A nurse is caring for a client who is postoperative and requesting something to drink.
The nurse reads the client’s postoperative prescriptions, which include, “Clear liquids, advance diet as tolerated.” What action should the nurse take first?
Elevate the client’s head of bed.
Offer the client apple juice.
Auscultate the client’s abdomen.
Order a lunch tray for the client.
The Correct Answer is C
Choice A rationale:
Elevating the head of the bed can promote comfort and ease breathing, but it's not the first priority in this situation. The nurse needs to assess the client's gastrointestinal status before offering any fluids or food.
While elevating the head of the bed may be helpful in some postoperative situations, it doesn't directly address the client's request for something to drink or the need to assess for potential contraindications to oral intake.
It's important to prioritize assessment before intervention to ensure safe and effective care.
Choice B rationale:
Offering apple juice, a clear liquid, might seem appropriate given the postoperative orders, but it's premature without first assessing the client's abdomen.
Auscultation can reveal important information about bowel sounds, which can indicate whether the client's gastrointestinal system is ready to tolerate fluids or food.
Prematurely offering fluids could lead to complications like nausea, vomiting, or aspiration if the client's bowels are not functioning properly.
Choice D rationale:
Ordering a lunch tray is not appropriate at this stage. The nurse needs to first assess the client's tolerance for clear liquids before advancing the diet.
Advancing the diet too quickly could also lead to gastrointestinal complications.
It's important to follow the postoperative orders and progress the diet gradually as tolerated.
Choice C rationale:
Auscultating the client's abdomen is the essential first step in this scenario. It allows the nurse to gather crucial data about the client's gastrointestinal status.
By listening to bowel sounds, the nurse can determine if the client's intestines are active and functioning properly. If bowel sounds are present and normal, it suggests that the client is likely able to tolerate clear liquids.
If bowel sounds are absent or abnormal, it may indicate a potential problem, such as ileus (a temporary paralysis of the intestines), and the nurse would need to hold oral intake and notify the healthcare provider.
This assessment provides essential information to guide the nurse's subsequent actions and ensure the client's safety.
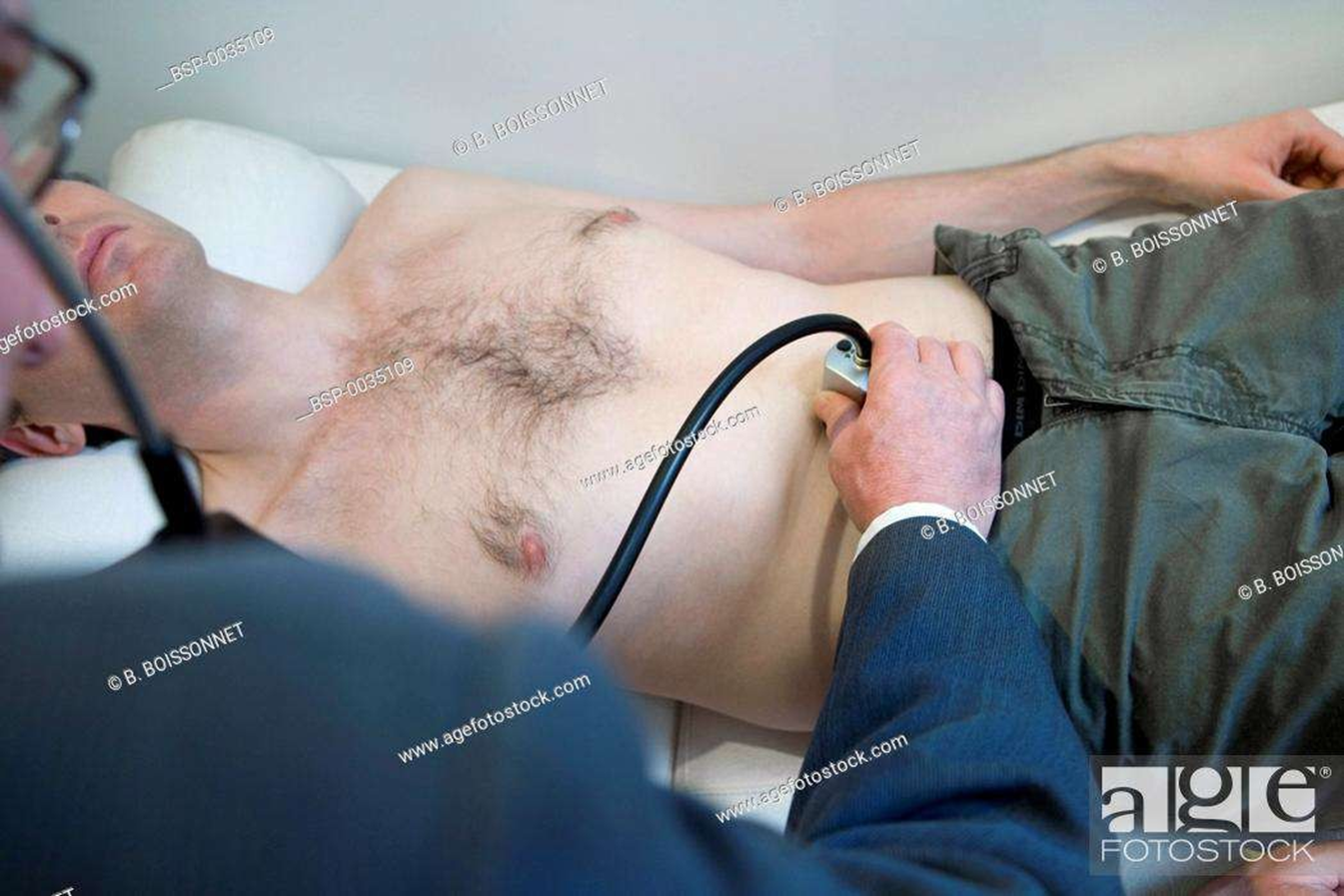
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
Choice A rationale:
Tenderness to touch is a common finding in wounds healing by secondary intention. It's often due to inflammation, which is a normal part of the healing process. The inflammation brings in cells and substances that promote healing. However, increased tenderness, especially when accompanied by other signs of infection, should be reported.
