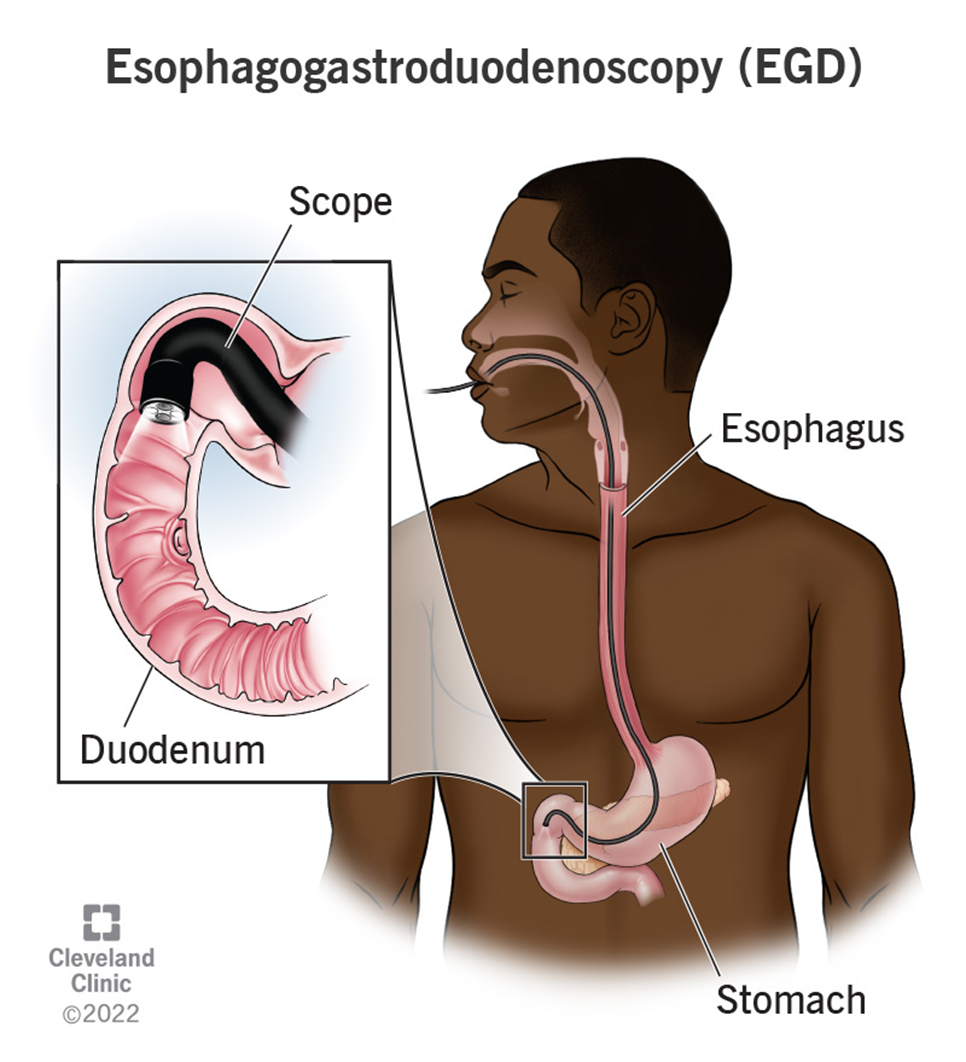
The nurse is caring for a client recovering from an esophagogastroduodenoscopy (EGD). Which of the following client symptoms would require further nursing assessment?
Thirst
Sore throat
Abdominal distention
Drowsiness
The Correct Answer is C
Choice A Reason:
Thirst is a common and expected symptom after an EGD, especially if the client has been fasting before the procedure. It does not typically indicate a complication and can be managed by gradually reintroducing fluids as tolerated. Therefore, thirst does not require further nursing assessment beyond routine post-procedure care.
Choice B Reason:
A sore throat is also a common symptom following an EGD. The procedure involves passing an endoscope through the throat, which can cause temporary irritation and discomfort. This symptom usually resolves on its own within a few days and does not indicate a serious complication. Therefore, a sore throat does not require further nursing assessment beyond providing comfort measures such as lozenges or warm saltwater gargles.
