Here is the edited text:
A nurse is caring for a client who has a traumatic brain injury. The nurse notes that the client has a widening pulse pressure. Which of the following actions should the nurse take?
Administer a vasodilator medication.
Elevate the head of the bed to 30°.
Apply a cold compress to the forehead.
Decrease the oxygen flow rate.
The Correct Answer is B
Choice A Reason: This choice is incorrect because administering a vasodilator medication may lower the blood pressure and worsen the cerebral perfusion. A vasodilator medication is a drug that relaxes the blood vessels and reduces the resistance to blood flow. It may be used for clients who have hypertension, angina, or heart failure, but it does not help to reduce the intracranial pressure (ICP).
Choice B Reason: This choice is correct because elevating the head of the bed to 30° may help to improve the venous drainage and decrease the ICP. ICP is the pressure exerted by the brain tissue, cerebrospinal fluid (CSF), and blood within the cranial cavity. A normal ICP range is 5 to 15 mm Hg, and an elevated ICP (>20 mm Hg) can cause cerebral ischemia, herniation, or death. Therefore, positioning the client in a semi-Fowler's position (30° angle) or high- Fowler's position (60° to 90° angle) can facilitate breathing and prevent further complications.
Choice C Reason: This choice is incorrect because applying a cold compress to the forehead may cause vasoconstriction and increase the ICP. A cold compress is a device that applies cold temperature to a body part to reduce inflammation, pain, or swelling. It may be used for clients who have headaches, sprains, or bruises, but it does not help to reduce the ICP.
Choice D Reason: This choice is incorrect because decreasing the oxygen flow rate may cause hypoxia and worsen the cerebral ischemia. Hypoxia is a condition in which the body or a part of it does not receive enough oxygen. It may cause symptoms such as confusion, agitation, or cyanosis. Therefore, providing adequate oxygenation and ventilation is essential to maintain the brain function and prevent further damage.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
Choice A Reason: Packed RBCs are indicated for clients who have hypovolemic shock due to blood loss, as they increase the oxygen-carrying capacity of the blood and restore the blood volume.
Choice B Reason: Cryoprecipitates are indicated for clients who have hemophilia or von Willebrand disease, as they contain clotting factors that help stop bleeding.
Choice C Reason: Albumin is indicated for clients who have hypovolemic shock due to fluid loss, such as from burns or ascites, as it increases the plasma oncotic pressure and draws fluid into the vascular space.
Choice D Reason: Platelets are indicated for clients who have thrombocytopenia or platelet dysfunction, as they help prevent or control bleeding.
Correct Answer is A
Explanation
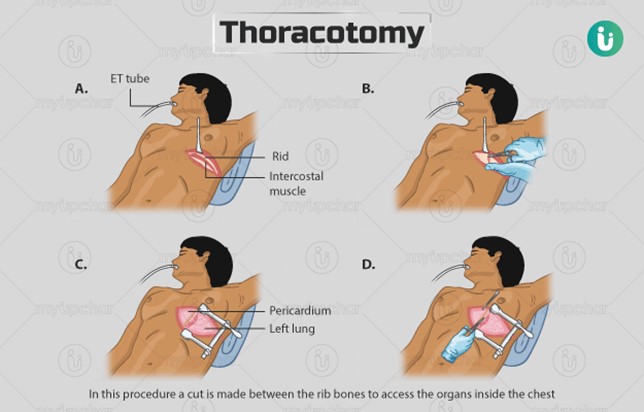
Choice A Reason: This choice is correct because slow, steady bubbling in the suction control chamber indicates that the suction is working properly and maintaining a negative pressure in the pleural space. The nurse should continue to monitor the client's respiratory status, such as breath sounds, oxygen saturation, and respiratory rate, to assess the effectiveness of the chest drainage system.
Choice B Reason: This choice is incorrect because checking the suction control outlet on the wall is not necessary unless there is no bubbling in the suction control chamber, which would indicate a problem with the suction source or setting. The nurse should ensure that the suction control outlet is set at the prescribed level, usually between 10 and 20 cm H2O.
Choice C Reason: This choice is incorrect because clamping the chest tube is not indicated unless there is a leak in the system or the chest drainage unit needs to be changed. Clamping the chest tube may cause a buildup of air or fluid in the pleural space, which can lead to tension pneumothorax or pleural effusion.
Choice D Reason: This choice is incorrect because checking the tubing connections for leaks is not necessary unless there is continuous bubbling in the water seal chamber, which would indicate an air leak in the system. The nurse should ensure that all tubing connections are tight and secure, and tape any loose connections.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
