Which of the following clinical manifestations of Disseminated intravascular coagulation (DIC)?
Decreased hematocrit, increased platelet counts, increased D-dimer
Decreased platelet counts, increased D-dimer, increased prothrombin time
Decreased Antithrombin III, increased platelet counts, increased fibrinogen
Decreased D-dimer, increased platelet counts, Increased hemoglobin
The Correct Answer is B
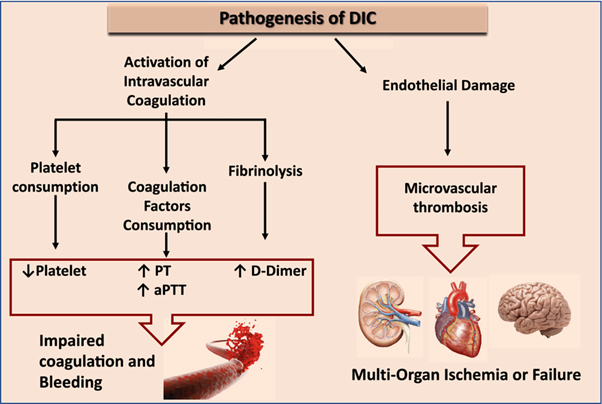
Disseminated Intravascular Coagulation (DIC) is a condition characterized by widespread activation of the coagulation system, leading to both excessive clot formation and consumption of clotting factors and platelets. This process can result in both bleeding and thrombosis.
The manifestations mentioned in option B are commonly seen in DIC:
Decreased platelet counts: DIC leads to platelet consumption and destruction, resulting in low platelet counts (thrombocytopenia).
Increased D-dimer: D-dimer is a fibrin degradation product, and its levels are increased DIC due to the breakdown of fibrin clots.
Increased prothrombin time (PT): DIC can lead to the depletion of clotting factors, resulting in prolonged prothrombin time, indicating impaired coagulation.
The other options mentioned do not represent the typical clinical manifestations of DIC:
A. Decreased hematocrit, increased platelet counts, and increased D-dimer in (option A) are incorrect because While platelet counts and D-dimer are increased in DIC, decreased hematocrit is not a characteristic finding.
C. Decreased Antithrombin III, increased platelet counts, and increased fibrinogen in (option C) is incorrect because: Decreased Antithrombin III can be seen in DIC, but increased platelet counts and fibrinogen levels are not specific to DIC.
D. Decreased D-dimer, increased platelet counts, and increased hemoglobin in (option D) is incorrect because Decreased D-dimer and increased hemoglobin are not typical findings in DIC, while increased platelet counts can be seen in some cases.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is D
Explanation
Norepinephrine is a vasopressor medication commonly used in the management of septic shock. It acts as a potent vasoconstrictor to increase systemic vascular resistance and improve blood pressure. By constricting blood vessels, norepinephrine helps restore tissue perfusion and improve organ function.
A. Nitroglycerine (Tridil) in (option A) is incorrect because: Nitroglycerine is a vasodilator and would further lower blood pressure. It is not suitable for a patient with septic shock who already has low blood pressure.
B. Atenolol (Tenormin) in (option B) is incorrect because: Atenolol is a beta-blocker and would further decrease heart rate and blood pressure. It is not appropriate for a patient in septic shock who requires intervention to increase blood pressure.
C. Dobutamine (Dobutrex) in (option C) is incorrect because: Dobutamine is an inotropic medication used to increase cardiac output. While it can be helpful in certain types of shock, such as cardiogenic shock, it is not the first-line choice for septic shock when there is inadequate blood pressure response.
Correct Answer is B
Explanation
Assessing the patient's level of consciousness is a critical initial step in evaluating a patient with shock. Altered mental status or decreased level of consciousness can be indicative of inadequate cerebral perfusion and may require immediate interventions to address compromised brain function and ensure patient safety.
While all the options mentioned are important in the assessment and management of a patient in shock, checking the level of consciousness takes priority as it provides essential information about the patient's neurological status and helps guide further interventions.
A. Obtaining the blood pressure in (option A) is incorrect because Assessing blood pressure is crucial in evaluating a patient in shock, but it can be done in conjunction with checking the level of consciousness and other vital signs.
C. Administering oxygen in (option C) is incorrect because: Administering oxygen is important in managing shock, as tissue hypoxia is a key concern. However, it can be done simultaneously with assessing the level of consciousness and initiating other interventions.
D. Obtaining a 12-lead electrocardiogram (ECG) in (option D) is incorrect because While an ECG may provide valuable information about the patient's cardiac function, it is not the first priority in a patient with shock of unknown etiology. Assessing the level of consciousness and vital signs takes precedence.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