Choice C Reason:
Abdominal distention is a concerning symptom that requires further nursing assessment. It can indicate complications such as perforation, bleeding, or infection following the EGD. Perforation of the gastrointestinal tract is a rare but serious complication that can lead to peritonitis and sepsis if not promptly addressed. Therefore, any signs of abdominal distention should be reported to the provider immediately for further evaluation and intervention.
Choice D Reason:
Drowsiness is a common side effect of the sedatives used during the EGD procedure. It is expected that the client may feel drowsy or sleepy for a few hours after the procedure as the sedative wears off. This symptom does not typically require further nursing assessment unless it persists for an unusually long time or is accompanied by other concerning symptoms such as difficulty breathing or altered mental status.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is ["A","B","C"]
Explanation
Choice A reason: A 22-year-old client with asthma is considered a priority for pneumonia vaccination. Asthma is a chronic respiratory condition that can increase the risk of complications from pneumonia. Vaccination helps protect against pneumococcal infections, which can be particularly severe in individuals with underlying respiratory conditions.
Choice B reason: A healthy 72-year-old client is also a priority for pneumonia vaccination. The Centers for Disease Control and Prevention (CDC) recommends pneumococcal vaccination for all adults aged 65 years and older. Older adults are at higher risk for pneumococcal disease due to age-related decline in immune function.
Choice C reason: A client with well-controlled diabetes should be prioritized for pneumonia vaccination. Diabetes can weaken the immune system, making individuals more susceptible to infections, including pneumonia. Vaccination is an important preventive measure for individuals with chronic health conditions.
Choice D reason: A client who is taking medication for hypertension is not necessarily a priority for pneumonia vaccination based solely on their hypertension. While hypertension is a common condition, it does not directly increase the risk of pneumococcal disease. However, if the client has other risk factors or comorbidities, they may still be considered for vaccination.
Choice E reason: A client who had a cholecystectomy last year is not a priority for pneumonia vaccination based on this surgical history alone. A cholecystectomy, which is the removal of the gallbladder, does not increase the risk of pneumococcal disease. Priority for vaccination is typically given to individuals with chronic health conditions, older adults, and those with weakened immune systems.
Correct Answer is D
Explanation
Choice A Reason:
Assess the client’s oxygen saturation and, if normal, turn off the oxygen. This option is not ideal because turning off the oxygen completely can lead to a rapid drop in oxygen saturation levels, especially in patients who require continuous oxygen therapy. Monitoring oxygen saturation is crucial, but turning off the oxygen is not recommended unless specifically advised by a healthcare provider. Normal oxygen saturation levels typically range from 95% to 100%1. If the levels drop below 90%, it can lead to hypoxemia, which can cause serious complications.
Choice B Reason:
Have the client lift the mask off the face when taking bites of food. This option is also not ideal because it can be cumbersome for the client and may lead to inconsistent oxygen delivery. The Venturi mask is designed to provide a precise concentration of oxygen, and lifting it off repeatedly can disrupt this consistency. Additionally, it can be uncomfortable and impractical for the client to manage the mask while eating.
Choice C Reason:
Turn the oxygen off while the client eats the meal and then restart it. This option is not recommended for similar reasons as Choice A. Turning off the oxygen can lead to a significant drop in oxygen saturation levels, which can be dangerous for the client. Continuous oxygen therapy is essential for maintaining adequate oxygen levels in patients who require it. Interrupting this therapy, even temporarily, can have adverse effects on the client’s health.
Choice D Reason:
Determine if the client can switch to a nasal cannula during the meal. This is the best option because a nasal cannula allows the client to receive continuous oxygen while eating. The nasal cannula is less obtrusive and more comfortable for the client, enabling them to eat without significant interruption to their oxygen therapy. Nasal cannulas are commonly used for patients who need supplemental oxygen but also need to perform activities such as eating and talking. This approach ensures that the client maintains adequate oxygen levels while having their meal.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
