The nurse is reviewing the medical records of a client with atrial fibrillation. Which prescription should the nurse question?
Obtain consent for transesophageal echocardiogram (TEE)
Obtain consent for a STAT defibrillation
Obtain consent for cardioversion.
Hold digoxin 48 hours prior to cardioversion.
The Correct Answer is B
Defibrillation is not the first-line treatment for atrial fibrillation. It is used to treat life-threatening cardiac arrhythmias such as ventricular fibrillation or pulseless ventricular tachycardia. Atrial fibrillation, on the other hand, is a rapid and irregular atrial rhythm, and defibrillation is not indicated for its treatment.
Obtain consent for transesophageal echocardiogram (TEE): This is an appropriate action for a client with atrial fibrillation. A TEE is often performed to assess the structure and function of the heart in cases of atrial fibrillation, especially when considering cardioversion or other interventions.
Obtain consent for cardioversion: Cardioversion is a common treatment option for atrial fibrillation, especially when the client is unstable or experiencing symptoms. It involves restoring a normal heart rhythm through the use of electrical shocks or medications. It is important to obtain informed consent before performing cardioversion, but this does not necessarily require questioning.
Hold digoxin 48 hours prior to cardioversion: Digoxin is commonly held before cardioversion because it can increase the risk of certain arrhythmias during the procedure. This is a standard precaution to minimize potential adverse effects. Therefore, the nurse does not need to question this action, as it aligns with established guidelines.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
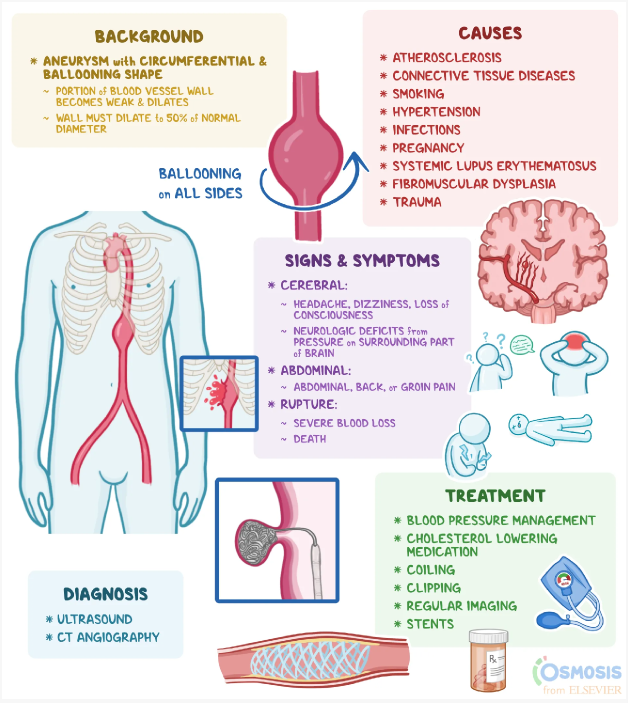
Abdominal aortic aneurysms (AAA) often do not present with specific symptoms in the early stages. It is not uncommon for individuals with AAA to be asymptomatic or have vague symptoms. Therefore, the absence of abdominal pain or any problems related to the abdomen is a common finding during the assessment of a client with an abdominal aortic aneurysm.
Let's briefly review the other statements:
"I have stomach pain every time I eat a big, heavy meal": This statement is more suggestive of gastrointestinal issues such as indigestion or acid reflux rather than specifically related to an abdominal aortic aneurysm.
"I have periodic episodes of constipation and then diarrhea": This statement may indicate gastrointestinal issues, but it is not a typical symptom associated with an abdominal aortic aneurysm. AAA is primarily related to the aorta, the main blood vessel in the abdomen, and its symptoms are not directly linked to bowel function.
"I belch a lot, especially when I lay down after eating": This statement suggests gastrointestinal symptoms such as acid reflux or gastroesophageal reflux disease (GERD). While these symptoms may be unrelated to the abdominal aortic aneurysm itself, they can coexist with other conditions.
Correct Answer is A
Explanation
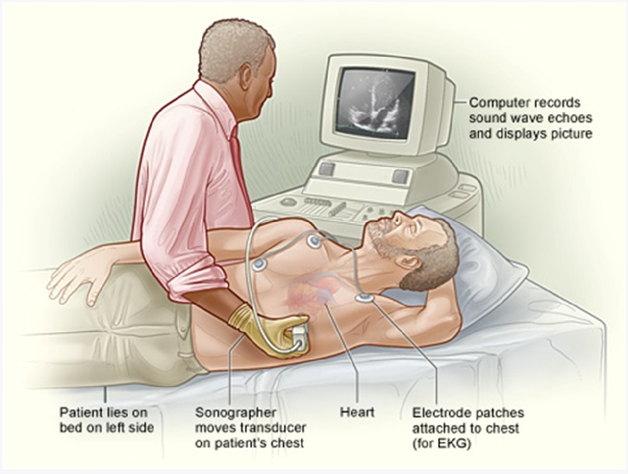
The nurse should teach the client that the transthoracic echocardiography is a noninvasive test and that nothing will be inserted into the client's body.
Transthoracic echocardiography is a diagnostic procedure that uses ultrasound to create images of the heart's structures and assess its function. It is a noninvasive test, meaning that it does not involve any insertion of instruments or devices into the body. Instead, a transducer is placed on the chest to obtain images of the heart.
The statement about managing pain aggressively during the procedure is not applicable to transthoracic echocardiography. It is generally a painless procedure that does not cause discomfort.
Transthoracic echocardiography primarily provides detailed images of the heart's structures and function, such as the chambers, valves, and pumping action. It does not specifically profile the heart's electrical activity, which is usually assessed using an electrocardiogram (ECG) or other specialized tests.
Regarding bed rest after the test, there is typically no need for bed rest following transthoracic echocardiography. The client can usually resume normal activities immediately after the procedure. However, the nurse should provide specific instructions based on the client's condition and any additional tests or interventions planned.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
