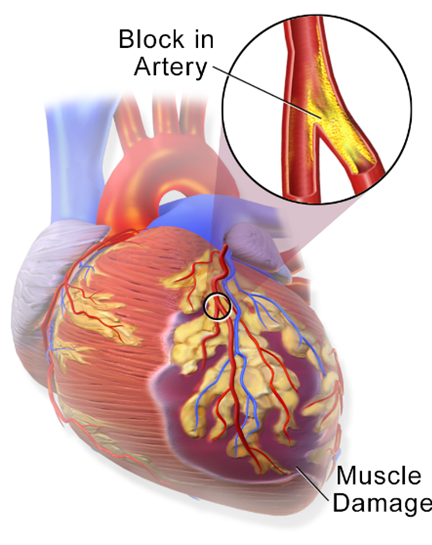
The nurse obtains a monitor strip on a patient who has had a myocardial infarction and makes the following analysis: P wave not apparent, ventricular rate 196, R-R interval regular, P-R interval not measurable, QRS complex wide and distorted, QRS duration 0.18 second. The nurse interprets the patient's cardiac rhythm as;
ventricular tachycardia.
atrial fibrillation.
atrial tachycardia.
ventricular fibrillation.
The Correct Answer is A
The characteristics described in the monitor strip analysis suggest ventricular tachycardia. The absence of a visible P wave and the wide and distorted QRS complex indicates that the electrical impulse is originating in the ventricles rather than the atria. The ventricular rate of 196 and regular R-R intervals further support the diagnosis of ventricular tachycardia.
B. Atrial fibrillation in (option B) is incorrect because it is characterized by irregularly irregular R-R intervals and the absence of discernible P waves. The QRS complex is typically narrow
C. Atrial tachycardia in (option C) is incorrect because it would have a rapid atrial rate with regular R-R intervals, and P waves may or may not be discernible. The QRS complex is typically narrow.
D. Ventricular fibrillation in (option D) is incorrect because it would present as a chaotic, rapid, and irregular electrical activity with no discernible P waves, QRS complexes, or regular R-R intervals. It is a life-threatening emergency that requires immediate defibrillation.
Therefore, based on the provided information, the nurse would interpret the patient's cardiac rhythm as ventricular tachycardia. However, it is important to note that an accurate interpretation should be made by a qualified healthcare professional, and the patient's clinical context should also be considered.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
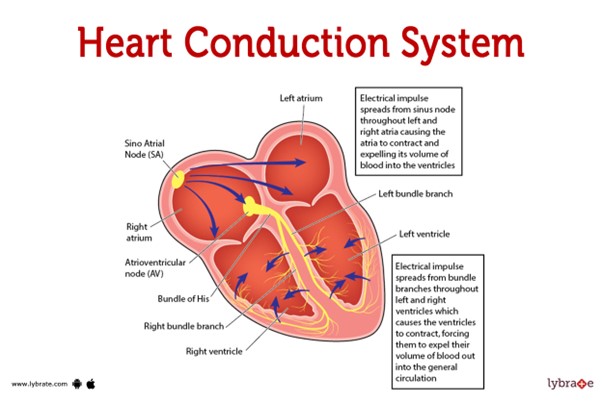 This pathway represents the normal sequence of electrical impulses that coordinate the contraction and relaxation of the heart chambers.
This pathway represents the normal sequence of electrical impulses that coordinate the contraction and relaxation of the heart chambers.
The electrical signal originates from the sinoatrial (SA) node, which is often referred to as the natural pacemaker of the heart. It is located in the right atrium and generates the electrical impulses that initiate each heartbeat. From the SA node, the electrical signal travels to the atrioventricular (AV) node, which is located at the junction between the atria and ventricles.
After passing through the AV node, the electrical impulse travels through the bundle of His (also known as the atrioventricular bundle) and divides into the right and left bundle branches. These branches continue the conduction pathway and deliver the electrical signal to the Purkinje fibers.
The Purkinje fibers spread the electrical impulse rapidly throughout the ventricles, stimulating the contraction of the ventricular muscle and allowing for efficient pumping of blood out of the heart.
Therefore, the correct sequence of the normal conduction pathway in the heart is:
A. SA node - AV node - bundle of His - bundle branches - Purkinje fibers.
Correct Answer is B
Explanation
In this scenario, the patient's signs and symptoms suggest a state of shock, which can be caused by various factors, such as hypovolemia, cardiac dysfunction, or systemic vasodilation. The first priority in managing a patient in shock is to ensure adequate oxygenation and tissue perfusion. Administering oxygen at 100% per non-rebreather mask helps improve oxygen delivery to the tissues and supports vital organ function.
A. Placing the patient on a continuous cardiac monitor in (option A) is incorrect because it is an important step to monitor the patient's heart rhythm and identify any abnormalities. However, providing oxygen should take priority to address the potential hypoxemia and tissue hypoperfusion.
C. Inserting two 14-gauge IV catheters in (option C) is incorrect because it is crucial for establishing large-bore access for fluid resuscitation and medication administration. While it is an important step, addressing oxygenation takes precedence.
D. Drawing blood to type and crossmatch for transfusions in (option D) is incorrect because it is an important step in managing a patient in shock who may require blood products. However, ensuring adequate oxygenation through oxygen administration is the immediate priority.
Therefore, the nurse should act first on the order to administer oxygen at 100% per non-rebreather mask to support the patient's oxygenation and tissue perfusion.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
