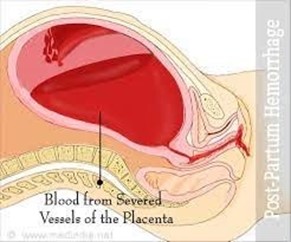
A nurse is assisting in the care of a client who is experiencing a postpartum hemorrhage.
Which of the following medications should the nurse plan to administer?
Terbutaline
Methylergonovine
Magnesium sulfate
Nifedipine
The Correct Answer is B
b. Methylergonovine.
Explanation:
Postpartum hemorrhage is a significant complication that can occur after childbirth. Methylergonovine is a medication commonly used to manage postpartum hemorrhage. It is an ergot alkaloid that helps to contract the uterus, reducing bleeding. It is typically administered either intramuscularly or orally.
Option a, Terbutaline, is a medication used for the management of preterm labor by relaxing the uterine smooth muscles. It is not indicated for postpartum hemorrhage.
Option c, Magnesium sulfate, is a medication used for the prevention and treatment of seizures in patients with preeclampsia or eclampsia. It is not specifically indicated for postpartum hemorrhage.
Option d, Nifedipine, is a calcium channel blocker commonly used to manage hypertension. It is not indicated for postpartum hemorrhage.
It's important to note that the specific management of postpartum hemorrhage may vary depending on the underlying cause, severity of bleeding, and individual patient factors. The healthcare provider will determine the most appropriate interventions and medications for each case.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
Answer: B. Elevated skin patches
Rationale:
A. Constipation:
Constipation is not a typical adverse effect of cefazolin. Antibiotics generally cause gastrointestinal symptoms like diarrhea rather than constipation, so this is not a primary concern with cefazolin therapy.
B. Elevated skin patches:
Elevated skin patches may indicate an allergic reaction, such as hives or a rash, which can be a serious side effect of cefazolin. Allergic reactions to antibiotics can escalate quickly and may require immediate medical attention. Monitoring for and reporting any skin changes is important to prevent potential complications.
C. Ringing in the ears:
Tinnitus (ringing in the ears) is not commonly associated with cefazolin. This symptom is more frequently associated with certain other antibiotics, such as aminoglycosides, but is not a primary concern with cefazolin use.
D. Depression:
Depression is not a known side effect of cefazolin. While mood changes may be seen with some medications, cefazolin’s primary side effects are related to hypersensitivity reactions and gastrointestinal symptoms.
Correct Answer is B
Explanation
The nurse should report the possible abuse to adult protective services if an older adult client states that their child took all their money. This is an important nursing intervention to ensure the safety and well-being of the client.
a) Instructing the client to report the theft to the police may be appropriate, but it is not the first action the nurse should take. The nurse has a legal and ethical obligation to report suspected abuse to the appropriate authorities.
c) Asking the client if there is another family member they can call for financial help may be appropriate, but it does not address the issue of possible abuse.
d) Restricting visitation for the client's family until discharge is not appropriate and may violate the client's rights.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
