The cardiac ICU nurse is assessing a patient who is in cardiogenic shock. Which hemodynamic manifestations and/or signs and symptoms do the nurse expect? Select all that apply.
Narrowed pulse pressure.
Tachycardia.
Elevated SBP.
Pulmonary congestion.
Pulmonary artery wedge pressure
Correct Answer : A,B,D,E
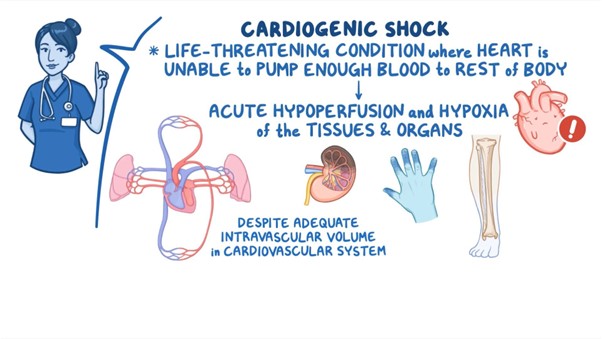
A. Narrowed pulse pressure: In cardiogenic shock, the cardiac output is compromised, resulting in reduced stroke volume and subsequent narrowed pulse pressure. The pulse pressure is the difference between systolic and diastolic blood pressure.
B. Tachycardia: Tachycardia is a compensatory response in cardiogenic shock, as the body attempts to increase cardiac output to maintain tissue perfusion despite decreased stroke volume. Increased heart rate is a common finding in this condition.
D. Pulmonary congestion: Cardiogenic shock is often associated with impaired left ventricular function, leading to an inadequate pump mechanism. This can result in fluid accumulation and congestion in the pulmonary circulation, leading to pulmonary edema and congestion. Patients may experience symptoms such as dyspnea, crackles on lung auscultation, and increased work of breathing.
E. Elevated pulmonary artery wedge pressure (PAWP): PAWP is a measurement obtained during invasive hemodynamic monitoring. In cardiogenic shock, the impaired left ventricular function leads to increased left atrial pressure, which is reflected by an elevated PAWP. Elevated PAWP indicates increased fluid volume and congestion in the left side of the heart.
C. Elevated SBP in (option C) is incorrect because Elevated systolic blood pressure (SBP) is not a typical finding in cardiogenic shock. Instead, hypotension or decreased blood pressure is commonly observed due to reduced cardiac output.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is D
Explanation
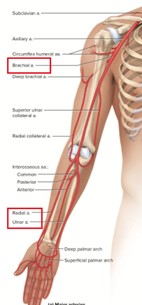
When the low-pressure alarm sounds, it indicates that the pressure being detected by the arterial line is below the set threshold. This could be due to a variety of reasons, such as a loose connection, air bubbles, or a shift in the zero-reference point.
Rezeroing the monitoring equipment involves recalibrating or resetting the baseline reference point for the arterial pressure waveform. This ensures accurate measurement and monitoring of the patient's arterial pressure.
A. Checking the right hand for a rash in (option A) is incorrect because While assessing the patient for any skin changes or rashes is important, it is not the first action to take in response to a low-pressure alarm.
B. Assessing the waveform for under-dampening in (option B) is incorrect because Assessing the waveform characteristics is important in arterial line monitoring, but it may not be the initial action when the low-pressure alarm sounds. Rezeroing the equipment should be performed before assessing waveform characteristics.
C. Assessing for cardiac dysrhythmias in (option C) is incorrect because Assessing for dysrhythmias is an important aspect of patient care, but it may not be directly related to the low-pressure alarm from the arterial line. Rezeroing the monitoring equipment takes precedence.
Therefore, when the low-pressure alarm sounds for a patient with an arterial line, the nurse should first re-zero the monitoring equipment to ensure accurate measurement of arterial pressure.
