A nurse is collecting data about the fluid status of four patients.
Which patient should the nurse identify as being at risk for fluid volume deficit?
A patient who has heart failure and is receiving diuretic therapy.
A patient who has gastroenteritis and is receiving oral fluids.
A patient who has end-stage kidney disease who will undergo dialysis.
A patient who has NPO status since midnight for an endoscopy.
The Correct Answer is D
Rationale for Choice A:
Diuretics promote fluid loss, increasing the risk of fluid volume deficit.
Heart failure can lead to fluid retention, but diuretic therapy is often used to manage this excess fluid.
However, in this case, the patient is receiving diuretic therapy, which suggests that their fluid status is being actively managed.
Therefore, while this patient is at risk for fluid volume deficit, they are not the most likely candidate among the options presented.
Rationale for Choice B:
Gastroenteritis can lead to fluid loss through vomiting and diarrhea.
However, this patient is receiving oral fluids, which helps to replenish lost fluids and electrolytes.
As long as the patient is able to tolerate oral fluids and is not experiencing excessive fluid losses, they are not at significant risk for fluid volume deficit.
Rationale for Choice C:
End-stage kidney disease can impair the kidneys' ability to regulate fluid balance.
However, dialysis is a treatment that helps to remove excess fluid and waste products from the body.
Therefore, while this patient is at risk for fluid volume imbalances, they are receiving treatment to manage this risk.
Rationale for Choice D:
NPO status means that the patient has been instructed to have nothing by mouth. This means that the patient has not been able to consume any fluids since midnight.
Even in the absence of excessive fluid losses, this prolonged period of fluid restriction can lead to dehydration and fluid volume deficit.
Therefore, this patient is the most likely to be experiencing fluid volume deficit among the options presented.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
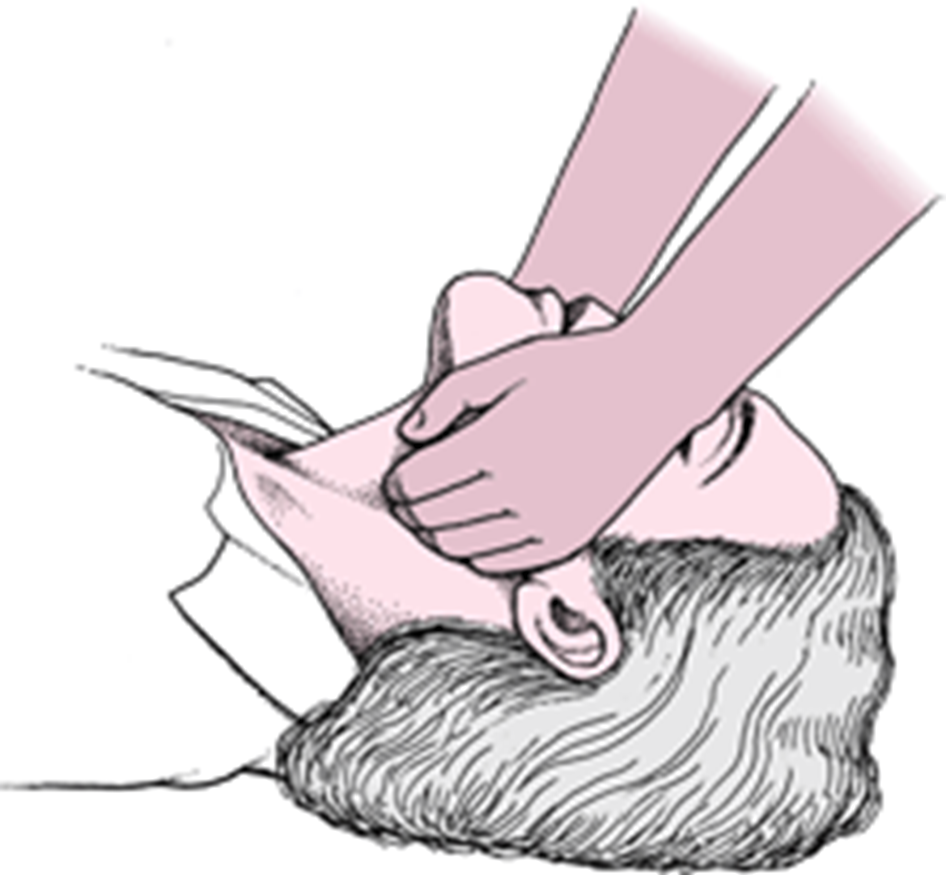
Establishing an open airway is the most crucial and immediate action in any respiratory arrest situation, including when a client has heart failure. Here's a detailed explanation: 1. Airway patency is paramount for survival: Oxygen, the essential element for life, cannot reach the lungs and bloodstream without a clear and unobstructed airway. Brain cells are extremely sensitive to oxygen deprivation and start to die within minutes without it, leading to irreversible brain damage or death. 2. Respiratory arrest in heart failure: Heart failure often leads to fluid buildup in the lungs (pulmonary edema), which can significantly impair breathing. Respiratory arrest can occur due to: Excessive fluid accumulation in the lungs. Weakening of respiratory muscles due to fatigue or heart failure itself. Arrhythmias or heart blocks affecting heart's ability to pump effectively. 3. Steps to establish an open airway: Head tilt-chin lift maneuver: Gently tilt the head back and lift the chin to open the airway. Jaw thrust maneuver: If a neck injury is suspected, use the jaw thrust maneuver to avoid further injury. Removal of any visible obstructions: Clear any visible foreign objects or fluids from the mouth or throat. Use of airway adjuncts: Consider using oral or nasal airways to maintain airway patency, especially if the patient is unconscious.
