A nurse is caring for a client who has a T-4 spinal cord injury. Which of the following client findings should the nurse identify as an indication the client is at risk for experiencing autonomic dysreflexia?
The client's bladder becomes distended.
The client states having a severe headache.
The client's blood pressure becomes elevated.
The client states having nasal congestion.
Correct Answer : A,B,C,D
Choice A Reason: A distended bladder is one of the most common triggers of autonomic dysreflexia, which is a life-threatening condition that occurs in clients with spinal cord injuries above T-6. The bladder becomes overfilled and stimulates the sympathetic nervous system, causing vasoconstriction and hypertension.
Choice B Reason: A severe headache is one of the most common symptoms of autonomic dysreflexia, caused by the increased blood pressure in the brain. The headache may be accompanied by blurred vision, sweating, flushing, or anxiety.
Choice C Reason: An elevated blood pressure is the hallmark sign of autonomic dysreflexia, which can reach dangerously high levels and cause stroke, seizure, or death. The blood pressure may rise up to 300/160 mmHg or higher.
Choice D Reason: Nasal congestion is another possible trigger of autonomic dysreflexia, as it stimulates the nasal mucosa and activates the sympathetic nervous system. Other potential triggers include bowel impaction, skin irritation, tight clothing, or temperature changes.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is D
Explanation
Choice A reason: This is incorrect because laceration is not an acute traumatic brain injury, but a type of wound that involves tearing or cutting of the skin or other tissues. Laceration can occur as a result of a motor vehicle accident, but it does not cause changes in the GCS or pupil size. The nurse should assess the client's skin for any signs of laceration, such as bleeding, swelling, or infection.
Choice B reason: This is incorrect because acute subdural hematoma is not likely to cause a dilated pupil on the left side. Acute subdural hematoma is a type of traumatic brain injury that involves bleeding between the dura mater and the arachnoid mater, which are two layers of the meninges that cover the brain. An acute subdural hematoma can cause a rapid decrease in the GCS, but it usually causes a dilated pupil on the same side as the injury, not on the opposite side.
Choice C reason: This is incorrect because intracerebral hemorrhage is not likely to cause a dilated pupil on the left side. Intracerebral hemorrhage is a type of traumatic brain injury that involves bleeding within the brain tissue itself. Intracerebral hemorrhage can cause a gradual decrease in the GCS, but it usually causes neurological deficits that correspond to the location of the bleeding, such as weakness, numbness, or aphasia, not pupillary changes.
Choice D reason: This is correct because epidural hematoma can cause a dilated pupil on the left side. Epidural hematoma is a type of traumatic brain injury that involves bleeding between the dura mater and the skull. Epidural hematoma can cause a lucid interval, which is a period of normal consciousness followed by a sudden decrease in the GCS, and a dilated pupil on the opposite side of the injury, due to compression of the third cranial nerve. The nurse should notify the provider immediately and prepare for emergency surgery.
Correct Answer is ["D","E"]
Explanation
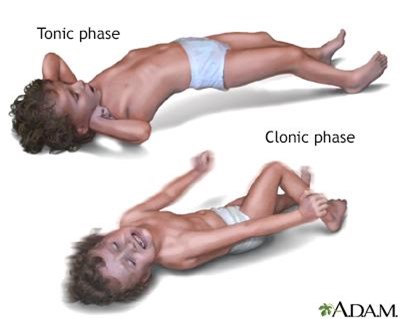
Choice A Reason: This choice is incorrect. Placing the client into a supine position is not an action that the nurse should take, as it can compromise the airway and increase the risk of aspiration. The nurse should position the client on their side with their head tilted slightly forward to allow saliva and secretions to drain out of their mouth.
Choice B Reason: This choice is incorrect. Applying restraints is not an action that the nurse should take, as it can cause injury and increase agitation. The nurse should protect the client from harm by removing any objects or furniture that may cause harm and padding any hard surfaces with blankets or pillows.
Choice C Reason: This choice is incorrect. Inserting a bite stick into the client's mouth is not an action that the nurse should take, as it can cause injury and obstruction. The nurse should never force anything into the client's mouth during a seizure, as it can damage their teeth, gums, tongue, or jaw.
Choice D Reason: This is a correct choice. Loosening restrictive clothing is an action that the nurse should take, as it can improve breathing and circulation. The nurse should unbutton any tight collars, belts, or ties that may constrict the chest or neck.
Choice E Reason: This is a correct choice. Placing a pillow under the client's head is an action that the nurse should take, as it can prevent injury and provide comfort. The nurse should support the client's head with a soft pillow or cushion to prevent hitting it against any hard surfaces.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
