A nurse is planning care for a child who has epiglottitis. Which of the following actions should the nurse plan to take?
Obtain a throat culture.
Visualize the epiglottis using a tongue depressor.
Provide moist air to reduce the inflammation of the epiglottis
Initiate airborne precautions.
The Correct Answer is C
A. Obtain a throat culture.
This option is not appropriate as a primary nursing action in the acute management of epiglottitis. While obtaining a throat culture may be necessary for diagnostic purposes, it is not a priority in the immediate care of a child with suspected epiglottitis. The focus should be on ensuring airway patency and providing emergency treatment.
B. Visualize the epiglottis using a tongue depressor.
This option is contraindicated in the acute management of epiglottitis. Direct visualization of the epiglottis using a tongue depressor or other instruments can provoke spasm of the epiglottis and worsen airway obstruction. Attempting to visualize the epiglottis should be avoided until the child's airway has been secured in a controlled environment, such as in the operating room under anesthesia.
C. Provide moist air to reduce the inflammation of the epiglottis.
This option is appropriate. Providing moist air, such as humidified oxygen or a cool mist, can help soothe the inflamed tissues of the epiglottis and upper airway. Moist air may help alleviate discomfort and reduce inflammation, although it will not directly address the risk of airway obstruction. It is often used as supportive therapy in conjunction with other interventions.
D. Initiate airborne precautions.
This option is not necessary for the care of a child with epiglottitis. Epiglottitis is not typically transmitted through airborne droplets. The priority in the management of epiglottitis is ensuring a patent airway and providing appropriate treatment to reduce inflammation and prevent complications.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
A. "At this age you should expect your child to be upset when you leave.": This statement provides normalcy to the parents' experience and reassures them that their child's reaction is typical for his age. It acknowledges the child's developmental stage and separation anxiety, helping to alleviate parental concerns.
B. "Your child needs to rest.": While rest is important for infants, this statement does not address the child's emotional needs or the parents' concerns about leaving their child. It may also minimize the significance of the child's distress.
C. "I will notify the provider of his behavior.": Notifying the healthcare provider may be appropriate if the child's distress continues or if there are concerns about the child's well-being, but this statement does not directly address the parents' concerns or provide guidance on how to manage the situation.
D. "Your child is responding to an overstimulating environment.": This statement suggests a possible cause for the child's distress but does not provide guidance or reassurance to the parents on how to address the situation or manage their child's reaction.
Correct Answer is C
Explanation
A. Respiratory
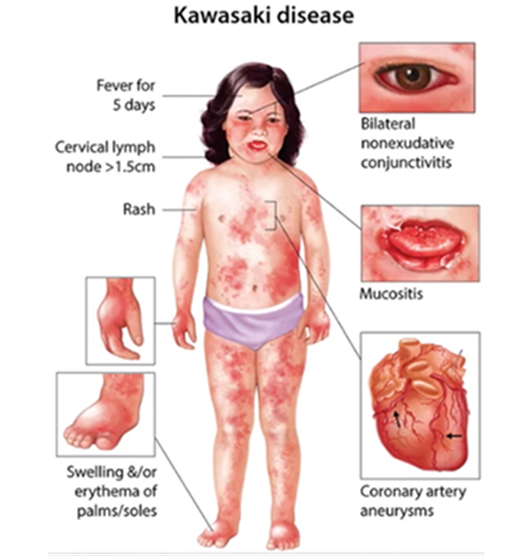
Kawasaki disease primarily affects the cardiovascular system rather than the respiratory system. While respiratory symptoms such as cough or congestion may occur in some cases, they are not the primary focus of the disease.
B. Gastrointestinal
Although gastrointestinal symptoms such as abdominal pain, vomiting, or diarrhea can occur in Kawasaki disease, they are not the primary system affected. Gastrointestinal symptoms are considered part of the systemic manifestations of the disease but do not define its primary pathology.
C. Cardiovascular
This is the correct answer. Kawasaki disease primarily affects the cardiovascular system. It is characterized by inflammation of the blood vessels, particularly the medium-sized arteries, including the coronary arteries. Coronary artery involvement can lead to coronary artery aneurysms and other cardiovascular complications, making the cardiovascular system the primary focus of the disease.
D. Integumentary
The integumentary system (skin) is not primarily affected by Kawasaki disease. While changes in the skin, such as a rash, may occur as part of the systemic manifestations of the disease, they are not the primary focus of Kawasaki disease.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
