A nurse is caring for a client who has pericarditis and reports feeling a new onset of palpitations and shortness of breath. Which of the following assessments should indicate to the nurse that the client may have developed atrial fibrillation?
Different blood pressures in the upper limbs.
Differences in upper and lower lung sounds.
Differences between oral and axillary temperatures.
Different apical and radial pulses.
The Correct Answer is D
D. Atrial fibrillation can lead to irregular and often rapid heart rates, resulting in discrepancies between the apical (heart) and radial (peripheral) pulses. In atrial fibrillation, the atria fibrillate instead of contracting effectively, leading to irregular and sometimes asynchronous ventricular contractions. This irregularity may result in a pulse deficit, where the number of apical beats exceeds the number of radial pulses felt at the wrist.
A. Different blood pressures in the upper limbs may indicate conditions such as aortic dissection or arterial stenosis, but they are not typically associated with atrial fibrillation. Atrial fibrillation primarily affects the heart rhythm rather than blood pressure distribution.
B. Differences in upper and lower lung sounds may indicate conditions such as pneumonia or pleural effusion, but they are not specific to atrial fibrillation. Atrial fibrillation primarily affects the heart's electrical activity rather than respiratory findings.
C. Differences between oral and axillary temperatures may indicate localized variations in temperature, such as infection or inflammation, but they are not specific to atrial fibrillation. Atrial fibrillation primarily affects cardiac rhythm rather than body temperature regulation.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is D
Explanation
D. Asystole represents the absence of electrical activity in the heart and is not amenable to defibrillation. Therefore, the RRT would continue cardiopulmonary resuscitation (CPR) with chest compressions and may administer medications or other interventions as indicated. This statement provides accurate information to the family about the patient's condition and the actions being taken by the RRT.
A. Defibrillation is not indicated for asystole. Asystole represents a flatline on the cardiac monitor, indicating the absence of electrical activity in the heart. Defibrillation is only effective for certain types of cardiac rhythms, such as ventricular fibrillation or pulseless ventricular tachycardia. Therefore, the RRT would not use defibrillation for a patient in asystole.
B. It does not provide the family with information about the patient's condition or the actions being taken by the RRT. Moreover, excluding the family from the patient's care may cause additional distress and prevent them from being present to support their loved one during a critical situation.
C. Cardiopulmonary resuscitation (CPR) is performed to maintain blood flow and oxygenation to vital organs during cardiac arrest. However, it does not restore normal blood flow or circulation. The goal of CPR is to provide temporary support until advanced interventions can be initiated or until return of spontaneous circulation (ROSC) is achieved.
Correct Answer is B
Explanation
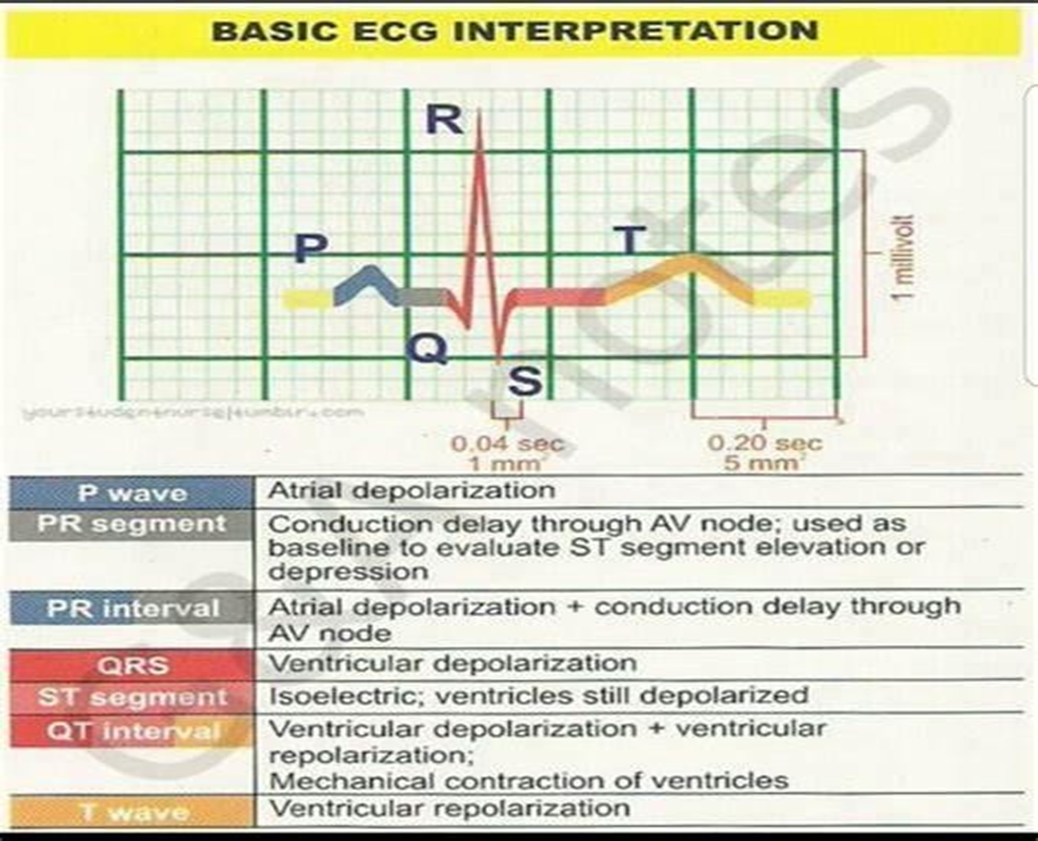
B. The QT interval represents ventricular depolarization and repolarization. It starts at the beginning of the QRS complex and ends at the end of the T wave. The QT interval reflects the total time it takes for both ventricular depolarization and repolarization to occur. Prolongation of the QT interval can be associated with an increased risk of arrhythmias, including torsades de pointes.
A. The QRS complex represents ventricular depolarization, which is the electrical activation of the ventricles. The duration of the QRS complex provides information about the time it takes for ventricular depolarization to occur. A prolonged QRS complex can indicate abnormalities in ventricular conduction, such as bundle branch blocks or ventricular hypertrophy.
C. The ST segment represents the early part of ventricular repolarization. It starts at the end of the QRS complex and ends at the beginning of the T wave. Changes in the ST segment, such as elevation or depression, can indicate myocardial ischemia or injury.
D. The PR interval represents the time it takes for the electrical impulse to travel from the atria to the ventricles. It includes atrial depolarization, atrial contraction, and the delay at the atrioventricular node. The PR interval does not specifically provide information about ventricular depolarization and repolarization.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