Correct Answer is D
Explanation
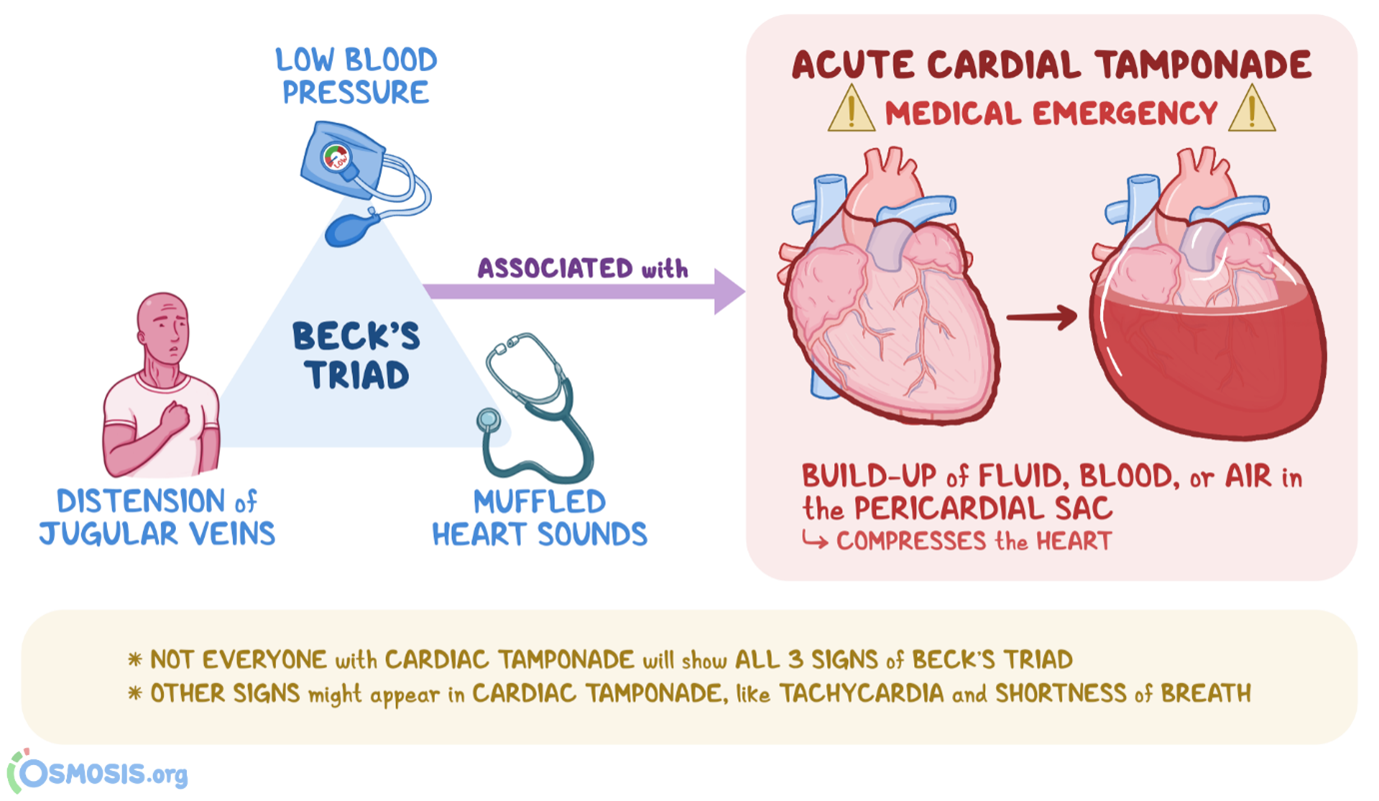
Beck's triad consists of three classic clinical manifestations that are suggestive of cardiac tamponade, which is the compression of the heart by accumulated fluid or blood within the pericardial sac. The three components of Beck's triad include:
A. Muffled heart tones in (option A) are incorrect because Cardiac tamponade can dampen or muffle heart sounds due to the presence of fluid or blood around the heart, which can impair sound transmission.
B. Marked hypotension in (option B) is incorrect because Cardiac tamponade can cause decreased cardiac output, leading to hypotension, which is characterized by low blood pressure.
C. Distended jugular veins in (option C) is incorrect because Elevated venous pressure resulting from impaired filling and elevated right-sided heart pressures can lead to jugular vein distension, which is commonly seen in cardiac tamponade.
However, widening pulse pressure (the difference between systolic and diastolic blood pressure) is not typically part of Beck's triad. Widening pulse pressure is associated with her conditions such as aortic regurgitation, hyperthyroidism, or conditions involving increased stroke volume, rather than cardiac tamponade specifically.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