4. Rationale for other choices:
A. Auscultating for breath sounds: While important for assessment, it does not address the immediate need to establish airflow.
C. Establishing IV access: IV access is necessary for medications and fluids, but airway takes priority in respiratory arrest.
D. Feeling for a carotid pulse: Checking for a pulse is essential, but only after ensuring an open airway and attempting to restore breathing.
5. Importance of prioritizing airway: Establishing an open airway allows for potential rescue breaths and ventilation, which can help restore oxygen levels and prevent further deterioration. Even if a pulse is present, without a clear airway, oxygen cannot reach the vital organs, leading to organ failure and death.
Correct Answer is B
Explanation
Choice B rationale:
Checking the patency of the tubing is the first and most crucial step in addressing the lack of urinary output in this patient. Here's a detailed explanation of why this is the priority action:
Addresses the Most Likely Cause: Obstruction of the urinary catheter tubing is the most common and easily reversible cause of sudden cessation of urinary output in a patient with a continuous bladder irrigation system.
Prevents Complications: A blocked catheter can lead to a number of serious complications, including: Bladder distention, which can cause pain, discomfort, and potential bladder damage.
Urinary retention, which can increase the risk of urinary tract infections (UTIs) and kidney damage. Hematuria, or blood in the urine, due to clot formation in the bladder or catheter.
Non-Invasive Intervention: Checking the tubing is a simple, non-invasive procedure that can quickly identify and resolve the issue without requiring further interventions or delays in care.
Prioritizes Patient Safety: It's essential to promptly address any potential urinary obstruction to prevent the aforementioned complications and ensure patient safety.
Rationale for Other Choices:
Choice A: Administering a prescribed analgesic:
While pain management is important, it does not directly address the lack of urinary output. Pain medication would be appropriate if pain were assessed to be the cause of the decreased output, but it's not the first priority in this situation.
Choice C: Notifying the provider:
Although the provider should be informed of the situation, checking the tubing for patency is a necessary first step to gather more information and potentially resolve the issue quickly without requiring further intervention.
Choice D: Offering oral fluids:
Increasing fluid intake might be helpful in some cases of decreased urinary output, but it's not the priority action in a patient with a continuous bladder irrigation system and a potential catheter obstruction.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
