The practical nurse (PN) is monitoring the neurological vital signs of a client with a recently closed head injury. Which vital sign trends indicate increased intracranial pressure (ICP) and should be reported to the charge nurse?
Heart rate above 110 beats/minute, elevated respiratory rate, and hypotension.
Bounding pulse rate, groaning respiratory effort, and elevated blood pressure.
Thready rapid pulse, trembling, perspiration, weakness, and irritability.
Bradycardia, irregular respiratory patterns, widening pulse pressure.
The Correct Answer is D
The vital sign trends that indicate increased intracranial pressure (ICP) and should be reported to the charge nurse are:
Bradycardia: A slow heart rate can be a sign of increased ICP.
Irregular respiratory patterns: Abnormal breathing patterns, such as irregular or Cheyne-Stokes respirations, can be indicative of increased ICP.
Widening pulse pressure: An increased difference between systolic and diastolic blood pressure (widening pulse pressure) can be a sign of increased ICP.
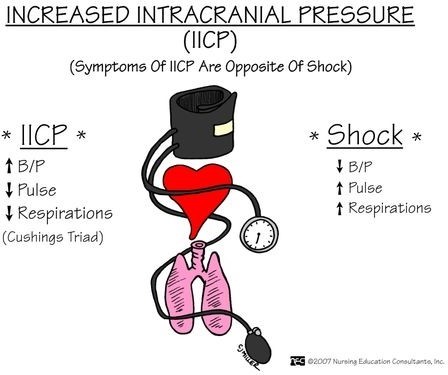
A- Heart rate above 110 beats/minute, elevated respiratory rate, and hypotension: While an elevated heart rate and respiratory rate can be associated with increased ICP, hypotension (low blood pressure) is not typically seen in this condition. Hypotension can be a sign of other factors, such as hypovolemia or shock, which may or may not be related to the head injury.
B- Bounding pulse rate, groaning respiratory effort, and elevated blood pressure: Bounding pulse rate and elevated blood pressure are not specific to increased ICP. They can be influenced by other factors such as pain, anxiety, or medications. Groaning respiratory effort may indicate respiratory distress, but it is not directly related to increased ICP.
C- Thready rapid pulse, trembling, perspiration, weakness, and irritability: These signs and symptoms can be associated with various conditions such as anxiety, stress, or other physiological responses. While they may occur in the context of increased ICP, they are not specific to this condition alone.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
After a hip arthroplasty with prosthesis placement, it is important to follow specific precautions to protect the surgical site and prevent dislocation of the hip joint. One common precaution is to avoid excessive internal rotation, adduction, and f
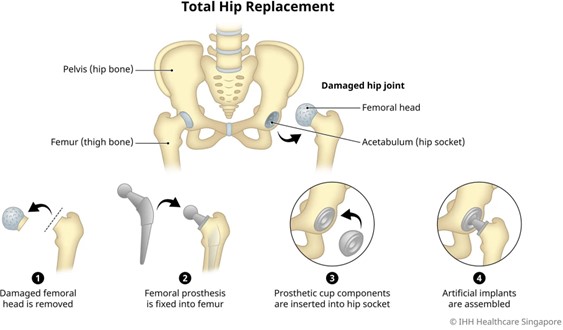
The other observations mentioned in the scenario are correct and demonstrate appropriate knowledge of the turning procedure:
A. Placing an abduction pillow between the client's legs helps maintain proper alignment and prevents adduction of the legs, which can cause hip dislocation.
C. Keeping the back straight and knees bent when moving the client promotes proper body mechanics and reduces the risk of injury to the UAPs.
D. Using a turning sheet under the client for turning and repositioning helps reduce friction and shearing forces, making the process safer and more comfortable for the client.
Correct Answer is C
Explanation
The best action for the practical nurse (PN) to assist the client in dealing with his pain would be to guide the client through slow, rhythmic breathing.
Guiding the client through slow, rhythmic breathing techniques can help promote relaxation and reduce anxiety, which can indirectly contribute to pain relief. Deep breathing exercises can help the client focus on their breath and divert attention away from the pain, providing some relief and helping them cope with the discomfort. It is a non-pharmacological intervention that can be implemented immediately to help the client manage their pain.
The other options are less effective or not appropriate in this situation:
A. Dimming the lights in the room and closing the door may create a more calming environment, but it does not directly address the client's pain or provide them with effective pain relief.
B. Turning the television on to the client's favorite show may serve as a distraction, but it may not be sufficient to alleviate the client's pain.
D. Obtaining a prescription for a higher dose of pain medication should only be considered after evaluating the client's current pain management regimen and assessing their response to the current medication. It is not the immediate best action to take without further assessment and consideration of other non-pharmacological interventions.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
