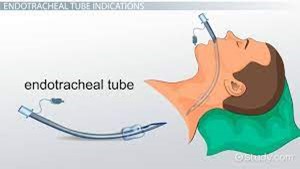
To verify the correct placement of an endotracheal tube (ET) after insertion, the best initial action by the nurse is to:
auscultate for the presence of bilateral breath sounds.
Use an end-tidal C02 monitor to check for placement in the trachea.
Observe the chest for symmetrical movement with ventilation.
Obtain a portable chest radiograph to check tube placement.
None
None
The Correct Answer is B
A. Auscultate for the presence of bilateral breath sounds.
It's an important check, but it is not the most reliable initial method because breath sounds can sometimes be misleading (for example, sounds may be heard in the stomach or transmitted incorrectly).
B. Use an end-tidal CO₂ monitor to check for placement in the trachea.
It's the correct answer. Continuous waveform capnography or end-tidal CO₂ detection is the most reliable and immediate method to confirm that the endotracheal tube is in the trachea and not in the esophagus. Presence of CO₂ indicates effective airway placement.
C. Observe the chest for symmetrical movement with ventilation.
Chest rise is helpful, but it is not specific both esophageal and tracheal intubation may show chest movement.
D. Obtain a portable chest radiograph to check tube placement.
It's the gold standard for final confirmation, but it is not the initial bedside method because it takes time.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is D
Explanation
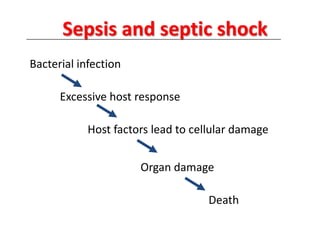
Septic shock is a life-threatening condition characterized by severe infection, systemic inflammation, and inadequate tissue perfusion. Hypotension, as indicated by a low blood pressure reading, is a significant concern in septic shock. It reflects inadequate perfusion to vital organs and tissues, leading to potential organ dysfunction and damage.
While all the assessment data provided may be important and require attention, the low blood pressure (BP) reading indicates impaired systemic perfusion and can contribute to end-organ damage. The nurse should prioritize interventions aimed at improving perfusion and stabilizing the patient's blood pressure.
A. Arterial oxygen saturation is 90% in (option A) is incorrect because While an arterial oxygen saturation of 90% is below the desired range, it is not as immediately life-threatening as low blood pressure. Oxygen therapy and interventions to improve oxygenation should still be initiated, but addressing hypotension takes priority.
B. Urine output of 15 ml for 2 hours in (option B) is incorrect because Decreased urine output is a concerning sign, as it may indicate impaired renal perfusion. However, the immediate concern in septic shock is addressing the low blood pressure to improve overall perfusion, including renal perfusion.
C. Apical pulse 110 beats/min in (option C) is incorrect because: Tachycardia is a common finding in septic shock and represents the body's compensatory response to maintain cardiac output. While it requires monitoring and consideration, low blood pressure is a more significant concern.
Correct Answer is D
Explanation
Arterial pressure monitoring involves the insertion of an arterial catheter, typically in the radial artery, to directly measure blood pressure. Complications can arise from this invasive procedure, and one potential complication is inadequate blood flow to the hand, leading to numbness or ischemia.
A. The Allen's test is positive in (option A) is incorrect because The Allen's test is performed before arterial catheter insertion to assess the collateral circulation of the hand. A positive Allen test indicates adequate collateral circulation, which is desirable before performing the procedure. However, it does not directly indicate a complication during or after arterial pressure monitoring.
B. The mean arterial pressure (MAP) is 90 mm Hg in (option B) is incorrect because The mean arterial pressure (MAP) represents the average pressure in the arterial system during one cardiac cycle. While changes in MAP can be significant for patient management, it does not specifically indicate a complication of arterial pressure monitoring.
C. The dicrotic notch visible in the waveform in (option C) is incorrect because The dicrotic notch represents the closure of the aortic valve and is a normal finding in arterial waveforms. Its presence does not indicate a complication.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
