A patient who has been involved in a motor vehicle crash arrives in the emergency department (ED) with cool, clammy skin; tachycardia; and hypotension. ordered by the health care provider should the nurse implement first?
Insert two large-bore IV catheters.
Provide oxygen at 100% per non-rebreather mask.
Draw blood to type and crossmatch for transfusions. Initiate continuous
electrocardiogram (ECG) monitoring.
The Correct Answer is B
Cool, clammy skin, tachycardia, and hypotension are signs of shock, indicating inadequate tissue perfusion and oxygenation. The immediate priority is to ensure adequate oxygen delivery to the tissues. Providing oxygen at 100% via a non-rebreather mask helps increase the patient's oxygen saturation and improve tissue oxygenation.
While all the options mentioned are important in the management of a patient in shock, oxygenation takes priority as it directly addresses compromised tissue perfusion and oxygenation.
A. Inserting two large-bore IV catheters in (option A) is incorrect because: Establishing intravenous access is crucial for fluid resuscitation and administration of medications, but it can be done after ensuring adequate oxygenation.
C. Drawing blood to type and crossmatch for transfusions in (option C) is incorrect because Blood typing and crossmatching are important for potential blood transfusions but should not be the first action in this critical situation.
D. Initiating continuous electrocardiogram (ECG) monitoring in (option D) is incorrect because Continuous ECG monitoring is important for assessing cardiac rhythm and detecting any dysrhythmias, but ensuring oxygenation should be the initial priority.
Therefore, in a patient presenting with cool, clammy skin, tachycardia, and hypotension, the nurse should first provide oxygen at 100% via a non-rebreather mask to address inadequate tissue perfusion and oxygenation.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
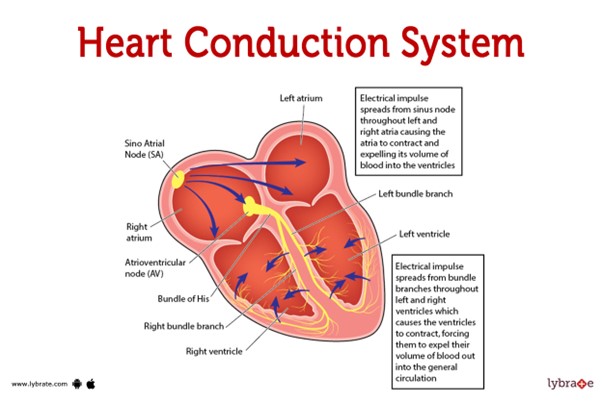 This pathway represents the normal sequence of electrical impulses that coordinate the contraction and relaxation of the heart chambers.
This pathway represents the normal sequence of electrical impulses that coordinate the contraction and relaxation of the heart chambers.
The electrical signal originates from the sinoatrial (SA) node, which is often referred to as the natural pacemaker of the heart. It is located in the right atrium and generates the electrical impulses that initiate each heartbeat. From the SA node, the electrical signal travels to the atrioventricular (AV) node, which is located at the junction between the atria and ventricles.
After passing through the AV node, the electrical impulse travels through the bundle of His (also known as the atrioventricular bundle) and divides into the right and left bundle branches. These branches continue the conduction pathway and deliver the electrical signal to the Purkinje fibers.
The Purkinje fibers spread the electrical impulse rapidly throughout the ventricles, stimulating the contraction of the ventricular muscle and allowing for efficient pumping of blood out of the heart.
Therefore, the correct sequence of the normal conduction pathway in the heart is:
A. SA node - AV node - bundle of His - bundle branches - Purkinje fibers.
Correct Answer is ["9"]
Explanation
-
Doseinmcg/min=2mcg/kg/min×60kg=120mcg/min
Convert this to mg/min since the concentration is in mg:
120mcg/min=0.12mg/min120 \text{ mcg/min} = 0.12 \text{ mg/min}120mcg/min=0.12mg/min
-
Determine the concentration of Dopamine:
- Total amount of Dopamine: 200 mg in 250 mL of saline
- Concentration:
Concentration=200mg250mL=0.8mg/mL\text{Concentration} = \frac{200 \text{ mg}}{250 \text{ mL}} = 0.8 \text{ mg/mL}Concentration=250mL200mg=0.8mg/mL
-
Calculate the pump rate in mL/min:
To find the rate in mL/min needed to deliver 0.12 mg/min:
Pumprate=Desireddose(mg/min)Concentration(mg/mL)\text{Pump rate} = \frac{\text{Desired dose (mg/min)}}{\text{Concentration (mg/mL)}}Pumprate=Concentration(mg/mL)Desireddose(mg/min)
Pumprate=0.12mg/min0.8mg/mL=0.15mL/min\text{Pump rate} = \frac{0.12 \text{ mg/min}}{0.8 \text{ mg/mL}} = 0.15 \text{ mL/min}Pumprate=0.8mg/mL0.12mg/min=0.15mL/min
-
Convert the pump rate to mL/hour:
Multiply by 60 to convert from mL/min to mL/hour:
Pumprate=0.15mL/min×60min/hour=9mL/hour\text{Pump rate} = 0.15 \text{ mL/min} \times 60 \text{ min/hour} = 9 \text{ mL/hour}Pumprate=0.15mL/min×60min/hour=9mL/hour
So, you should set the pump to deliver Dopamine at a rate of 9 mL/hour.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
