A nurse is completing an admission assessment of a client. Which of the following findings should the nurse identify as a stage 2 pressure injury?
A defined area of cool, boggy skin.
A shallow crater involving the epidermis.
Reddened area that does not blanch.
Undermining or tunneling of the skin.
The Correct Answer is B
Choice A rationale:
A defined area of cool, boggy skin is not indicative of a stage 2 pressure injury. Stage 2 pressure injuries involve partial-thickness skin loss, usually appearing as a shallow open ulcer with a red-pink wound bed, without slough or bruising.
Choice B rationale:
A shallow crater involving the epidermis is characteristic of a stage 2 pressure injury. It presents as a partial-thickness skin loss with the loss of the epidermis, and the wound may be superficial and appear as an abrasion, blister, or shallow ulcer.
Choice C rationale:
The reddened area that does not blanch is more indicative of an early-stage pressure injury (Stage 1). In Stage 1, the skin remains intact, but there is non-blanch-able erythema indicating damage to the skin and underlying tissue.
Choice D rationale:
Undermining or tunneling of the skin is not specific to stage 2 pressure injuries. These features may be observed in more advanced stages of pressure injuries, such as stages 3 and 4, where there is full-thickness skin loss with damage to the subcutaneous tissue and underlying structures.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is C
Explanation
Choice A rationale:
Difficulty maintaining personal hygiene is not typically an early indication of mild Alzheimer's disease. In the early stages, individuals can still manage personal hygiene.
Choice B rationale:
Difficulty handling finances may occur in the later stages of Alzheimer's disease, but it is not an early indication. In the early stages, the person might still manage financial matters.
Choice C rationale:
Difficulty remembering the names of new friends is a common early sign of mild Alzheimer's disease. It reflects the impairment of short-term memory that often occurs in the early stages of the disease.
Choice D rationale:
Difficulty driving to and from familiar places is more likely to be a mid-to-late-stage symptom of Alzheimer's disease. In the early stages, individuals might still drive familiar routes with minimal difficulty.
Correct Answer is A
Explanation
Choice A rationale:
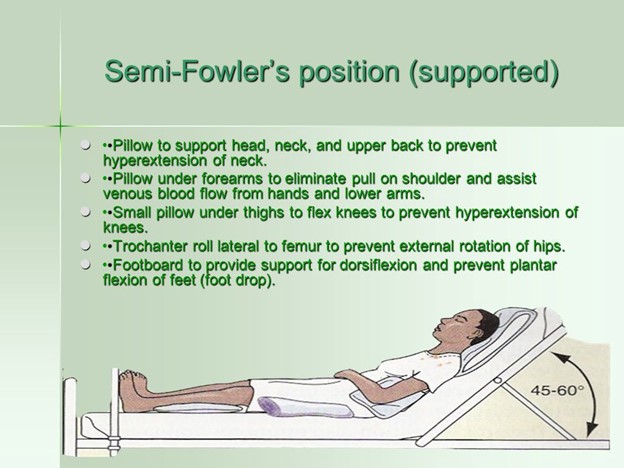
The nurse should maintain the client in a semi-Fowler's position to promote comfort and reduce the risk of complications related to appendicitis. This position helps to decrease pressure on the abdomen and may alleviate pain by reducing tension on the abdominal muscles.
Choice B rationale:
Administering an enema 1 hour prior to surgery is not indicated for a client with appendicitis. Enemas are generally not recommended for clients with suspected or confirmed appendicitis as they can potentially worsen inflammation and cause perforation of the inflamed appendix.
Choice C rationale:
Applying a warm pack to the client's lower abdomen is contraindicated in appendicitis. Heat can exacerbate inflammation and should be avoided in such cases.
Choice D rationale:
Placing the client on a clear liquid diet is not appropriate for appendicitis. Clients with appendicitis are typically NPO (nothing by mouth) to avoid stimulating the gastrointestinal tract and reduce the risk of rupture if surgery is needed.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
