A nurse is evaluating the central venous pressure (CVP) of a client who has sustained multiple traumas. Which of the following interpretations of a low CVP should the nurse make?
Fluid overload
Intracardiac shunt
Hypovolemia
Left ventricular failure
The Correct Answer is C
Choice A Reason: This is incorrect because fluid overload is a condition of excess fluid volume in the body. A client who has fluid overload is more likely to have a high CVP, which indicates increased pressure in the right atrium and vena cava.
Choice B Reason: This is incorrect because an intracardiac shunt is a condition of abnormal blood flow between the chambers of the heart. A client who has an intracardiac shunt may have a normal or high CVP, depending on the direction and magnitude of the shunt.
Choice C Reason: This is correct because hypovolemia is a condition of low fluid volume in the body. A client who has hypovolemia is more likely to have a low CVP, which indicates decreased pressure in the right atrium and vena cava.
Choice D Reason: This is incorrect because left ventricular failure is a condition of impaired pumping function of the left ventricle. A client who has left ventricular failure may have a normal or high CVP, depending on the degree of backward failure and pulmonary congestion.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is C
Explanation
Choice A Reason: This is incorrect because right ventricular failure would cause an increase in right atrial pressure and right ventricular end-diastolic pressure, but not in PAWP, which reflects left atrial pressure and left ventricular end- diastolic pressure.
Choice B Reason: This is incorrect because fluid volume deficit would cause a decrease in PAWP, as there would be less blood volume in the pulmonary circulation.
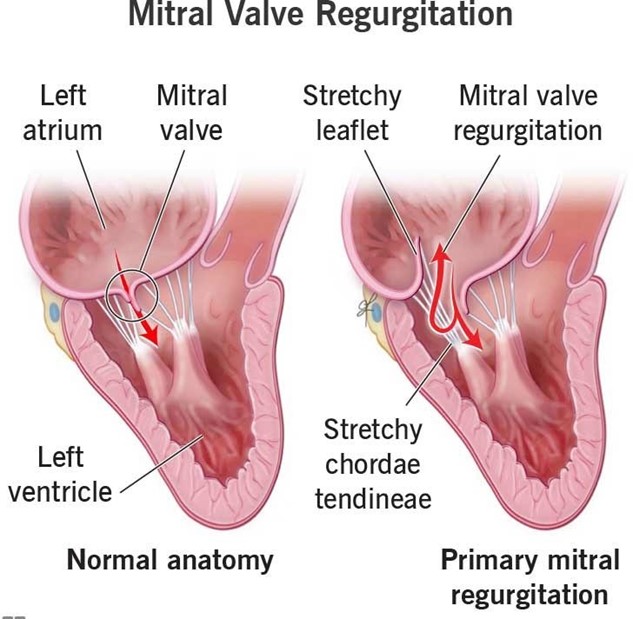
Choice C Reason: This is correct because mitral regurgitation would cause an increase in PAWP, as the blood would back up into the left atrium and pulmonary veins due to the incompetent mitral valve.
Choice D Reason: This is incorrect because afterload reduction would cause a decrease in PAWP, as there would be less resistance to the left ventricular ejection and less blood volume in the pulmonary circulation.
Correct Answer is A
Explanation
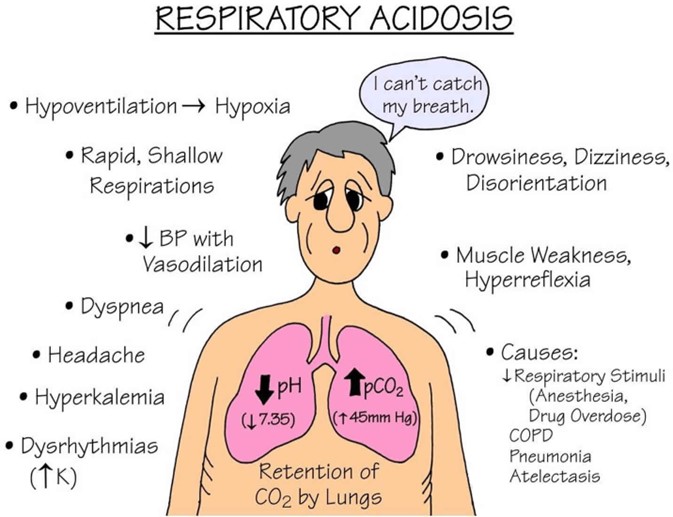
Choice A Reason: This choice is correct because respiratory acidosis is a condition in which the lungs cannot eliminate enough carbon dioxide (CO2) from the blood, resulting in a high level of CO2 (PaCO2) and a low level of pH. A normal PaCO2 range is 35 to 45 mm Hg, so a value of 50 mm Hg indicates respiratory acidosis.
Choice B Reason: This choice is incorrect because HCO3 (bicarbonate) is a base that helps to buffer the excess acid in the blood. In respiratory acidosis, the kidneys try to compensate by retaining more HCO3 and excreting more hydrogen ions. Therefore, a high level of HCO3 (above 26 mEq/L) would indicate a chronic or compensated respiratory acidosis, not an acute or uncompensated one.
Choice C Reason: This choice is incorrect because pH is a measure of the acidity or alkalinity of the blood. A normal pH range is 7.35 to 7.45, so a value of 7.45 indicates a neutral or slightly alkaline blood, not an acidic one. A low pH (below 7.35) would indicate respiratory acidosis.
Choice D Reason: This choice is incorrect because potassium is an electrolyte that helps to regulate the nerve and muscle function, as well as the fluid balance in the body. In respiratory acidosis, the increased hydrogen ions in the blood may shift into the cells in exchange for potassium, resulting in a high level of potassium (hyperkalemia).
Therefore, a low level of potassium (below 3.5 mEq/L) would indicate hypokalemia, not respiratory acidosis.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
