A nurse is assessing a client with intermittent claudication. What client statement supports this information?
"My feet feel like I have pins and needles."
"When I stand or sit too long, my feet swell."
"My legs get a painful cramp when I walk over 30 minutes."
"I get short of breath when I climb a lot of stairs.”
The Correct Answer is C
The client statement that supports the information of intermittent claudication is: "My legs get a painful cramp when I walk over 30 minutes.": Intermittent claudication is a symptom of peripheral artery disease (PAD) characterized by pain, cramping, or fatigue in the muscles of the lower extremities, typically the calves, thighs, or buttocks. This pain is usually triggered by physical activity, such as walking, and is relieved with rest. The pain is caused by inadequate blood flow and oxygen supply to the muscles due to narrowed or blocked arteries.
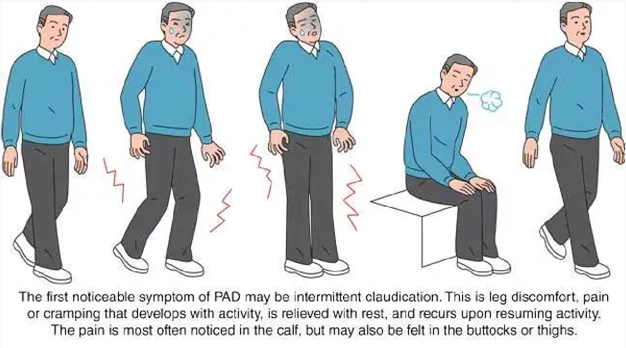
The other client statements do not specifically indicate intermittent claudication:
"My feet feel like I have pins and needles": This sensation of pins and needles is often associated with peripheral neuropathy, which is a condition involving nerve damage and does not directly relate to intermittent claudication.
"When I stand or sit too long, my feet swell": This statement suggests the possibility of venous insufficiency rather than intermittent claudication. Venous insufficiency involves impaired blood return from the legs to the heart and may result in swelling, aching, or heaviness in the legs.
"I get short of breath when I climb a lot of stairs": This symptom is more indicative of cardiovascular or respiratory issues, such as heart or lung disease, rather than intermittent claudication. It suggests that the client may experience exercise intolerance due to cardiopulmonary limitations.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
The best response by the nurse would be to explain that no food or drink is allowed for 4 hours before the stress test.
The reason for this restriction is that consuming food or drink can affect the accuracy of the cardiac stress test results. Eating or drinking can increase heart rate and blood pressure, potentially altering the test's interpretation. It is important for the client to have an empty stomach to ensure accurate test results.
Let's review the other options and explain why they are not the best responses:
Asking the client's visitor to bring some coffee from the cafeteria for the client: This option goes against the restriction of no food or drink before the stress test. It is important to adhere to the guidelines provided to ensure accurate test results.
Making up a small breakfast tray from what is available on the unit: Similarly, providing breakfast to the client goes against the restriction of no food before the stress test. The client should have an empty stomach for the test.
Offering hot tea or coffee only: While hot tea or coffee might be tempting for the client, it still violates the requirement of no food or drink before the stress test. The client should only be allowed to consume water during the fasting period.
Correct Answer is D
Explanation
Helping to position a client for a portable x-ray generally involves physically assisting the client in moving into the appropriate position or adjusting their body as needed. This task can be safely delegated to the UAP as long as they have received proper training on how to safely assist with positioning and have a clear understanding of the specific instructions provided by the radiology department.
Assisting the client to take the beta-blocker involves administering medication, which falls within the scope of nursing practice and requires the nurse's expertise in medication administration and monitoring the client's response.
Transporting the client to the intensive care unit via a stretcher involves moving the client to another unit and may require additional monitoring and coordination of care during the transfer. This task is best performed by the nurse, who can assess the client's stability, ensure appropriate documentation, and communicate effectively with the receiving unit.
Providing discharge-teaching instructions to the client going home requires the nurse to provide information about medications, wound care, follow-up appointments, and other important instructions. This task involves comprehensive education and assessment ofthe client's understanding, and is best performed by the nurse to ensure accurate and complete information is provided.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
