A nurse explains to new parents that their newborn has developed respiratory distress syndrome (RDS). Which of the following assessments that the nurse makes would support a diagnosis of RDS?
Select one:
Apical pulse of 148 beats per minute.
Respiratory rate of 40 during sleep.
Skin color jaundiced.
Chest retractions.
The Correct Answer is D
Choice A Reason: Apical pulse of 148 beats per minute. This is not a finding that would support a diagnosis of RDS, but rather a normal finding for a newborn. A normal apical pulse for a newborn ranges from 120 to 160 beats per minute. A high pulse rate may indicate fever, infection, anemia, or dehydration. A low pulse rate may indicate hypothermia, hypoxia, or heart block.
Choice B Reason: Respiratory rate of 40 during sleep. This is not a finding that would support a diagnosis of RDS, but rather a normal finding for a newborn. A normal respiratory rate for a newborn ranges from 40 to 60 breaths per minute. A high respiratory rate may indicate respiratory distress, infection, or metabolic acidosis. A low respiratory rate may indicate respiratory depression, hypothermia, or narcotic exposure.
Choice C Reason: Skin color jaundiced. This is not a finding that would support a diagnosis of RDS, but rather a different condition called jaundice. Jaundice is a yellowish discoloration of the skin and mucous membranes caused by elevated levels of bilirubin in the blood. Bilirubin is a breakdown product of hemoglobin that is normally excreted by the liver and kidneys. Jaundice can occur in newborns due to immature liver function, increased red blood cell breakdown, or blood group incompatibility. Jaundice does not affect lung function or oxygenation.
Choice D Reason: Chest retractions. This is because chest retractions are a sign of respiratory distress that indicate increased work of breathing and reduced lung compliance. Chest retractions occur when the chest wall sinks in between the ribs or below the sternum during inhalation, creating a negative pressure that helps draw air into the lungs. RDS is a serious condition where the newborn's lungs are immature and lack sufficient surfactant, which is a substance that reduces surface tension and prevents alveolar collapse. RDS can cause respiratory distress, hypoxia, acidosis, and organ failure. It is more common in preterm infants, especially those born before 37 weeks' gestation.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is D
Explanation
Choice A Reason: Applying Vaseline or lotion to newborn to maximize light absorption. This is an incorrect answer that indicates a contraindicated and harmful intervention that can interfere with phototherapy. Applying Vaseline or lotion to newborn can create a barrier or a reflective surface that can reduce the exposure and penetration of light to the skin, which can decrease the efficacy of phototherapy. Applying Vaseline or lotion to newborn can also cause skin irritation, infection, or burns, as it can trap heat and moisture under the light source.
Choice B Reason: Reducing the amount of fluid intake to 8 ounces daily. This is an incorrect answer that suggests a detrimental and dangerous intervention that can impair phototherapy. Reducing the amount of fluid intake to 8 ounces daily can cause dehydration, hypoglycemia, or electrolyte imbalance in newborns, which can worsen jaundice and increase the risk of complications such as kernicterus (brain damage due to high bilirubin levels). Reducing the amount of fluid intake to 8 ounces daily can also decrease the excretion of bilirubin through urine or stool, which can counteract the effect of phototherapy.
Choice C Reason: Keeping the newborn in the supine position. This is an incorrect answer that implies an incomplete and inadequate intervention that can limit phototherapy. Keeping the newborn in the supine position is a nursing action that involves placing the newborn on their back, which can expose their anterior body surface to light.
However, keeping the newborn in the supine position alone is not sufficient for phototherapy, as it does not expose their posterior body surface to light. The nurse should also reposition the newborn frequently to expose different body parts to light, such as their sides or abdomen.
Choice D Reason: Feeding every 3 hours to maximize intake of fluids and output. This is because feeding every 3 hours is a nursing intervention that can enhance the effectiveness and safety of phototherapy, which is a treatment that uses blue or white light to reduce the level of bilirubin in the blood. Bilirubin is a yellow pigment that is produced when red blood cells are broken down, which can cause jaundice (yellowish discoloration of the skin and mucous membranes) if it accumulates in excess. Phototherapy works by converting bilirubin into a water-soluble form that can be excreted through urine or stool. Feeding every 3 hours can increase the intake of fluids and calories, which can promote hydration, nutrition, and elimination of bilirubin.
Correct Answer is C
Explanation
Choice A Reason: Late decelerations. This is an incorrect answer that refers to a different type of fetal heart rate patern that indicates uteroplacental insufficiency, which can reduce blood flow and oxygen delivery to the fetus. Late decelerations are characterized by gradual decreases in fetal heart rate that begin after the peak of uterine contractions and return to baseline after the end of contractions. Amnioinfusion is not effective for late decelerations, as it does not address the underlying cause of uteroplacental insufficiency, which may be due to maternal hypertension, diabetes, preeclampsia, or placental abruption.
Choice B Reason: Moderate decelerations. This is an incorrect answer that refers to a non-existent type of fetal heart rate patern, as there is no such term as moderate decelerations. The term moderate refers to the category of fetal heart rate variability, which is a measure of the fluctuations in fetal heart rate around the baseline. Moderate variability indicates normal fetal oxygenation and well-being, while absent or minimal variability indicates fetal hypoxia or distress.
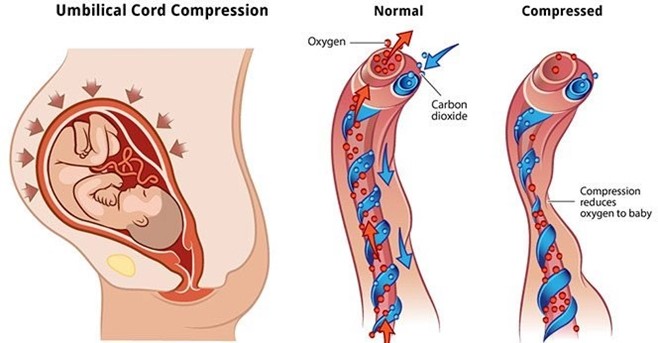
Choice C Reason: Variable decelerations. This is because variable decelerations are a type of fetal heart rate patern that indicates cord compression, which can reduce blood flow and oxygen delivery to the fetus. Variable decelerations are characterized by abrupt decreases in fetal heart rate that vary in onset, depth, and duration, and do not have a consistent relationship with uterine contractions. Amnioinfusion is a procedure that involves infusing saline or lactated Ringer's solution into the amniotic cavity through a transcervical catheter, which can relieve cord compression by increasing the volume of amniotic fluid and cushioning the cord. Amnioinfusion can improve fetal oxygenation and reduce variable decelerations.
Choice D Reason: Early decelerations. This is an incorrect answer that refers to a different type of fetal heart rate patern that indicates head compression, which can stimulate the vagus nerve and slow down the fetal heart rate. Early decelerations are characterized by gradual decreases in fetal heart rate that begin with the onset of uterine contractions and return to baseline with the end of contractions. Early decelerations are benign and do not require intervention, as they reflect normal fetal head descent and progress of labor. Amnioinfusion is not indicated for early decelerations, as it does not affect head compression or vagal stimulation.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
