associated with her conditions such as aortic regurgitation, hyperthyroidism, or conditions involving increased stroke volume, rather than cardiac tamponade specifically.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
