Which of the following would be essential to implement to prevent late postpartum hemorrhage? Select one:
Inspecting the placenta after delivery for intactness.
Manually removing the placenta at delivery.
Administering broad-spectrum antibiotics prophylactically.
Applying traction on the umbilical cord to speed up separation of the placenta.
The Correct Answer is A
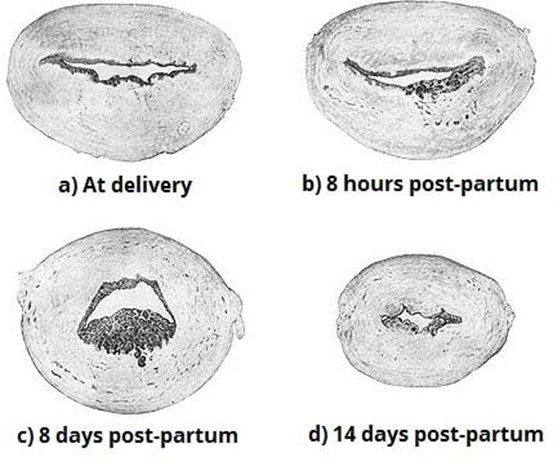
Choice A Reason: Inspecting the placenta after delivery for intactness. This is because inspecting the placenta after delivery for intactness is a nursing intervention that can prevent late postpartum hemorrhage, which is excessive bleeding from the uterus or genital tract that occurs more than 24 hours but less than 12 weeks after delivery. Late postpartum hemorrhage can be caused by retained placental fragments, subinvolution of the uterus, infection, or coagulation disorders. Inspecting the placenta after delivery for intactness can help identify and remove any retained placental fragments that may interfere with uterine contraction and involution, which are essential for hemostasis.
Choice B Reason: Manually removing the placenta at delivery. This is an incorrect answer that indicates an inappropriate and risky intervention that can cause late postpartum hemorrhage. Manually removing the placenta at delivery is a procedure that involves inserting a hand into the uterus and detaching the placenta from the uterine wall. Manually removing the placenta at delivery is indicated only for a retained or adherent placenta that does not separate spontaneously or with gentle traction within 30 minutes after delivery. Manually removing the placenta at delivery can cause trauma, infection, or incomplete removal of the placenta, which can increase the risk of late postpartum hemorrhage.
Choice C Reason: Administering broad-spectrum antibiotics prophylactically. This is an incorrect answer that suggests an unnecessary and ineffective intervention that can prevent late postpartum hemorrhage. Administering broad- spectrum antibiotics prophylactically is a pharmacological intervention that involves giving antibiotics to prevent or treat infection. Administering broad-spectrum antibiotics prophylactically is indicated for women with risk factors or signs of infection during or after delivery, such as prolonged rupture of membranes, chorioamnionitis, fever, or foul- smelling lochia. Administering broad-spectrum antibiotics prophylactically may reduce the risk of infection-related late postpartum hemorrhage, but it does not address other causes of late postpartum hemorrhage such as retained placental fragments or subinvolution of the uterus.
Choice D Reason: Applying traction on the umbilical cord to speed up separation of the placenta. This is an incorrect answer that refers to a different intervention that can prevent early postpartum hemorrhage, not late postpartum hemorrhage. Applying traction on the umbilical cord to speed up separation of the placenta is a technique that involves pulling on the umbilical cord while applying counter pressure on the uterus to facilitate placental expulsion. Applying traction on the umbilical cord to speed up separation of the placenta is indicated for active management of the third stage of labor, which can prevent early postpartum hemorrhage, which is excessive bleeding from the uterus or genital tract that occurs within 24 hours after delivery. Early postpartum hemorrhage can be caused by uterine atony, retained placenta, lacerations, or coagulation disorders.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
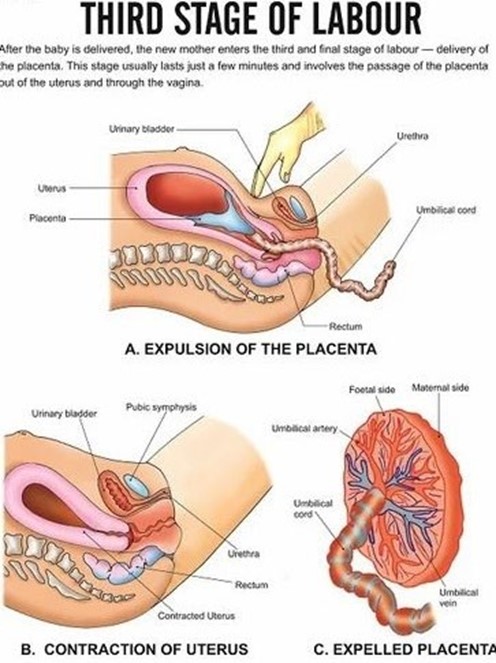
Choice A Reason: Assisting with the delivery of the placenta and ensuring that the fundus is contracted afterward. This is an appropriate action for the nurse to perform during the third stage of labor, as it helps complete the process of labor and prevent complications.
Choice B Reason: Palpating the woman's fundus for position and firmness. This is an action that is done after the delivery of the placenta, not during. It is important to monitor the fundal height, location, and consistency to assess uterine involution and bleeding.
Choice C Reason: Encouraging the woman to push with her contractions. This is an action that is done during the second stage of labor, not the third. The second stage of labor is the period from full cervical dilation to the birth of the baby. The nurse's role is to support and coach the woman to push effectively with her contractions.
Choice D Reason: Alleviating perineal discomfort with the application of ice packs. This is an action that is done after the delivery of the placenta, not during. It is a comfort measure that can reduce swelling, pain, and inflammation in the perineal area.
Correct Answer is A
Explanation
Choice A Reason: Docusate sodium (Colace). This is because docusate sodium is a stool softener that can prevent constipation and straining during defecation, which can aggravate or impair the healing of a perineal laceration. A fourth-degree perineal laceration is a severe tear that extends through the skin, muscles, perineal body, and anal sphincter into the rectal mucosa. It can occur during vaginal delivery due to factors such as fetal macrosomia, forceps use, or episiotomy.
Choice B Reason: Bromocriptine (Parlodel). This is an inappropriate medication for a postpartum client with a fourth- degree perineal laceration, as it has no effect on wound healing or pain relief. Bromocriptine is a dopamine agonist that can suppress lactation by inhibiting prolactin secretion. It is used for women who do not wish to breastfeed or who have medical contraindications to breastfeeding.
Choice C Reason: Ferrous sulfate (Feosol). This is an unnecessary medication for a postpartum client with a fourth- degree perineal laceration, unless she has iron deficiency anemia. Ferrous sulfate is an iron supplement that can treat or prevent anemia by increasing hemoglobin production and oxygen-carrying capacity. Anemia can occur in the postpartum period due to blood loss during delivery or poor nutritional intake during pregnancy.
Choice D Reason: Methylergonovine (Methergine). This is an irrelevant medication for a postpartum client with a fourth-degree perineal laceration, as it does not affect wound healing or pain relief. Methylergonovine is an ergot alkaloid that can stimulate uterine contractions and reduce postpartum bleeding. It is used for women who have uterine atony or hemorrhage.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
