A patient is admitted for pain in the arm and jaw. The patient is later diagnosed with angina.
What type of pain does the arm and jaw pain most likely represent?
Intractable
Phantom
Referred
Cramping
The Correct Answer is C
Choice A rationale:
Intractable pain is pain that is persistent and does not respond to usual pain management methods. While angina can be intractable in some cases, it does not typically manifest as pain in the arm and jaw. Moreover, the patient in this scenario has not yet undergone pain management efforts, so it's premature to classify the pain as intractable.
Choice B rationale:
Phantom pain is pain that is felt in a part of the body that has been amputated or is no longer there. The patient in this scenario has not experienced any amputations, so phantom pain is not a valid explanation for the arm and jaw pain.
Choice C rationale:
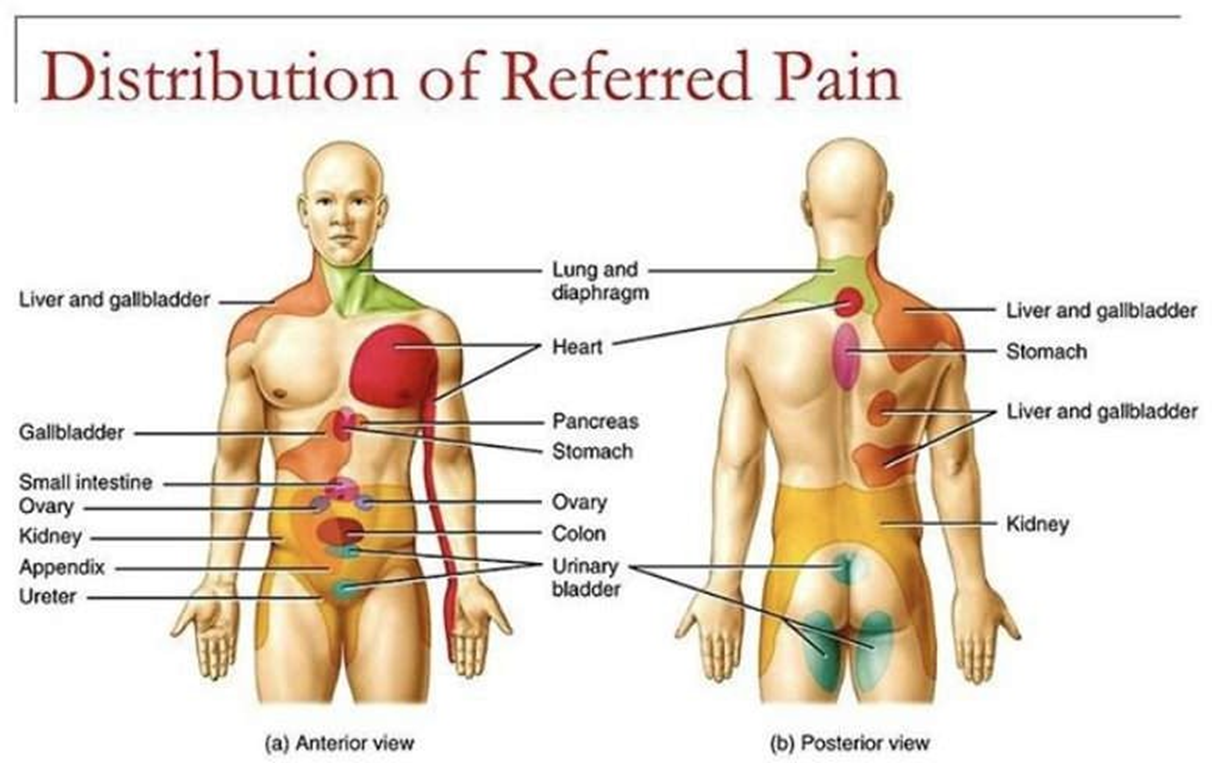
Referred pain is pain that is felt in a part of the body that is different from the source of the pain. This is the most likely explanation for the arm and jaw pain in this patient. The heart and the arm and jaw share nerve pathways, so pain signals from the heart can be misinterpreted by the brain as coming from these other areas. This is a common phenomenon in patients with angina.
Choice D rationale:
Cramping pain is a type of pain that is often described as a muscle tightening or squeezing sensation. It is not typically associated with angina. While angina can sometimes cause chest tightness, it's not characterized by cramping in the arm and jaw.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
Choice A rationale:
Painful urination (dysuria) can be a sign of several conditions that could potentially affect the client's IVP or indicate a need for further assessment. These conditions include:
Urinary tract infection (UTI): UTIs are common in clients with recurrent kidney stones, and they can cause inflammation and pain in the urinary tract. If a client has a UTI, it's important to treat it before the IVP to reduce the risk of spreading the infection to the kidneys.
Kidney stone passage: The client's history of kidney stones makes it possible that the pain could be due to the passage of a stone. This would be important information for the healthcare team to know, as it could affect the interpretation of the IVP results.
Other urological conditions: There are other urological conditions, such as bladder or urethral strictures, that can also cause painful urination. These conditions might also need to be considered and assessed for.
It's important for the nurse to collect more data about the client's painful urination to determine the underlying cause and whether it could impact the IVP. This might include asking questions about:
The severity and duration of the pain
Any other associated symptoms, such as fever, urgency, or frequency The client's history of UTIs or kidney stones
Any recent changes in urinary habits
Based on this additional information, the nurse can then collaborate with the healthcare team to determine the best course of action, which might include:
Further assessment, such as a urinalysis or urine culture Treatment for a UTI, if present
Pain management
Rescheduling the IVP, if necessary
Correct Answer is B
Explanation
Choice A rationale:
Incorrect. Patients have a legal right to access their medical records under the Health Information Portability and Accountability Act (HIPAA). Denying access is a violation of patient rights and could lead to legal consequences.
Undermines patient autonomy and trust. Patients have a right to know what information is in their medical records and to participate in their own healthcare decisions. Denying access can erode trust in the healthcare system.
Potential for errors and misunderstandings. If patients cannot review their records, they may not be able to identify errors or misunderstandings that could impact their care.
Choice B rationale:
Correct. This response upholds patient rights while ensuring that the request for access is documented and handled appropriately.
Protects patient privacy and confidentiality. The written request process helps to ensure that only the patient or their authorized representative has access to the records.
Provides a mechanism for tracking and auditing access requests. This can help to prevent unauthorized access and ensure compliance with HIPAA regulations.
Choice C rationale:
Incorrect. Patients have a right to access their records at any time, not just when they are being discharged.
Delays access to information. Patients may need to review their records to make informed decisions about their care, even if they are not being discharged.
Potential for records to be lost or misplaced. There is a risk that records could be lost or misplaced if they are not provided to the patient until discharge.
Choice D rationale:
Incorrect. Patients do not need to provide a reason for wanting to access their medical records.
Intrusive and unnecessary. Patients may feel uncomfortable or embarrassed about having to explain their reasons for wanting to access their records.
Potential for discrimination. Patients may be less likely to request access to their records if they feel that they will be judged or questioned about their reasons for doing so.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
