The nurse administers amiodarone to a client with ventricular tachycardia. Which monitoring by the nurse is necessary with this drug? (Select all that apply)
QT interval
Heart rate
Respiratory rate
Heart rhythm
Urine output
Correct Answer : A,B,C,D,E
Choice A Reason:
Monitoring the QT interval is crucial when administering amiodarone because this drug can prolong the QT interval, increasing the risk of torsades de pointes, a potentially life-threatening type of ventricular tachycardia. Regular monitoring helps in early detection and management of this adverse effect, ensuring patient safety.
Title: Choice B Reason:
Heart rate monitoring is essential as amiodarone can cause bradycardia (slow heart rate). Continuous monitoring allows the nurse to detect any significant changes in heart rate and take appropriate actions, such as adjusting the medication dosage or providing interventions to manage bradycardia.
Title: Choice C Reason:
Respiratory rate monitoring is necessary because amiodarone can cause pulmonary toxicity, including interstitial pneumonitis and acute respiratory distress syndrome (ARDS). By keeping track of the respiratory rate, the nurse can identify early signs of respiratory complications and intervene promptly
Title: Choice D Reason:
Heart rhythm monitoring is vital since amiodarone is used to treat arrhythmias. Continuous electrocardiogram (ECG) monitoring helps in assessing the effectiveness of the drug in controlling arrhythmias and detecting any new or worsening arrhythmias that may require immediate attention.
Title: Choice E Reason:
Monitoring urine output is important because amiodarone can affect renal function, especially in patients with pre-existing kidney conditions. Keeping track of urine output helps in assessing renal function and ensuring that the drug is not causing nephrotoxicity
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is ["B","C","D"]
Explanation
Choice A Reason:
Administering 0.45% NS (normal saline) at 50 mL/h is not appropriate for a client with SIADH (Syndrome of Inappropriate Antidiuretic Hormone Secretion). This solution is hypotonic and can exacerbate the condition by increasing water retention and worsening hyponatremia. Therefore, this choice is not included in the plan of care.
Choice B Reason:
Obtaining daily weight is crucial for monitoring fluid balance in clients with SIADH. Daily weights help detect fluid retention or loss, which is essential for managing the condition. Accurate weight measurements can indicate changes in fluid status and guide adjustments in treatment.
Choice C Reason:
Maintaining seizure precautions is vital for clients with SIADH because severe hyponatremia can lead to neurological symptoms, including seizures. Implementing seizure precautions helps ensure the client’s safety and allows for prompt intervention if seizures occur.
Choice D Reason:
Administering 3% saline as ordered is appropriate for treating severe hyponatremia in clients with SIADH. Hypertonic saline helps increase serum sodium levels, which is critical for correcting the electrolyte imbalance. This intervention should be closely monitored to avoid rapid changes in sodium levels.
Choice E Reason:
Encouraging fluid intake is not appropriate for clients with SIADH. The condition is characterized by excessive water retention, and increasing fluid intake can worsen hyponatremia. Instead, fluid restriction is typically recommended to manage the condition effectively.
Correct Answer is A
Explanation
Choice A Reason:
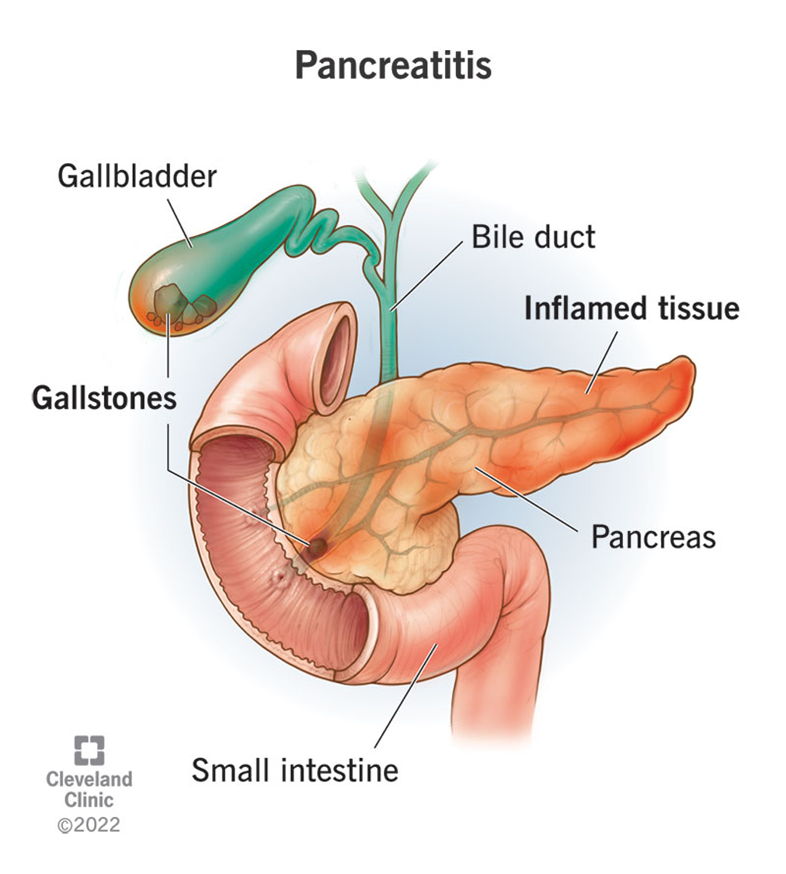
Increased serum amylase is a key indicator of acute pancreatitis. Amylase is an enzyme produced by the pancreas to help digest carbohydrates. In cases of acute pancreatitis, the pancreas becomes inflamed, leading to the release of amylase into the bloodstream. Elevated levels of serum amylase, typically more than three times the upper limit of normal, are a strong indication of acute pancreatitis. This enzyme level usually rises within a few hours of the onset of pancreatitis and can remain elevated for several days.
Choice B Reason:
Increased serum calcium is not typically associated with acute pancreatitis. In fact, acute pancreatitis can often lead to hypocalcemia (low calcium levels) due to fat saponification in the pancreas, where calcium binds with fatty acids. Therefore, an increase in serum calcium would not be expected in a patient with acute pancreatitis. Monitoring calcium levels is important, but an increase is not a diagnostic marker for this condition.
Choice C Reason:
Decreased WBC (white blood cell count) is not a characteristic finding in acute pancreatitis. On the contrary, acute pancreatitis often leads to an elevated WBC count due to the inflammatory response in the body. Leukocytosis (increased WBC) is a common finding in many inflammatory and infectious conditions, including acute pancreatitis. Therefore, a decreased WBC count would not be expected and does not support the diagnosis of acute pancreatitis.
Choice D Reason:
Decreased serum lipase is incorrect. Similar to amylase, lipase is another enzyme produced by the pancreas, which helps in the digestion of fats. In acute pancreatitis, serum lipase levels also increase significantly, often more than three times the upper limit of normal. Lipase levels tend to rise slightly later than amylase but remain elevated for a longer period, making it a useful marker for diagnosing acute pancreatitis. Therefore, decreased serum lipase would not be expected in this condition.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
