A nurse is monitoring a patient who is receiving a blood transfusion.
Which of the following symptoms should the nurse report to the charge nurse as a sign of an allergic blood transfusion reaction?
Bilateral flank pain.
Distended jugular veins.
Generalized urticaria.
Blood pressure 184/92 mm Hg.
The Correct Answer is C
Choice A rationale:
Bilateral flank pain is not a typical sign of an allergic blood transfusion reaction. It can be associated with other conditions, such as kidney problems, musculoskeletal issues, or abdominal aortic aneurysm. While it's important to assess flank pain, it doesn't directly suggest an allergic reaction to the transfusion.
Choice B Rationale:
Distended jugular veins can indicate fluid overload, which could potentially occur during a transfusion. However, it's not a specific sign of an allergic reaction. Fluid overload can result from various causes, including heart failure, kidney problems, or excessive fluid intake. It's crucial to monitor for fluid overload during transfusions, but it doesn't definitively point to an allergic reaction.
Choice C Rationale:
Generalized urticaria, or hives, is a hallmark sign of an allergic reaction. It's characterized by raised, red, itchy welts that can appear on various parts of the body. Hives can develop rapidly and spread extensively. During a blood transfusion, generalized urticaria strongly suggests that the patient's immune system is reacting to a component of the transfused blood, such as proteins or antibodies.
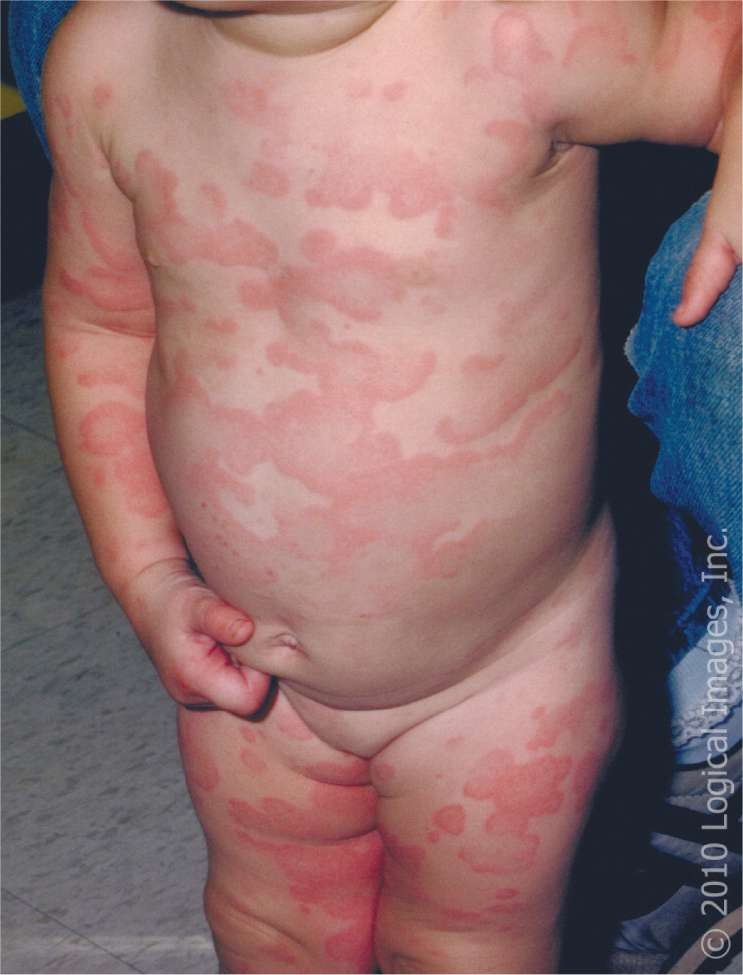
Choice D Rationale:
Blood pressure 184/92 mm Hg is elevated and could be concerning, but it's not specific to allergic reactions. High blood pressure can have various causes, including stress, pain, anxiety, or underlying hypertension. While monitoring blood pressure during transfusions is essential, it doesn't directly indicate an allergic reaction.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
The correct answer is Choice A.
Choice A rationale: Encouraging increased fluid intake helps maintain blood volume and reduces viscosity, promoting circulation and lowering the risk of venous stasis and clot formation postoperatively.
Choice B rationale: Keeping the affected knee flexed impairs venous return and increases stasis, elevating the risk of thrombosis. Proper positioning with extension promotes circulation and reduces clot risk.
Choice C rationale: Prolonged bed rest contributes to immobility-induced venous stasis, a major risk factor for DVT. Early ambulation and leg exercises are essential to prevent thromboembolic events.
Choice D rationale: Massaging the calf of a postoperative patient is contraindicated due to the risk of dislodging a thrombus, potentially leading to a life-threatening pulmonary embolism.
Correct Answer is C
Explanation
Choice A rationale:
Elevating the head of the bed can promote comfort and ease breathing, but it's not the first priority in this situation. The nurse needs to assess the client's gastrointestinal status before offering any fluids or food.
While elevating the head of the bed may be helpful in some postoperative situations, it doesn't directly address the client's request for something to drink or the need to assess for potential contraindications to oral intake.
It's important to prioritize assessment before intervention to ensure safe and effective care.
Choice B rationale:
Offering apple juice, a clear liquid, might seem appropriate given the postoperative orders, but it's premature without first assessing the client's abdomen.
Auscultation can reveal important information about bowel sounds, which can indicate whether the client's gastrointestinal system is ready to tolerate fluids or food.
Prematurely offering fluids could lead to complications like nausea, vomiting, or aspiration if the client's bowels are not functioning properly.
Choice D rationale:
Ordering a lunch tray is not appropriate at this stage. The nurse needs to first assess the client's tolerance for clear liquids before advancing the diet.
Advancing the diet too quickly could also lead to gastrointestinal complications.
It's important to follow the postoperative orders and progress the diet gradually as tolerated.
Choice C rationale:
Auscultating the client's abdomen is the essential first step in this scenario. It allows the nurse to gather crucial data about the client's gastrointestinal status.
By listening to bowel sounds, the nurse can determine if the client's intestines are active and functioning properly. If bowel sounds are present and normal, it suggests that the client is likely able to tolerate clear liquids.
If bowel sounds are absent or abnormal, it may indicate a potential problem, such as ileus (a temporary paralysis of the intestines), and the nurse would need to hold oral intake and notify the healthcare provider.
This assessment provides essential information to guide the nurse's subsequent actions and ensure the client's safety.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
