A nurse is assessing four female clients for obesity. Which of the following clients have manifestations of obesity?
Client who weighs 28% above ideal body weight
Client who has a waist circumference of 81.3 cm (32 in)
Client who has a BMI of 28
Client who has a body fat of 22%
The Correct Answer is A
Choice A reason: This is the correct answer because weighing 28% above ideal body weight is a sign of obesity. Ideal body weight is an estimate of the weight that corresponds to the lowest mortality for a given height and gender. Obesity is defined as having a body weight that is 20% or more above ideal body weight.
Choice B reason: This is not the correct answer because having a waist circumference of 81.3 cm (32 in) is not a manifestation of obesity. Waist circumference is a measure of abdominal fat, which is associated with increased health risks. However, the cut-off point for waist circumference varies by gender and ethnicity. For women, a waist circumference of more than 88 cm (35 in) is considered high.
Choice C reason: This is not the correct answer because having a BMI of 28 is not a manifestation of obesity. BMI is a measure of body mass index, which is calculated by dividing weight in kilograms by height in meters squared. BMI is used to classify weight status and health risks. For adults, a BMI of 18.5 to 24.9 is considered normal, 25 to 29.9 is considered overweight, and 30 or more is considered obese.
Choice D reason: This is not the correct answer because having a body fat of 22% is not a manifestation of obesity. Body fat is a measure of the percentage of fat in the body, which is determined by various methods such as skinfold thickness, bioelectrical impedance, or underwater weighing. Body fat is influenced by age, gender, and physical activity. For women, a body fat of 21 to 33% is considered normal, 33 to 39% is considered high, and more than 39% is considered very high.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is C
Explanation
Choice A reason: This is not a correct finding for hypervolemia. Hypotension is a low blood pressure, which can be caused by hypovolemia (low blood volume) or other factors. Hypervolemia is an excess of fluid in the body, which can increase the blood pressure.
Choice B reason: This is not a correct finding for hypervolemia. Bradycardia is a slow heart rate, which can be caused by heart block, medication, or other factors. Hypervolemia can cause tachycardia (fast heart rate) as the heart tries to pump the excess fluid.
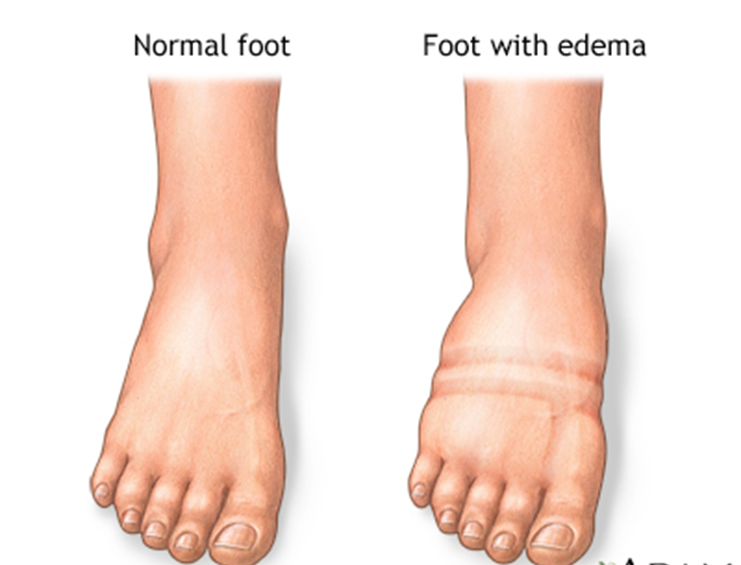
Choice C reason: This is a correct finding for hypervolemia. Peripheral edema is a swelling of the extremities due to fluid accumulation in the tissues. Hypervolemia can cause peripheral edema as the fluid leaks from the blood vessels into the interstitial spaces.
Choice D reason: This is not a correct finding for hypervolemia. Weight loss is a decrease in body weight, which can be caused by dehydration, malnutrition, or other factors. Hypervolemia can cause weight gain as the body retains more fluid.
Correct Answer is B
Explanation
Choice A reason: Gastritis is not the most likely condition that these clinical manifestations indicate. Gastritis is an inflammation of the stomach lining, which can cause abdominal pain, nausea, vomiting, and loss of appetite. Gastritis may cause heartburn or dyspepsia, but it does not usually cause dysphagia, which is difficulty swallowing.
Choice B reason: GERD is the most likely condition that these clinical manifestations indicate. GERD stands for gastroesophageal reflux disease, which is a chronic condition where the stomach acid flows back into the esophagus, causing irritation and inflammation. GERD can cause heartburn, which is a burning sensation in the chest or throat, dysphagia, which is difficulty swallowing or a feeling of a lump in the throat, and dyspepsia, which is indigestion or discomfort in the upper abdomen.
Choice C reason: Peptic ulcer disease is not the most likely condition that these clinical manifestations indicate. Peptic ulcer disease is a condition where there are open sores or ulcers in the lining of the stomach or duodenum, which can cause bleeding, perforation, or obstruction. Peptic ulcer disease can cause dyspepsia, which is indigestion or discomfort in the upper abdomen, but it does not usually cause heartburn or dysphagia, which are more characteristic of GERD.
Choice D reason: Pancreatitis is not the most likely condition that these clinical manifestations indicate. Pancreatitis is an inflammation of the pancreas, which can cause severe abdominal pain, nausea, vomiting, fever, and jaundice. Pancreatitis does not cause heartburn, dysphagia, or dyspepsia, which are more characteristic of GERD.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