Choice B rationale:
A halo of erythema on the surrounding skin is a sign of infection. This is a serious complication that can delay healing and lead to further complications. The erythema indicates that the infection is spreading beyond the wound edges and needs prompt attention.
Choice C rationale:
Drainage of serosanguineous fluid is also common in wounds healing by secondary intention. This fluid is a mixture of serum (clear yellowish fluid) and blood. It's a sign that the wound is cleaning itself and new tissue is forming. While excessive drainage or a change in color or odor could signal a problem, drainage itself is not necessarily a cause for concern.
Choice D rationale:
Pink, shiny tissue with a granular appearance is a sign of healthy granulation tissue. This is a type of tissue that forms during the healing process. It's rich in blood vessels and collagen, which are essential for wound healing. The presence of granulation tissue indicates that the wound is healing well.
Correct Answer is B
Explanation
Choice A rationale:
The spinal cord plays a crucial role in pain transmission, but it does not initiate the afferent pathways. It receives pain signals from nociceptors and relays them to the brain for processing.
The spinal cord is also involved in pain modulation, as it can dampen or amplify pain signals depending on various factors. However, it is not the primary trigger for pain sensation. That role belongs to nociceptors.
Choice B rationale:
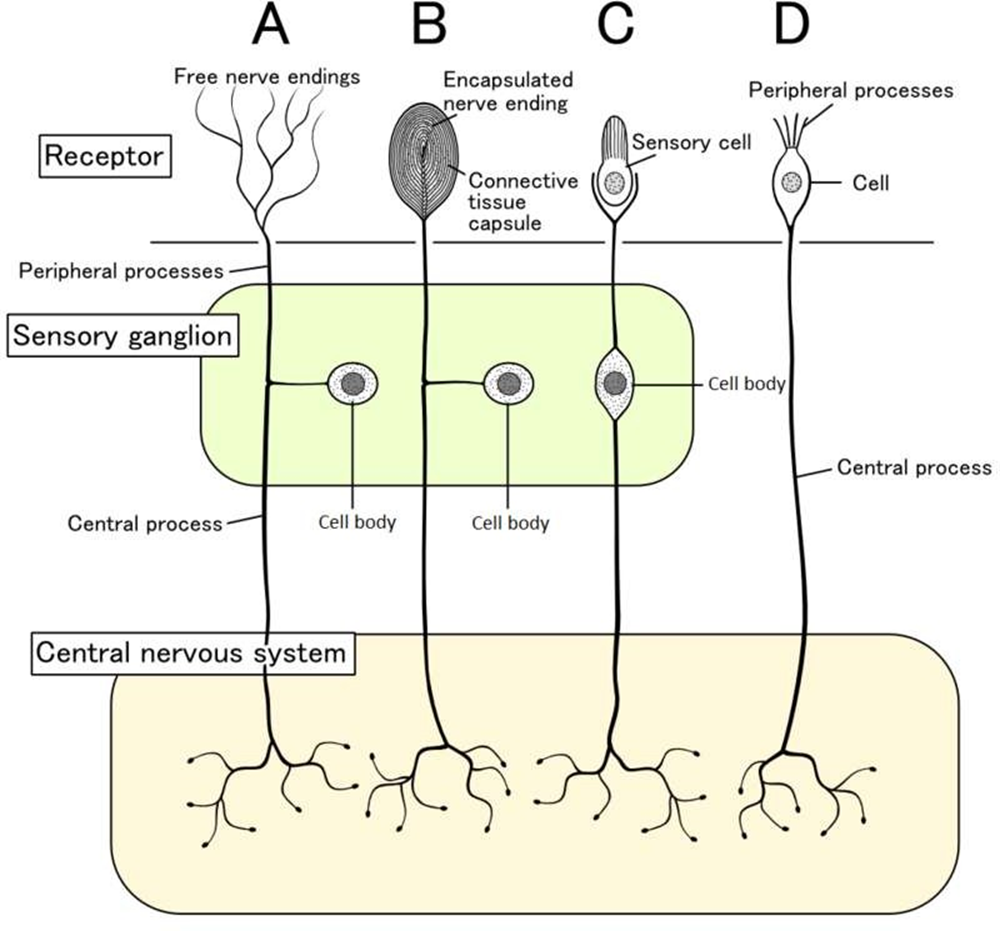
Nociceptors are specialized sensory receptors that detect potentially damaging stimuli, such as intense heat, pressure, or chemical irritants.
They are located throughout the body, including the skin, muscles, joints, and internal organs.
When nociceptors are activated, they generate electrical signals that travel along nerve fibers to the spinal cord and brain. This process initiates the afferent pathways, which ultimately lead to the conscious perception of pain.
Nociceptors are essential for protecting the body from harm. They alert us to potential dangers and trigger responses that help us avoid injury or further damage.
Choice C rationale:
Endorphins are natural pain-relieving substances produced by the body. They act on receptors in the brain and spinal cord to reduce pain perception.
However, endorphins do not trigger the afferent pathways. They work by modulating pain signals that have already been initiated by nociceptors.
Choice D rationale:
The cortex is the outer layer of the brain that is responsible for higher-level functions, such as thinking, feeling, and decision- making.
It plays a role in the conscious experience of pain, but it does not trigger the afferent pathways.
The cortex receives pain signals from the spinal cord and processes them, leading to the awareness of pain.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
