In a client's seventh month of pregnancy, she reports feeling "dizzy, like I'm going to pass out, when I lie down flat on my back". The nurse explains that this is due to:
Select one:
Physiologic anemia due to maternal increased plasma volume.
Pressure of the gravid uterus on the maternal inferior vena cava and aorta.
Pressure of the presenting fetal part on the maternal diaphragm.
A 50% increase in maternal blood volume during pregnancy.
The Correct Answer is B
Choice A Reason: Physiologic anemia due to maternal increased plasma volume. This is an incorrect answer that refers to a different condition that affects hemoglobin levels, not blood pressure. Physiologic anemia is a condition where the maternal plasma volume increases more than the red blood cell mass during pregnancy, which dilutes the hemoglobin concentration and lowers the hematocrit value. Physiologic anemia does not cause significant symptoms or complications in pregnant women, as it is an adaptive mechanism that enhances oxygen delivery and prevents fluid overload.
Choice B Reason: Pressure of the gravid uterus on the maternal inferior vena cava and aorta. This is because this statement explains the cause of supine hypotensive syndrome, which is a condition where lying flat on the back causes compression of the major blood vessels by the gravid uterus, which reduces venous return and cardiac output, which lowers blood pressure and perfusion to vital organs. Supine hypotensive syndrome can cause symptoms such as dizziness, lightheadedness, nausea, pallor, or syncope in pregnant women, especially in the third trimester.
Choice C Reason: Pressure of the presenting fetal part on the maternal diaphragm. This is an incorrect answer that indicates a different condition that affects respiratory function, not blood pressure. Pressure of the presenting fetal part on the maternal diaphragm is a result of cephalic engagement or lightening, which occurs when the fetal head descends into the pelvis and occupies more space in the abdominal cavity. Pressure of the presenting fetal part on the maternal diaphragm can cause symptoms such as dyspnea, heartburn, or rib pain in pregnant women.
Choice D Reason: A 50% increase in maternal blood volume during pregnancy. This is an incorrect answer that describes a normal physiological change that occurs during pregnancy, not a cause of supine hypotensive syndrome. A 50% increase in maternal blood volume during pregnancy is due to increased production of plasma and red blood cells, which helps meet the increased oxygen and nutrient demands of the fetus and placenta, and prepares the mother for blood loss during delivery. A 50% increase in maternal blood volume during pregnancy does not cause hypotension or dizziness in pregnant women.

Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
Choice A Reason: The cheek of the newborn is touched, and the newborn turns toward the side that was touched. This is an incorrect answer that describes a different reflex called the rooting reflex. The rooting reflex is a feeding reflex that helps the newborn locate the nipple and initiate sucking. The rooting reflex is elicited by stroking the cheek or corner of the mouth of the newborn, which causes them to turn their head and open their mouth toward the stimulus.
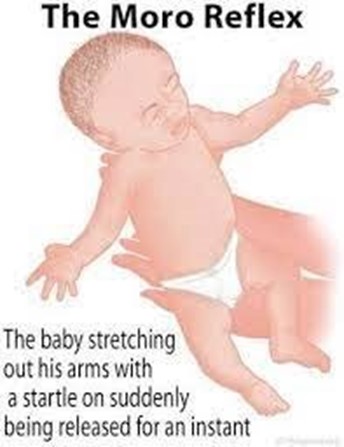
Choice B Reason: The newborn is suddenly lowered or startled, and they extend their arms, legs and neck, then rapidly bring their arms together. This is because this response describes the Moro reflex, which is a primitive reflex that is present at birth and disappears by 3 to 6 months of age. The Moro reflex is elicited by simulating a falling sensation or a loud noise, which triggers a fear response in the newborn. The Moro reflex consists of four phases: extension, abduction, adduction, and crying.
Choice C Reason: The newborn is supine and their head is turned to one side, then the arm on that same side extends. This is an incorrect answer that refers to another reflex called the tonic neck reflex. The tonic neck reflex is a postural reflex that helps prepare the newborn for voluntary reaching. The tonic neck reflex is elicited by placing the newborn in a supine position and turning their head to one side, which causes them to assume a "fencing" posture with one arm extended and one arm flexed.
Choice D Reason: The lateral aspect of the sole of the newborn's foot is stroked, and the toes extend and fan outward. This is an incorrect answer that indicates a different reflex called the Babinski reflex. The Babinski reflex is a neurological reflex that tests for spinal cord integrity. The Babinski reflex is elicited by stroking the lateral aspect of the sole of the foot from heel to toe, which causes the big toe to dorsiflex and the other toes to fan out.
Correct Answer is D
Explanation
Choice A Reason: Vitamin K will increase erythropoiesis. This is an incorrect statement that confuses vitamin K with erythropoietin. Erythropoietin is a hormone that stimulates red blood cell production in the bone marrow. Vitamin K does not affect erythropoiesis.
Choice B Reason: Vitamin K will enhance bilirubin breakdown. This is an incorrect statement that confuses vitamin K with phototherapy. Phototherapy is a treatment that exposes the newborn's skin to light, which converts bilirubin into water-soluble forms that can be excreted by the liver and kidneys. Bilirubin is a yellow pigment that results from the breakdown of red blood cells. High levels of bilirubin can cause jaundice and brain damage in newborns. Vitamin K does not affect bilirubin metabolism.
Choice C Reason: Vitamin K will stop Rh sensitization. This is an incorrect statement that confuses vitamin K with Rh immune globulin. Rh immune globulin is an injection given to Rh-negative mothers who deliver Rh-positive babies, to prevent them from developing antibodies against Rh-positive blood cells in future pregnancies. Rh sensitization is a condition where the mother's immune system atacks the baby's blood cells, causing hemolytic disease of the newborn. Vitamin K does not affect Rh sensitization.
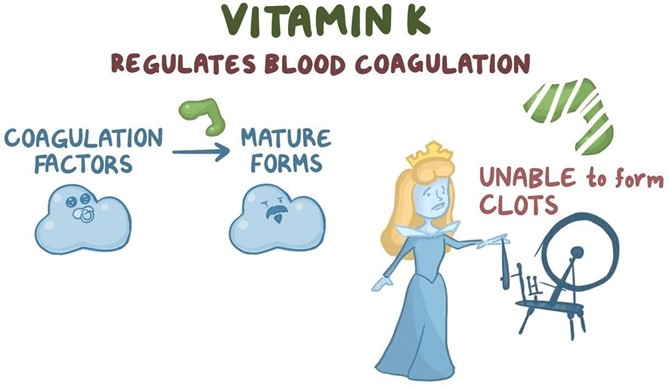
Choice D Reason: Vitamin K will promote blood clotting ability. This is a correct statement that explains the rationale for administering vitamin K as prophylaxis to newborns. Vitamin K is essential for the synthesis of clotting factors in the liver. Newborns have low levels of vitamin K at birth due to poor placental transfer and lack of intestinal bacteria that produce vitamin K. Therefore, they are at risk of bleeding disorders such as hemorrhagic disease of the newborn.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
