The ICU nurse provides care for a 67-year-old female patient experiencing a distributive shock. Assessment findings are indicative of decreasing cardiac output, decreased peripheral perfusion, and increased capillary permeability. The nurse identifies that the patient is in which stage of shock.
Progressive stage
Compensatory stage
Initial stage
Refractory stage
The Correct Answer is A
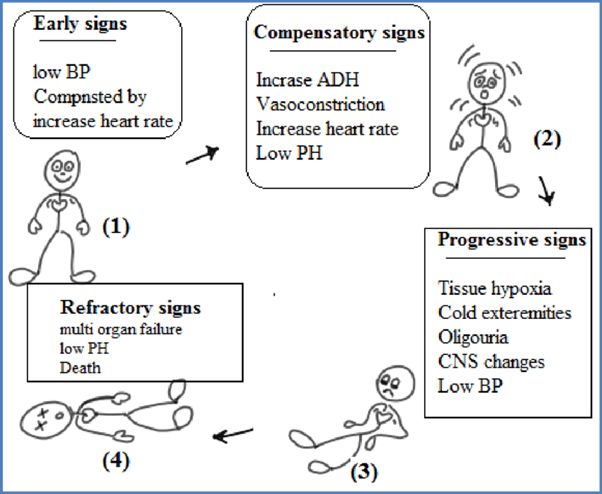
The stages of shock are commonly described as the initial, compensatory, progressive, and refractory stages. Here is an explanation of each stage and why the patient's assessment findings correspond to the progressive stage:
B. The compensatory stage in (option B) is incorrect because, In the compensatory stage, the body continues to activate compensatory mechanisms to maintain perfusion. This includes increased heart rate, peripheral vasoconstriction, and shunting of blood to vital organs. The patient's assessment findings of decreasing cardiac output, decreased peripheral perfusion, and increased capillary permeability suggest that the body's compensatory mechanisms are no longer sufficient to maintain perfusion adequately. Therefore, the patient has progressed beyond the compensatory stage.
C. The initial stage in (option C) is incorrect because, In the initial stage, there is an initial insult or injury that triggers the shock state. The body's compensatory mechanisms are activated, such as increased heart rate and vasoconstriction, to maintain blood pressure and perfusion. However, the patient's assessment findings indicate that they have progressed beyond the initial stage.
D. The refractory stage in (option D) is incorrect because The refractory stage represents a severe and irreversible state of shock where vital organs fail, and despite interventions, the patient's condition does not improve. The patient's assessment findings do not suggest the refractory stage, as there is still potential for intervention and management.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
Cool, clammy skin, tachycardia, and hypotension are signs of shock, indicating inadequate tissue perfusion and oxygenation. The immediate priority is to ensure adequate oxygen delivery to the tissues. Providing oxygen at 100% via a non-rebreather mask helps increase the patient's oxygen saturation and improve tissue oxygenation.
While all the options mentioned are important in the management of a patient in shock, oxygenation takes priority as it directly addresses compromised tissue perfusion and oxygenation.
A. Inserting two large-bore IV catheters in (option A) is incorrect because: Establishing intravenous access is crucial for fluid resuscitation and administration of medications, but it can be done after ensuring adequate oxygenation.
C. Drawing blood to type and crossmatch for transfusions in (option C) is incorrect because Blood typing and crossmatching are important for potential blood transfusions but should not be the first action in this critical situation.
D. Initiating continuous electrocardiogram (ECG) monitoring in (option D) is incorrect because Continuous ECG monitoring is important for assessing cardiac rhythm and detecting any dysrhythmias, but ensuring oxygenation should be the initial priority.
Therefore, in a patient presenting with cool, clammy skin, tachycardia, and hypotension, the nurse should first provide oxygen at 100% via a non-rebreather mask to address inadequate tissue perfusion and oxygenation.
Correct Answer is B
Explanation
Mean arterial pressure (MAP) is a measure of the average pressure within the arteries during one cardiac cycle. It represents the perfusion pressure that drives blood flow to organs and tissues. MAP is calculated using the formula:
MAP = Diastolic blood pressure + 1/3 (Systolic blood pressure - Diastolic blood pressure)
Blood loss, particularly in cases of significant hemorrhage, leads to a decrease in blood volume. When blood volume decreases, there is less circulating blood available to generate pressure within the arterial system. This reduction in blood volume results in decreased MAP.
Therefore, in the case of massive blood loss after trauma, the student can correlate it with a lower blood volume, which in turn leads to a lower MAP. The decrease in blood volume reduces the perfusion pressure, compromising organ and tissue perfusion
A. It causes vasoconstriction and increased MAP in (option A) is incorrect because: While vasoconstriction can occur as a compensatory mechanism to maintain blood pressure, it does not necessarily lead to an increased MAP in the context of significant blood loss.
C. It raises cardiac output and MAP in (option C) is incorrect because Blood loss typically leads to a reduction in cardiac output due to decreased blood volume. Therefore, it does not raise cardiac output and MAP.
D. There is no direct correlation to MAP in (option D) is incorrect because: There is indeed a direct correlation between blood loss and MAP. As blood volume decreases, MAP decreases as well.
Therefore, the correct correlation between blood loss and MAP is that lower blood volume lowers MAP.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
