A nurse is assisting with the care of a client who is 1 day postoperative following a thyroidectomy and reports severe muscle spasms of the lower extremities. Which of the following actions should the nurse take?
Determine the client’s calcium level.
Give the client an oral potassium supplement.
Administer intravenous normal saline solution.
Monitor the client’s peripheral pulses.
The Correct Answer is A
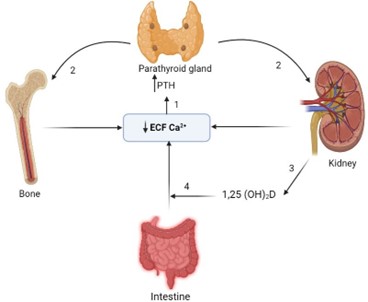
Choice A: Determine the client’s calcium level. This is the priority action for the nurse to take because the client might have hypocalcemia, which is a low level of calcium in the blood. Hypocalcemia can occur after a thyroidectomy due to accidental removal or damage of the parathyroid glands, which regulate calcium levels. Hypocalcemia can cause muscle spasms, tetany, paresthesia, and seizures.
Choice B: Give the client an oral potassium supplement. This is not an appropriate action for the nurse to take because the client might have hyperkalemia, which is a high level of potassium in the blood. Hyperkalemia can also occur after a thyroidectomy due to damage to the adrenal glands, which regulate potassium levels. Hyperkalemia can cause muscle weakness, arrhythmias, and cardiac arrest.
Choice C: Administer intravenous normal saline solution. This is not a necessary action for the nurse to take because the client does not have signs of dehydration or fluid imbalance. Normal saline solution does not affect calcium or potassium levels.
Choice D: Monitor the client’s peripheral pulses. This is an important action for the nurse to take, but not the priority. The nurse should monitor the client’s peripheral pulses for signs of decreased perfusion or ischemia, which can result from hypocalcemia or hyperkalemia affecting the cardiac function. However, this should be done after determining the client’s calcium level and correcting it if needed.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is D
Explanation
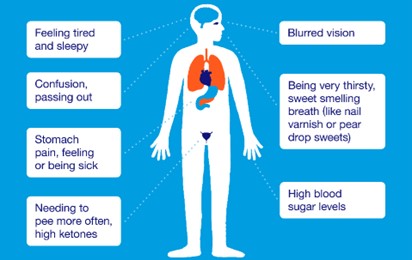
Choice A: Rapid pulse. This is not a finding that indicates that the client is experiencing DKA, but rather a sign of hypoglycemia, which is a low level of glucose in the blood. Hypoglycemia can cause rapid pulse due to increased sympathetic nervous system activity and decreased cardiac output.
Choice B: Clammy skin. This is not a finding that indicates that the client is experiencing DKA, but rather a sign of hypoglycemia. Hypoglycemia can cause clammy skin due to increased sweating and vasoconstriction.
Choice C: Choice C: Confusion is commonly found in HHS rather than DKA.
Choice D: Polydipsia. This is a finding that indicates that the client is experiencing DKA due to the high level of glucose in the blood. Hyperglycemia in DKA can cause polydipsia, which is excessive thirst, due to osmotic diuresis and dehydration.
Correct Answer is A
Explanation
Choice A: Determine the client’s calcium level. This is the priority action for the nurse to take because the client might have hypocalcemia, which is a low level of calcium in the blood. Hypocalcemia can occur after a thyroidectomy due to accidental removal or damage of the parathyroid glands, which regulate calcium levels. Hypocalcemia can cause muscle spasms, tetany, paresthesia, and seizures.
Choice B: Give the client an oral potassium supplement. This is not an appropriate action for the nurse to take because the client might have hyperkalemia, which is a high level of potassium in the blood. Hyperkalemia can also occur after a thyroidectomy due to damage to the adrenal glands, which regulate potassium levels. Hyperkalemia can cause muscle weakness, arrhythmias, and cardiac arrest.
Choice C: Administer intravenous normal saline solution. This is not a necessary action for the nurse to take because the client does not have signs of dehydration or fluid imbalance. Normal saline solution does not affect calcium or potassium levels.
Choice D: Monitor the client’s peripheral pulses. This is an important action for the nurse to take, but not the priority. The nurse should monitor the client’s peripheral pulses for signs of decreased perfusion or ischemia, which can result from hypocalcemia or hyperkalemia affecting the cardiac function. However, this should be done after determining the client’s calcium level and correcting it if needed.

Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
