A 48-year-old female patient with septic shock presents with a BP of 70/46, pulse 136, respirations 32, temperature 104.0° F, and blood glucose of 246 mg/dl. The following have been ordered. Which order will the nurse accomplish first?
Draw an arterial blood gas (ABG).
Start insulin drip to maintain blood glucose at 150 mg/dl or lower.
Give a normal saline bolus IV of 30mL/kg.
Titrate norepinephrine (Levophed) to keep MAP greater than 65 mm Hg.
The Correct Answer is C
Septic shock is characterized by inadequate tissue perfusion and hypotension, which can lead to organ dysfunction and failure. The administration of intravenous fluids, such as a normal saline bolus, is the initial priority in the management of septic shock to restore intravascular volume and improve perfusion.
A. Draw an arterial blood gas (ABG) in (option A) is incorrect because: ABG may be ordered to assess the patient's acid-base status and oxygenation, but addressing hypotension and restoring perfusion through fluid administration takes priority.
B. Start insulin drip to maintain blood glucose at 150 mg/dl or lower in (option B) is incorrect because: Hyperglycaemia is commonly observed in critically ill patients, including those with septic shock. While controlling blood glucose is important, it is not the immediate priority compared to addressing hypotension and restoring intravascular volume.
D. Titrate norepinephrine (Levophed) to keep mean arterial pressure (MAP) greater than 65 mm Hg in (option D) is incorrect because: Norepinephrine is a vasopressor medication used to increase blood pressure and perfusion in septic shock. While it may be necessary for the management of septic shock, fluid resuscitation should be initiated first to optimize intravascular volume before starting vasopressors.
Therefore, the first order that the nurse should accomplish in this scenario is to give a normal saline bolus IV of 30 mL/kg to address the hypotension and restore intravascular volume.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A,B,D,C
Explanation
A. Decreased blood volume: Burn injuries can lead to fluid loss, primarily through damaged skin. This fluid loss causes a decrease in blood volume, leading to hypovolemia. Hypovolemia contributes to decreased cardiac output and tissue perfusion.
B. Increased vascular permeability: Burn injuries cause an inflammatory response, leading to increased vascular permeability. This increased permeability allows fluid, electrolytes, and proteins to leak from the intravascular space into the interstitial space.
C. Development of edema: The increased vascular permeability and fluid leakage lead to the development of edema. Edema occurs as fluid accumulates in the interstitial spaces, further contributing to tissue swelling and compromised perfusion.
D. Increased peripheral resistance: In response to decreased blood volume and tissue hypoperfusion, the body activates compensatory mechanisms to maintain blood pressure and tissue perfusion. One of these mechanisms is increased peripheral resistance, which occurs as blood vessels constrict to maintain blood pressure. Increased peripheral resistance helps redirect blood flow to vital organs but also contributes to increased workload on the heart.
Therefore, the correct sequential order of events involved in burn shock following a patient's exposure to burns is:
A. Decreased blood volume B. Increased vascular permeability D. Development of edema C. Increased peripheral resistance
Correct Answer is A
Explanation
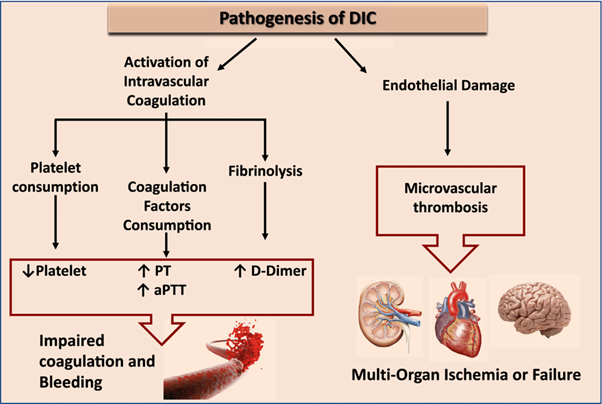
Disseminated intravascular coagulation (DIC) is a condition characterized by both widespread activation of the coagulation system and excessive clotting, leading to the consumption of clotting factors and platelets. This results in a prothrombotic state, which can lead to organ dysfunction and bleeding manifestations.
Elevated D-dimer levels are a characteristic finding in DIC. D-dimer is a fibrin degradation product that is elevated when there is excessive fibrin formation and breakdown. Elevated D-dimer indicates ongoing fibrinolysis and activation of the clotting system.
B. Decreased prothrombin time in (option B) is incorrect because: DIC is characterized by consumption of clotting factors, which can result in prolongation of the prothrombin time (PT) as well as other coagulation tests.
C. Decreased partial thromboplastin time in (option C) is incorrect because Similar to the prothrombin time, the partial thromboplastin time (PTT) can also be prolonged in DIC due to the consumption of clotting factors.
D. Elevated fibrinogen level in (option D) is incorrect because, In DIC, there is consumption of fibrinogen along with other clotting factors. Therefore, elevated fibrinogen levels are not consistent with the pathophysiology of DIC.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
