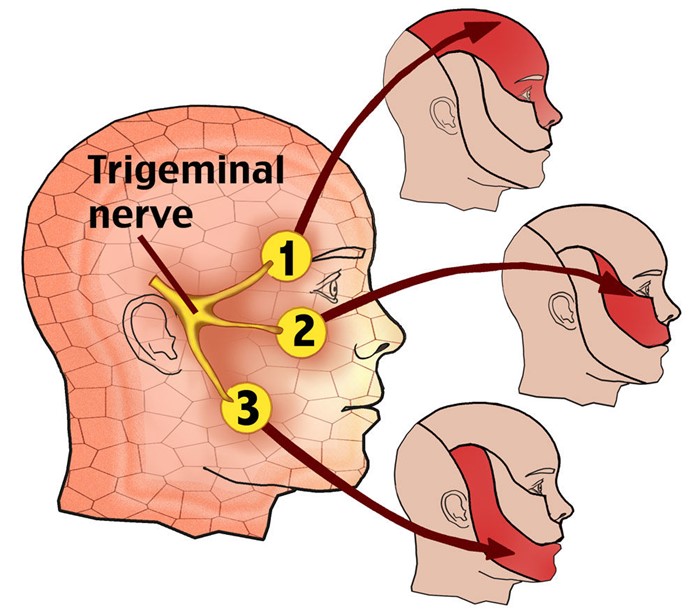
A client diagnosed with trigeminal neuralgia is experiencing intermittent, sudden, severe pain on the left side of the face. The nurse identifies which classification of medications is most effective in treating this pain.
Analgesics
Antihistamines
Antibiotics
Anticonvulsants
The Correct Answer is D
Choice A reason: Analgesics are medications that relieve pain by blocking pain signals or reducing inflammation. They include nonsteroidal anti-inflammatory drugs (NSAIDs), opioids, and acetaminophen. However, analgesics are not very effective in treating trigeminal neuralgia, as they do not address the underlying cause of the pain, which is the compression or irritation of the trigeminal nerve.
Choice B reason: Antihistamines are medications that block the effects of histamine, a chemical that causes allergic reactions such as itching, sneezing, and swelling. They include diphenhydramine, cetirizine, and loratadine. Antihistamines are not effective in treating trigeminal neuralgia, as they do not affect the trigeminal nerve or its function.
Choice C reason: Antibiotics are medications that kill or inhibit the growth of bacteria that cause infections. They include penicillin, amoxicillin, and ciprofloxacin. Antibiotics are not effective in treating trigeminal neuralgia, as they do not target the trigeminal nerve or its pathology.
Choice D reason: Anticonvulsants are medications that prevent or reduce the frequency and severity of seizures by stabilizing the electrical activity of the brain. They include carbamazepine, gabapentin, and phenytoin. Anticonvulsants are the most effective medications in treating trigeminal neuralgia, as they reduce the abnormal firing of the trigeminal nerve that causes the pain. Anticonvulsants are considered the first-line therapy for trigeminal neuralgia and can provide significant relief for most clients.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is C
Explanation
Choice A reason: Delivering a urine specimen to the laboratory is not a priority task, as it does not affect the client's immediate health or safety. This task can be done later or delegated to another staff member.
Choice B reason: Feeding a client who has bilateral casts is an important task, as it helps the client meet their nutritional needs and prevents complications such as pressure ulcers. However, this task is not as urgent as monitoring blood glucose levels, as it can be done within a reasonable time frame without causing harm to the client.
Choice C reason: Performing blood glucose monitoring of a client who has a prescription for short-acting insulin is a priority task, as it determines the dosage of insulin that the client needs to receive. Insulin is a high-alert medication that can cause serious adverse effects if given incorrectly. Therefore, this task should be done first by the AP who has been trained and certified to do so.
Choice D reason: Obtaining an extra box of tissues for a client who is concerned about running out of them is a low-priority task, as it does not affect the client's physical or psychological well-being. This task can be done at any time or delegated to another staff member.
Correct Answer is ["A","B","C","D"]
Explanation
Choice A reason: Nurses performing duties outside of the nurses' typical job description is a component that should include nurses. In a disaster situation, nurses may have to assume roles and responsibilities that are beyond their usual scope of practice, such as triage, first aid, or mass casualty management. Nurses should be trained and prepared to perform these duties safely and effectively.
Choice B reason: A plan for comprehensive practice drills is a component that should include nurses. Practice drills are essential for testing and improving the disaster plan, as well as enhancing the skills and confidence of the staff. Nurses should participate in regular and realistic drills that simulate different types of disasters and scenarios.
Choice C reason: Identification of resources to meet anticipated needs for food, water, and supplies is a component that should include nurses. In a disaster situation, the demand for resources may exceed the supply, and the availability of resources may be disrupted or limited. Nurses should be involved in identifying and prioritizing the essential resources that are needed to provide care and support to the clients and staff.
Choice D reason: An internal and external communication plan is a component that should include nurses. In a disaster situation, communication is vital for coordinating actions, sharing information, and providing updates. Nurses should be aware of the communication channels and protocols that are used within and outside the hospital, such as radios, phones, or social media.
Choice E reason: Discharge all surgical clients who are one day or more post-op is not a component that should include nurses. This is not a realistic or appropriate strategy for reducing the hospital's occupancy or workload in a disaster situation. Discharging surgical clients who are still recovering may compromise their health outcomes and increase their risk of complications or readmission.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
