A nurse accompanies a client to an exercise stress test. The client can achieve the target heart rate, but the electrocardiogram indicates ST-segment elevation. Which procedure will the nurse prepare the patient for?
cardiac catheterization
transesophageal echocardiogram
telemetry monitoring
pharmacologic stress test
The Correct Answer is A
ST-segment elevation during exercise stress testing is a concerning finding that may indicate reduced blood flow to the heart muscle. It can be a sign of myocardial ischemia or coronary artery disease. Cardiac catheterization is a diagnostic procedure that allows direct visualization of the coronary arteries and helps identify any blockages or narrowing that may be causing the ST-segment elevation.
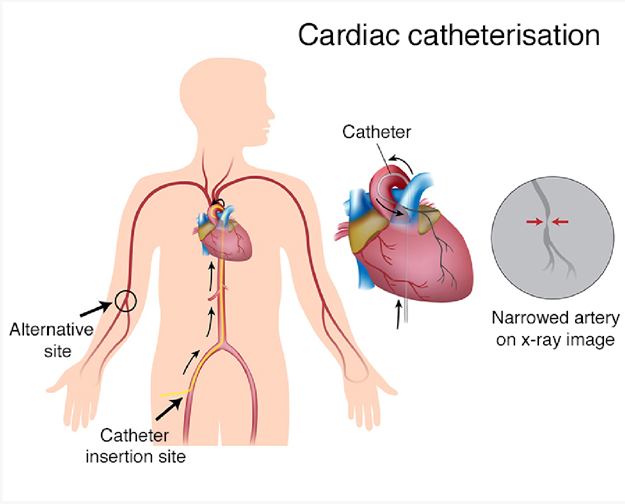
Here's an explanation of why the other options are not the most appropriate procedures:
Transesophageal echocardiogram: Transesophageal echocardiogram (TEE) is a diagnostic test that involves inserting a probe into the esophagus to obtain detailed images of the heart. It is not typically used to evaluate ST-segment elevation, which primarily indicates coronary artery issues rather than structural abnormalities.
Telemetry monitoring: Telemetry monitoring involves continuous monitoring of a patient's heart rhythm and can be used for various cardiac conditions. While telemetry monitoring may be necessary for ongoing cardiac assessment, it is not a specific procedure to address the ST-segment elevation found during the exercise stress test.
Pharmacologic stress test: A pharmacologic stress test is an alternative to an exercise stress test for patients who cannot exercise. It involves administering medications that stimulate the heart to mimic the effects of exercise. While a pharmacologic stress test can also reveal ST-segment changes, the presence of ST-segment elevation usually requires further evaluation with a more invasive procedure like cardiac catheterization.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is ["D","E"]
Explanation
The traces that should require immediate follow-up by the nurse are:
● Pacer spikes occur directly before the T waves.
Pacer spikes occurring on the T waves indicate an issue with the pacemaker's timing or sensing. This could lead to inappropriate pacing or pacing during the refractory period, which can be detrimental to the client's heart function.
● The heart rate is outside of programmed parameters.
If the heart rate is outside of the programmed parameters set for the client's pacemaker, it may indicate a malfunction or failure of the device or a change in the client's cardiac status. It is important for the nurse to assess the client's condition and notify the healthcare provider for further evaluation and intervention.
Let's review the other options and explain why they do not require immediate follow-up:
Pacer spikes are adequate in number: This indicates that the pacemaker is delivering the appropriate number of electrical impulses as programmed. As long as the other parameters are normal, this finding does not require immediate follow-up.
Pacer spikes occur directly before the P waves: This is the desired and expected pattern for a pacemaker in normal sinus rhythm. It indicates proper timing and coordination between the pacemaker and the client's intrinsic electrical activity.
Pacer spikes occur directly before the QRS waves: This is also the desired and expected pattern for a pacemaker in clients with ventricular pacing. It indicates proper timing and coordination between the pacemaker and the client's intrinsic electrical activity.
The heart rate is within programmed parameters: If the heart rate falls within the programmed parameters set for the client's pacemaker, it indicates that the device is functioning appropriately in maintaining the desired heart rate.
Correct Answer is A
Explanation
Elevated levels of LDL (low-density lipoprotein) cholesterol are associated with an increased risk of coronary artery disease (CAD). LDL cholesterol is often referred to as "bad" cholesterol because it can contribute to the formation of plaque in the arteries, leading to narrowing and blockage of the arteries supplying the heart. This increases the risk of developing CAD and related complications such as heart attack and stroke.
On the other hand, HDL (high-density lipoprotein) cholesterol is often referred to as "good" cholesterol. HDL cholesterol helps remove excess cholesterol from the bloodstream and transport it back to the liver for processing and excretion. Higher levels of HDL cholesterol are associated with a decreased risk of CAD because it helps to prevent the accumulation of cholesterol on artery walls.
Therefore, understanding that increased LDL and decreased HDL levels increase the risk of coronary artery disease demonstrates a good understanding of the significance of cholesterol levels and their impact on cardiovascular health.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
