A client with a complex cardiac history is scheduled for transthoracic echocardiography. What should the nurse teach the client in anticipation of this diagnostic procedure?
The test is noninvasive, and nothing will be inserted into the client's body.
The client's pain will be managed aggressively during the procedure
The test will provide a detailed profile of the heart's electrical activity
The client will remain on bed rest for 1 to 2 hours after the test
The Correct Answer is A
The nurse should teach the client that the transthoracic echocardiography is a noninvasive test and that nothing will be inserted into the client's body.
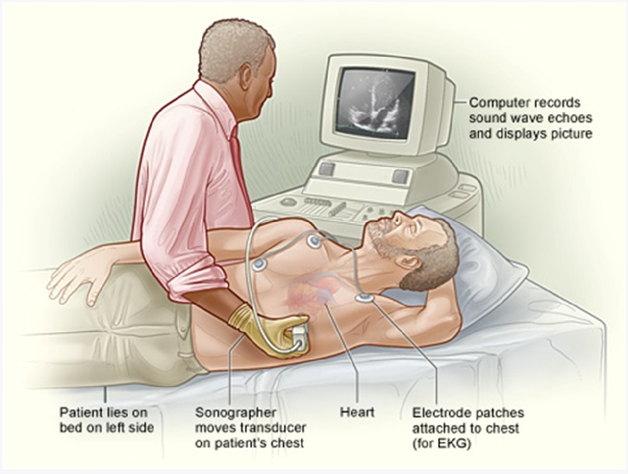
Transthoracic echocardiography is a diagnostic procedure that uses ultrasound to create images of the heart's structures and assess its function. It is a noninvasive test, meaning that it does not involve any insertion of instruments or devices into the body. Instead, a transducer is placed on the chest to obtain images of the heart.
The statement about managing pain aggressively during the procedure is not applicable to transthoracic echocardiography. It is generally a painless procedure that does not cause discomfort.
Transthoracic echocardiography primarily provides detailed images of the heart's structures and function, such as the chambers, valves, and pumping action. It does not specifically profile the heart's electrical activity, which is usually assessed using an electrocardiogram (ECG) or other specialized tests.
Regarding bed rest after the test, there is typically no need for bed rest following transthoracic echocardiography. The client can usually resume normal activities immediately after the procedure. However, the nurse should provide specific instructions based on the client's condition and any additional tests or interventions planned.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is D
Explanation
The client reports a headache with pain at level 5 of 10.: While a headache can be a symptom of high blood pressure, a pain level of 5 out of 10 alone does not indicate an immediate life-threatening condition. It is important to assess and manage the client's pain, but it may not be the most critical finding to report in this situation.
The client has epistaxis after blowing his nose several times. : Epistaxis, or a nosebleed, can occur due to high blood pressure, but it is not the most urgent or critical symptom in a hypertensive emergency. While it is essential to address the nosebleed and monitor blood pressure, other symptoms may indicate more severe consequences of uncontrolled high blood pressure.
The client has a urine output of 120 mL over 4 hours.: While decreased urine output can be a concerning sign, it is not the most significant finding to report in a hypertensive emergency. In this scenario, the focus is on acute complications related to high blood pressure, such as organ damage or impending stroke, which require immediate attention.
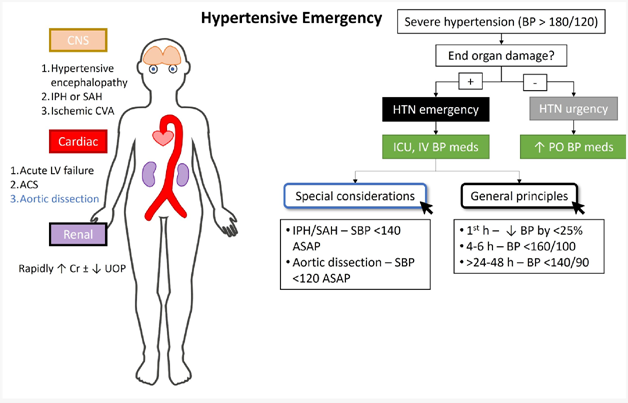
In summary, the finding that is most important to report to the healthcare provider in a client with a hypertensive emergency is the presence of new-onset blurry vision and facial asymmetry. These symptoms suggest potential neurological involvement and the need for urgent medical intervention to prevent serious complications like stroke.
Correct Answer is D
Explanation
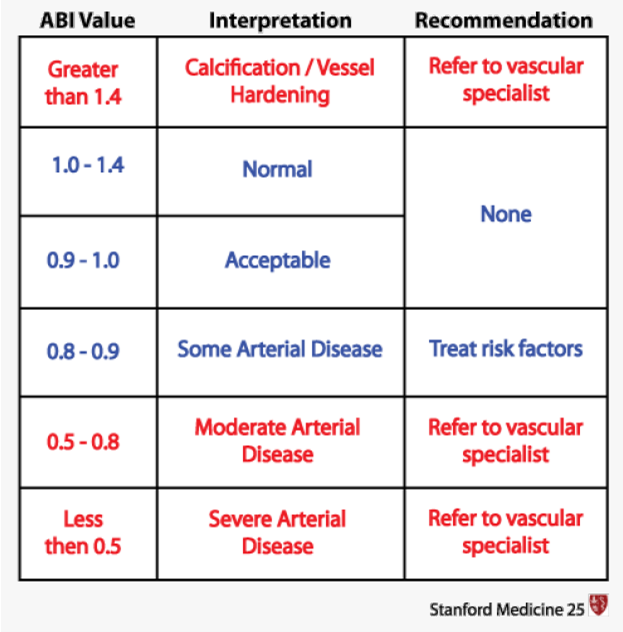
An ABI of 0.89 indicates a reduced blood flow to the lower extremities, which is suggestive of peripheral arterial disease (PAD). In PAD, there is narrowing or blockage of the arteries that supply blood to the legs and feet. Medications like clopidogrel and simvastatin are commonly prescribed for individuals with PAD to manage the condition and reduce the risk of complications.
Here's an explanation of why the other options are not the most appropriate interventions:
Document the information as a normal finding: An ABI of 0.89 is not considered a normal finding. An ABI value below 0.9 is generally indicative of PAD or reduced blood flow to the lower extremities.
Prepare the client for an arterial bypass: An ABI value of 0.89 alone does not warrant immediate preparation for an arterial bypass. Arterial bypass surgery is typically considered for severe cases of PAD with significant symptoms that significantly impact the client's quality of life and other conservative treatments have not been successful.
Educate the client about the use of compression stockings: While compression stockings may be a part of the overall management of PAD, the ABI result alone does not indicate an immediate need for education about compression stockings. Other interventions, such as medication management, lifestyle modifications, and possibly revascularization procedures, may be more appropriate based on the severity of the PAD.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
