A nurse collects the health history of a 65-year-old client. Which of the following risk factors in the client's history puts the client at the highest risk for embolic stroke?
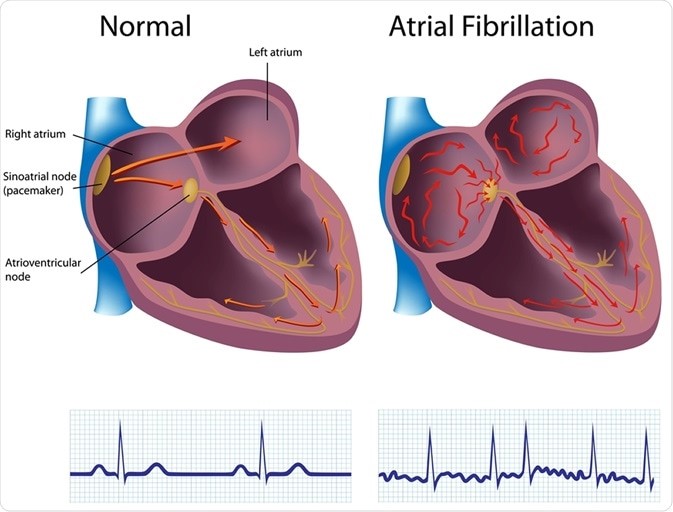
Atrial fibrillation.
Hypertension.
Diabetes.
Alcohol abuse.
The Correct Answer is A
Choice A reason: This is the correct answer because atrial fibrillation is the risk factor that puts the client at
the highest risk for embolic stroke. Atrial fibrillation is an irregular and rapid heart rate that causes poor blood flow and blood pooling in the heart chambers. This can lead to the formation of blood clots that can travel to the brain and block an artery, causing an embolic stroke.
Choice B reason: This is incorrect because hypertension is not the risk factor that puts the client at
the highest risk for embolic stroke. Hypertension is high blood pressure that puts stress on the blood vessels and increases the risk of bleeding or rupture. This can lead to a hemorrhagic stroke, but not an embolic stroke.
Choice C reason: This is incorrect because diabetes is not the risk factor that puts the client at
the highest risk for embolic stroke. Diabetes is a condition that causes high blood sugar levels and damages the blood vessels and nerves. This can lead to poor circulation and increased risk of infection and ulcers, but not an embolic stroke.
Choice D reason: This is incorrect because alcohol abuse is not the risk factor that puts the client at
the highest risk for embolic stroke. Alcohol abuse is excessive consumption of alcohol that affects liver function and blood clotting factors. This can lead to liver disease and bleeding disorders, but not an embolic stroke.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
Choice A Reason: This is incorrect because inability to recognize any words may indicate a problem with the auditory cortex, which is the part of the brain that processes sound, not the inner ear. The inner ear consists of the cochlea, which converts sound waves into nerve impulses, and the vestibular system, which helps with balance and orientation.
Choice B Reason: This is correct because loss of balance is a common symptom of an inner ear infection. An inner ear infection can cause inflammation and fluid buildup in the vestibular system, which can disrupt the sense of equilibrium and cause vertigo, dizziness, or nausea.
Choice C Reason: This is incorrect because twitching of the cheek may indicate a problem with the facial nerve, which controls the muscles of facial expression, not the inner ear. The facial nerve runs close to the inner ear, but it is not part of it.
Choice D Reason: This is incorrect because lack of air sound may indicate a problem with the outer or middle ear, which transmit sound waves to the inner ear, not the inner ear itself. The outer ear consists of the pinna and the ear canal, and the middle ear consists of the eardrum and the ossicles.
Correct Answer is D
Explanation
Choice A Reason: This choice is incorrect. Losing bladder control is not a feature of complex partial seizures, but rather of generalized tonic-clonic seizures. Complex partial seizures are a type of focal seizures that affect a specific area of the brain and cause impaired awareness and automatisms. Automatisms are repetitive and involuntary movements or behaviors that occur during a seizure.
Choice B Reason: This choice is incorrect. Having fixed and dilated eyes is not a feature of complex partial seizures, but rather of brain death or severe brain injury. Complex partial seizures do not affect the pupils or eye movements, but rather the level of consciousness and motor activity.
Choice C Reason: This choice is incorrect. Making involuntary groaning sounds is not a feature of complex partial seizures, but rather of simple partial seizures. Simple partial seizures are a type of focal seizures that affect a specific area of the brain and do not impair awareness or cause automatisms. They can cause sensory, motor, or psychic symptoms, such as auditory or visual hallucinations, tingling sensations, or emotional changes.
Choice D Reason: This is the correct choice. Having involuntary facial movements, such as lip-smacking, is a feature of complex partial seizures. Complex partial seizures often originate from the temporal lobe of the brain, which is involved in memory, language, and emotion. They can cause automatisms that affect the mouth, face, or hands, such as chewing, swallowing, picking, or fidgeting.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
