The ICU charge nurse will evaluate that teaching about hemodynamic monitoring for a new staff nurse has been effective when the new nurse does which of the following?
Position the limb with the catheter insertion site at the level of the transducer.
Positions the transducer level with the phlebostatic axis.
Ensures that the patient is lying with the head of the bed flat for all readings.
Balances and calibrates the hemodynamic monitoring equipment every hour.
The Correct Answer is B
Positioning the transducer level with the phlebostatic axis is a crucial step in accurate hemodynamic monitoring. The phlebostatic axis is an imaginary reference point located at the fourth intercostal space, mid-anterior/posterior chest. Placing the transducer at this level ensures that the pressure measurements obtained are reflective of the patient's true hemodynamic status.
A. Positioning the limb with the catheter insertion site at the level of the transducer in (option A) is incorrect because: While it is important to position the limb appropriately to avoid kinks or occlusions in the catheter tubing, this is not directly related to the accurate measurement of hemodynamic parameters.
C. Ensuring that the patient is lying with the head of the bed flat for all readings in (option C) is incorrect because The position of the patient's head does not directly impact the accuracy of hemodynamic monitoring unless it specifically relates to changes in preload or intracranial pressure monitoring.
D. Balancing and calibrating the hemodynamic monitoring equipment every hour in (option D) is incorrect because: While it is important to ensure that the monitoring equipment is calibrated and functioning properly, doing so every hour may not be necessary. Calibration frequency may vary based on institutional policies and patient stability.
Therefore, the correct action that demonstrates effective teaching about hemodynamic monitoring is positioning the transducer level with the phlebostatic axis.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is D
Explanation
The absence of palpable pulses suggests a lack of effective cardiac output, and the patient is in cardiac arrest. In this situation, immediate initiation of cardiopulmonary resuscitation (CPR) is crucial to maintain circulation and provide oxygenation to vital organs.
CPR consists of chest compressions and rescue breaths to circulate oxygenated blood to the brain and other vital organs. It is the primary intervention in cardiac arrest to provide temporary life support until advanced cardiac life support (ACLS) measures, such as defibrillation or medication administration, can be initiated.
A. Administering the prescribed Beta-Blocker in (option A) is incorrect because Administering a beta-blocker is not the initial action in a patient who is in cardiac arrest and requires immediate resuscitation.
B. Prepare for Cardioversion per hospital protocol (option B) is incorrect because Cardioversion, which is the delivery of an electric shock to the heart, may be considered in certain situations like unstable ventricular tachycardia or certain supraventricular tachycardias. However, in the given scenario, the patient is unresponsive and has no pulses, indicating cardiac arrest where CPR takes precedence over cardioversion.
C. Give 100% oxygen per non-rebreather mask in (option C) is incorrect because: While oxygenation is important, it should not delay or replace the initiation of CPR, which is the immediate priority in a patient without palpable pulses.
Therefore, the first action that the nurse should take in this scenario is to start CPR.
Correct Answer is A
Explanation
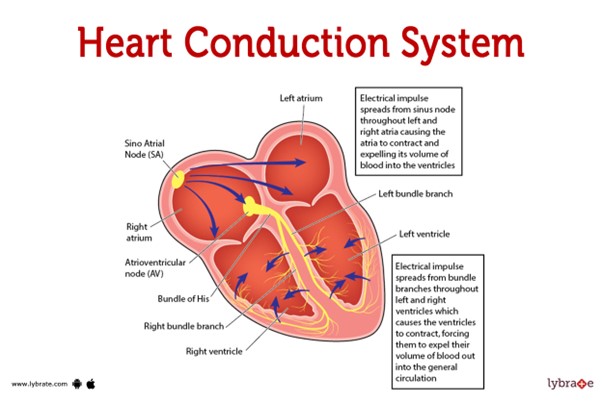 This pathway represents the normal sequence of electrical impulses that coordinate the contraction and relaxation of the heart chambers.
This pathway represents the normal sequence of electrical impulses that coordinate the contraction and relaxation of the heart chambers.
The electrical signal originates from the sinoatrial (SA) node, which is often referred to as the natural pacemaker of the heart. It is located in the right atrium and generates the electrical impulses that initiate each heartbeat. From the SA node, the electrical signal travels to the atrioventricular (AV) node, which is located at the junction between the atria and ventricles.
After passing through the AV node, the electrical impulse travels through the bundle of His (also known as the atrioventricular bundle) and divides into the right and left bundle branches. These branches continue the conduction pathway and deliver the electrical signal to the Purkinje fibers.
The Purkinje fibers spread the electrical impulse rapidly throughout the ventricles, stimulating the contraction of the ventricular muscle and allowing for efficient pumping of blood out of the heart.
Therefore, the correct sequence of the normal conduction pathway in the heart is:
A. SA node - AV node - bundle of His - bundle branches - Purkinje fibers.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
