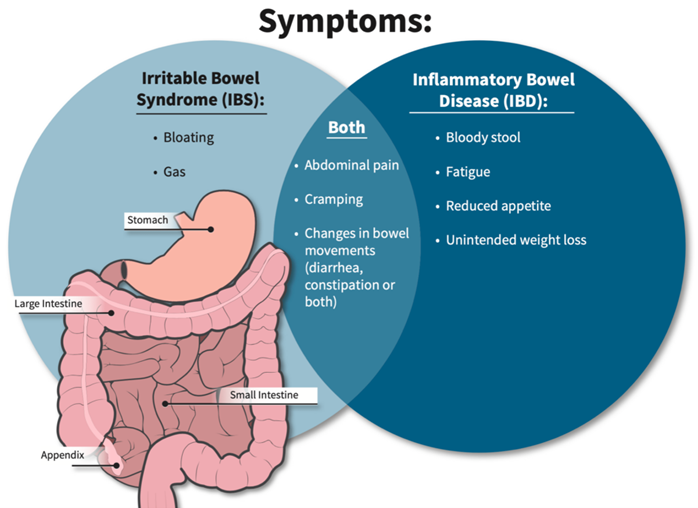
A nurse provides education to a client diagnosed with inflammatory bowel syndrome (IBS) about measures to treat diarrhea caused by acute flare-ups. Which statement by the client indicates a need for further teaching?
"I will eat frequent small meals."
"I will increase the intake of leafy greens and other sources of dietary fiber."
"I will increase fluids."
"I will take prescribed medications on schedule to regulate bowel patterns."
The Correct Answer is B
Choice A reason: This is correct because eating frequent small meals can help the client with IBS to avoid overloading the digestive system and triggering diarrhea. The nurse should advise the client to eat slowly chew well, and avoid foods that are spicy, fatty, or gas-producing.
Choice B reason: This is incorrect because increasing the intake of leafy greens and other sources of dietary fiber can worsen diarrhea by increasing stool bulk and motility. The nurse should advise the client to limit or avoid high-fiber foods, such as whole grains, fruits, vegetables, nuts, and seeds, during acute flare-ups of IBS. The client can gradually reintroduce fiber when the symptoms subside.
Choice C reason: This is correct because increasing fluids can help the client with IBS to prevent dehydration and electrolyte imbalance caused by diarrhea. The nurse should advise the client to drink at least 8 glasses of water per day and avoid caffeinated, alcoholic, or carbonated beverages that can irritate the bowel or cause gas.
Choice D reason: This is correct because taking prescribed medications on schedule can help the client with IBS to regulate bowel patterns and reduce diarrhea. The nurse should instruct the client on how to use medications, such as antidiarrheals, antispasmodics, or probiotics, as ordered by the provider. The nurse should also monitor the client for any adverse effects or interactions of the medications.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is ["B","D","F"]
Explanation
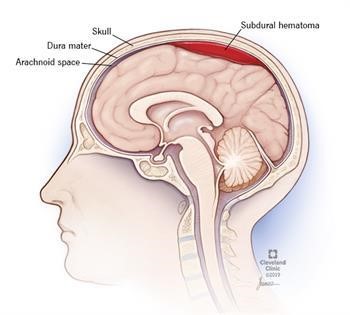
Choice A Reason: Slow even breathing is not a sign of Cushing's Triad, which is a late indicator of increased intracranial pressure (ICP). The breathing pattern may be altered due to brainstem compression, but not necessarily slow or even.
Choice B Reason: This is a correct answer because bradycardia and bounding pulse are part of Cushing's Triad, which reflects an increased vagal tone and decreased cardiac output due to increased ICP.
Choice C Reason: Systolic hypotension with a narrowing pulse pressure is not a sign of Cushing's Triad, which involves an increased systolic blood pressure and a widened pulse pressure due to increased ICP. Hypotension may occur due to shock or hemorrhage, but not as a result of increased ICP.
Choice D Reason: This is a correct answer because irregular respirations are part of Cushing's Triad, which reflects impaired respiratory control due to brainstem compression from increased ICP. The respirations may be Cheyne-Stokes, central neurogenic hyperventilation, apneustic, or ataxic.
Choice E Reason: Tachycardia and bounding pulse are not signs of Cushing's Triad, which involves bradycardia and bounding pulse due to increased ICP. Tachycardia may occur due to pain, anxiety, fever, or hypoxia, but not as a result of increased ICP.
Choice F Reason: This is a correct answer because systolic hypertension with a widening pulse pressure are part of Cushing's Triad, which reflects an increased cerebral perfusion pressure due to increased ICP. The diastolic blood pressure remains stable or decreases, resulting in a widened pulse pressure.
Correct Answer is D
Explanation
Choice A Reason: A facial tumor is not related to Guillain-Barre syndrome, which is an autoimmune disorder that affects the peripheral nerves.
Choice B Reason: Pregnancy is not a risk factor for Guillain-Barre syndrome, although it can occur during or after pregnancy in rare cases.
Choice C Reason: A puncture wound 3 weeks ago is unlikely to cause Guillain-Barre syndrome, which usually follows a respiratory or gastrointestinal infection.
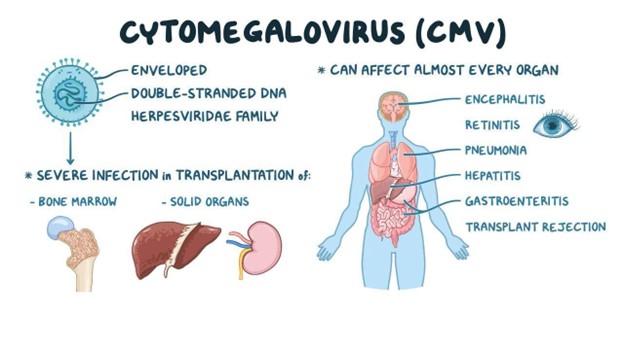
Choice D Reason: This is the correct answer because cytomegalovirus is one of the common infections that can trigger Guillain-Barre syndrome. It can cause inflammation and damage to the myelin sheath that covers the nerves.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
