A patient develops increasing dyspnea and hypoxemia 2 days after heart surgery. What procedure should the nurse anticipate assisting with to determine whether the patient has acute respiratory distress syndrome (ARDS) or pulmonary edema caused by heart failure?
Insertion of a pulmonary artery catheter
Obtaining a ventilation-perfusion scan
Drawing blood for arterial blood gases
Positioning the patient for a chest x-ray
The Correct Answer is A
A. The insertion of a pulmonary artery catheter can help in assessing hemodynamic parameters and distinguishing between these two conditions. It provides direct measurement of pulmonary artery pressures, which can be elevated in the case of heart failure.
B. A ventilation-perfusion (V/Q) scan is used to evaluate ventilation and perfusion in the lungs. While it can help identify areas of ventilation-perfusion mismatch, it may not be the most appropriate initial test for distinguishing between ARDS and pulmonary edema.
C. Drawing blood for arterial blood gases is also a critical step as it helps in assessing the severity of hypoxemia and respiratory failure.
D. A chest x-ray can show the presence of bilateral opacities, which are indicative of ARDS when cardiac failure or fluid overload is not the primary cause. However, transthoracic echocardiography (TTE) is often performed to seek evidence of cardiac dysfunction when cardiogenic pulmonary edema cannot be excluded by clinical evaluation, laboratory findings, or imaging.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
B Somnolence, or excessive sleepiness, can indicate respiratory depression, hypercapnia (elevated PaCO2), or impending respiratory failure. Somnolence in this context is concerning as it may suggest worsening respiratory status and impending respiratory compromise. Therefore, it should be immediately reported to the healthcare provider for further evaluation and intervention.
A blood pressure of 164/98 mmHg is elevated but may not necessarily require immediate intervention, especially if the patient is not exhibiting signs of acute hypertensive crisis or end-organ damage.
However, it should be closely monitored and managed as appropriate. While hypertension may contribute to respiratory distress, it may not be the most critical finding to report immediately in a patient with possible respiratory failure and a high PaCO2.
C An oxygen saturation of 90% indicates hypoxemia, which can exacerbate respiratory failure and contribute to respiratory distress. While hypoxemia requires prompt intervention to improve oxygenation, it may not be the most critical finding to report immediately if the patient is not showing signs of severe respiratory distress or impending respiratory failure. However, it should be closely monitored and managed to prevent further deterioration.
D Weakness is a nonspecific symptom and may be related to various underlying causes, including respiratory failure, electrolyte imbalances, or systemic illness. While weakness warrants further assessment and management, it may not be the most urgent finding to report immediately in a patient with possible respiratory failure and a high PaCO2 unless it is accompanied by other concerning symptoms or signs of impending respiratory compromise.
Correct Answer is B
Explanation
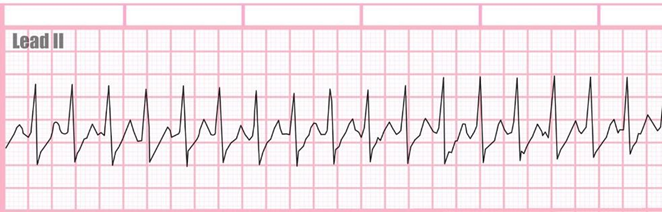
B This maneuver, called the Valsalva maneuver, can sometimes help to restore normal heart rhythm in cases of SVT. It involves blowing forcefully into a syringe or performing a similar action that increases intra-abdominal pressure, which can stimulate the vagus nerve and help to slow down the heart rate.
A Defibrillation is a treatment used for life-threatening cardiac arrhythmias, particularly ventricular fibrillation or pulseless ventricular tachycardia. It involves delivering a therapeutic dose of electrical energy to the heart with a device called a defibrillator.
C Drawing troponin levels may be appropriate if there is suspicion of myocardial infarction as the cause of chest palpitations or if there are other symptoms suggestive of acute coronary syndrome. However, in the context of SVT presenting with chest palpitations and a racing heart, the priority is to address the arrhythmia first
D Amiodarone is an antiarrhythmic medication used to treat various types of cardiac arrhythmias, including ventricular and supraventricular arrhythmias. While it can be effective in certain cases of SVT, it is not typically the first-line treatment or the immediate next step in managing SVT in the emergency department.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
