The emergency department nurse provides care for a 50-year-old male patient with septic shock. The nurse recalls that the renin- angiotensin system is activated during which stage of shock?
Initial stage
Progressive stage
Refractory stage
Compensatory stage
The Correct Answer is D
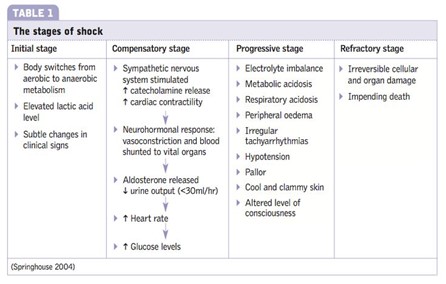
In the compensatory stage of shock, the body initiates various mechanisms to maintain perfusion to vital organs and restore homeostasis. Activation of the renin-angiotensin system is one of the compensatory responses. The decreased blood flow and oxygen delivery to the kidneys stimulate the release of renin from the kidneys. Renin acts on angiotensinogen, converting it into angiotensin I, which is further converted to angiotensin II by the action of angiotensin-converting enzyme (ACE). Angiotensin II is a potent vasoconstrictor and also stimulates the release of aldosterone, leading to sodium and water retention. These mechanisms aim to increase blood pressure and cardiac output and restore fluid balance.
A. The initial stage of shock in (option A) is incorrect because it is characterized by inadequate tissue perfusion and the activation of various compensatory mechanisms, including the release of stress hormones. However, the renin-angiotensin system is not specifically mentioned as activated in this stage.
B. The progressive stage of shock in (option B) is incorrect because it occurs when compensatory mechanisms fail to maintain adequate perfusion, leading to worsening hypoperfusion and organ dysfunction. The renin-angiotensin system continues to be activated during this stage, but it is primarily associated with the compensatory stage.
C. The refractory stage of shock in (option C) is incorrect because it is the stage of severe and prolonged hypoperfusion, where organ failure becomes irreversible. The renin-angiotensin system may still be activated, but it is not the primary focus of this stage.
Therefore, the activation of the renin-angiotensin system occurs during the compensatory stage of shock.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is C
Explanation
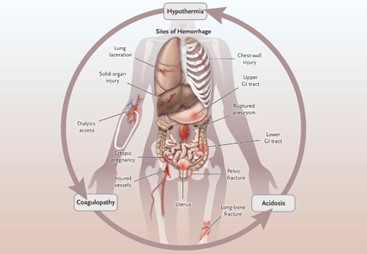
Hemorrhagic shock is characterized by severe blood loss, leading to inadequate tissue perfusion and hypovolemia. The primary goal in the initial management of hemorrhagic shock is to restore intravascular volume and improve tissue perfusion. Administering intravenous fluids, such as normal saline solution, is a critical intervention to address hypovolemia and improve blood pressure.
A. Give Plasmanate 1 unit now in (option A) is incorrect because: Plasmanate is a plasma-derived product used to replace coagulation factors. While it may be necessary to address coagulation abnormalities, administering intravenous fluids to restore volume takes priority over specific blood products.
B. Prepare for endotracheal intubation in (option B) is incorrect because Endotracheal intubation may be required in cases of impending respiratory failure or compromised airway, but it should not be the first action in addressing hypovolemic shock.
D. Type and crossmatch for 4 units of packed red blood cells (PRBCs) in (option D) is incorrect because transferring packed red blood cells is an important intervention to address blood loss and improve oxygen-carrying capacity. However, before administering blood products, it is crucial to stabilize the patient's hemodynamics through fluid resuscitation.
Therefore, in a patient with hemorrhagic shock, the nurse's first priority among the given options is to give normal saline solution of 250 mL/hr to restore intravascular volume and improve tissue perfusion.
Correct Answer is B
Explanation
Lactate is a by-product of anaerobic metabolism that accumulates when there is insufficient oxygen supply to meet cellular metabolic demands. In the context of severe tissue hypoxia, such as in septic shock, the body may resort to anaerobic metabolism, leading to increased lactate production and elevated lactate levels in the blood.
Elevated lactate levels, typically above 4.0 mmol/L, are indicative of tissue hypoxia and inadequate oxygenation at the cellular level. Higher lactate levels, such as 9.0 mmol/L, suggest more severe tissue hypoxia and increased anaerobic metabolism.
A. Partial thromboplastin time (PTT) 64 seconds in (option A) is incorrect because: PTT is a laboratory test that evaluates the intrinsic pathway of the coagulation cascade. While coagulation abnormalities may occur in septic shock, PTT alone does not specifically indicate severe tissue hypoxia.
C. Potassium 2.8 mEq/L (2.8 mmol/L) (option C) is incorrect because Low potassium levels (hypokalemia) can be a concern in septic shock, but it does not directly indicate severe tissue hypoxia.
D. PaCO2 58 mm Hg in (option D) is incorrect because: PaCO2 refers to the partial pressure of carbon dioxide in arterial blood and is a measure of the respiratory status. While an elevated PaCO2 can be a sign of respiratory acidosis, it is not specific to severe tissue hypoxia.
Therefore, in a critically ill patient with septic shock, an elevated lactate level, such as 9.0 mmol/L, indicates severe tissue hypoxia and inadequate oxygenation at the cellular level
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
