A nurse is assisting with the care of a client who had an epidural anesthesia block during the early stages of labor. The client's blood pressure is 80/40 mm Hg and the fetal heart recording is 140/min. Which of the following actions should the nurse take first?
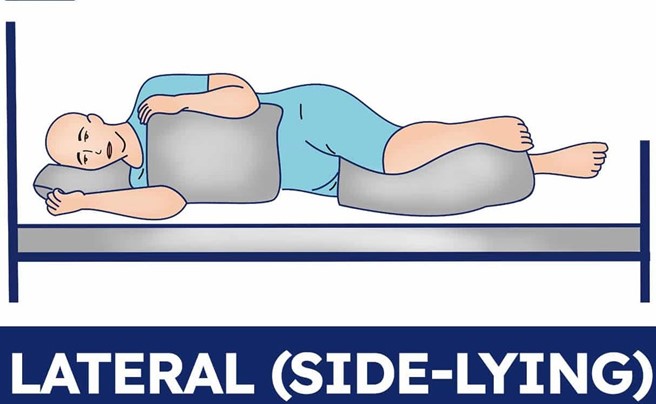
Place the client in a lateral position.
Notify the provider.
Increase IV fluid rate.
Elevate the legs.
The Correct Answer is A
Choice A reason:
Placing the client in a lateral position is the first action the nurse should take, as it can improve maternal and fetal circulation by relieving pressure on the inferior vena cava. The client's blood pressure is low, which can indicate hypotension due to epidural anesthesia or supine hypotension syndrome.
Choice B reason:
Notifying the provider is an important action, as it can facilitate further interventions and monitoring for the client and the fetus. However, this is not the first action the nurse should take, as it does not address the immediate problem of hypotension.
Choice C reason:
Increasing IV fluid rate is an important action, as it can expand blood volume and increase blood pressure. However, this is not the first action the nurse should take, as it may not be effective if the client is in a supine position.
Choice D reason:
Elevating the legs is an important action, as it can enhance venous return and increase blood pressure. However, this is not the first action the nurse should take, as it may worsen supine hypotension syndrome by increasing pressure on the inferior vena cava.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is D
Explanation
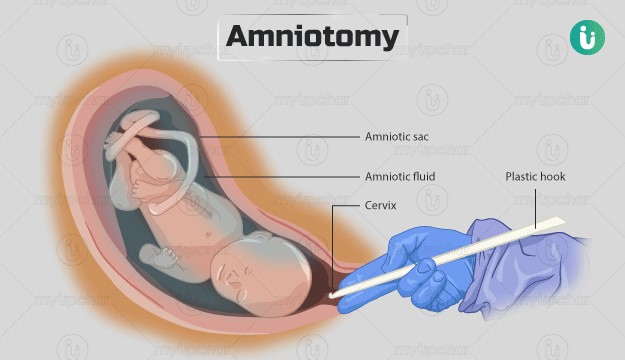
Choice A reason: Check the client's temperature every 4 hr is incorrect, as this action is not frequent enough for a client who had an amniotomy. The nurse should check the client's temperature every 2 hr after an amniotomy, as there is an increased risk of infection due to the rupture of membranes. The nurse should also monitor for signs of chorioamnionitis, such as foul-smelling amniotic fluid, maternal tachycardia, or fetal tachycardia.
Choice B reason: Remind the client to bear down with each contraction is incorrect, as this action is not appropriate for a client who is in the active phase of the first stage of labor. The nurse should instruct the client to avoid bearing down or pushing until they are in the second stage of labor, when the cervix is fully dilated and effaced. Bearing down too early can cause cervical edema, lacerations, or exhaustion.
Choice C reason: Maintain the client in the lithotomy position is incorrect, as this action is not optimal for a client who is in the active phase of the first stage of labor. The lithotomy position is a supine position with the legs elevated and abducted, which can reduce blood flow to the uterus and placenta, increase perineal edema, and limit pelvic outlet diameter. The nurse should encourage the client to change positions frequently and use upright or lateral positions that can enhance uterine contractility, fetal descent, and maternal comfort.
Choice D reason: Encourage the client to empty the bladder every 2 hr is correct, as this action can promote labor progress and prevent bladder distension and infection. The nurse should assist the client to void every 2 hr after an amniotomy, as there may be decreased sensation of bladder fullness due to pressure from the fetal head. A full bladder can interfere with uterine contractions, fetal descent, and cervical dilation.
Correct Answer is A
Explanation
Choice A reason: Fundal consistency is correct, as this finding can indicate the effectiveness of oxytocin in stimulating uterine contraction and preventing postpartum hemorrhage. Oxytocin is a uterotonic agent that can enhance or augment uterine contractility and involution. The nurse should monitor the fundal height, consistency, and position and report any signs of uterine atony or excessive bleeding.
Choice B reason: Fetal heart rate is incorrect, as this finding is not relevant for a client who has already delivered the baby. Fetal heart rate can indicate the fetal well-being and response to labor, but it is not affected by oxytocin administration after birth. The nurse should monitor the newborn's vital signs and appearance and report any signs of distress or infection.
Choice c reason: Urinary output is incorrect, as this finding is not specific for evaluating the effectiveness of oxytocin. Urinary output can indicate the client's renal function and fluid balance, but it can be influenced by many other factors, such as fluid intake, bladder distension, or epidural anesthesia. The nurse should monitor the client's intake and output and report any signs of oliguria or retention.
Choice D reason: Blood pressure is incorrect, as this finding is not specific for evaluating the effectiveness of oxytocin. Blood pressure can indicate the client's hemodynamic status and response to blood loss, but it can be influenced by many other factors, such as pain, anxiety, preeclampsia, or medication. The nurse should monitor the client's vital signs and fluid balance and report any signs of hypotension or hypertension
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
