The nurse is caring for a client with hypertension who is on alpha blockers. The nurse is concerned about postural hypotension. Which information should the nurse include in the teaching plan?
Change positions slowly
Check blood pressure every day for signs of rebound hypertension
Do not become dependent on canes, walkers, or handrails.
Eat plenty of salty food to prevent hypotension
The Correct Answer is A
The information that the nurse should include in the teaching plan for a client with hypertension who is on alpha blockers and at risk for postural hypotension is: Change positions slowly.
Alpha blockers are a class of medications commonly prescribed for hypertension. One potential side effect of alpha blockers is postural hypotension, which is a sudden drop in blood pressure when changing positions, such as from sitting to standing. To minimize the risk of postural hypotension, it is important for the client to change positions slowly. The nurse should advise the client to take their time when transitioning from lying down, sitting, or standing, allowing their body to adjust and stabilize their blood pressure.
The other options are not appropriate or helpful in managing postural hypotension:
Check blood pressure every day for signs of rebound hypertension: Rebound hypertension refers to a sudden increase in blood pressure that can occur when discontinuing certain antihypertensive medications. It is not directly related to postural hypotension. Regular blood pressure monitoring is important for managing hypertension, but it is not specifically related to postural hypotension or alpha blockers.
Do not become dependent on canes, walkers, or handrails: Assistive devices like canes, walkers, or handrails can provide support and stability for individuals who experience balance issues or are at risk of falls. It is not necessary to discourage their use unless there are specific contraindications or safety concerns.
Eat plenty of salty food to prevent hypotension: Increasing salt intake is generally not recommended for individuals with hypertension or those at risk of postural hypotension. A high-sodium diet can contribute to elevated blood pressure and is generally discouraged. The nurse should instead encourage a balanced diet that includes appropriate sodium intake based on the client's healthcare provider's recommendations.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is C
Explanation
Enalapril (Vasotec) is an angiotensin-converting enzyme (ACE) inhibitor medication commonly used to treat hypertension. One of the potential side effects of ACE inhibitors is hyperkalemia, which is an elevated level of potassium in the blood. Therefore, it is generally recommended for patients taking ACE inhibitors to avoid excessive intake of high-potassium foods.
The charge nurse should intervene because advising the client to increase their dietary intake of high-potassium foods contradicts the precautions associated with taking enalapril. Consuming high-potassium foods while taking this medication can potentially lead to an increased risk of hyperkalemia, which can have serious health consequences.
Let's review the other statements made by the nurse:
"Make an appointment with the dietitian for teaching": This is an appropriate statement as it encourages the client to seek professional guidance on dietary management of hypertension. A dietitian can provide valuable information on healthy eating habits and strategies to reduce blood pressure.
"Check your blood pressure at home at least once a day": This is also an appropriate statement as it promotes self-monitoring of blood pressure, which is important for clients with hypertension. Regular monitoring helps the client track their progress and detect any changes that may require medical attention.
"Move slowly when moving from lying to sitting to standing": This is a correct statement as it advises the client to practice orthostatic precautions. ACE inhibitors, including enalapril, can cause orthostatic hypotension, a drop in blood pressure upon standing. Moving slowly can help prevent dizziness and falls.
Correct Answer is C
Explanation
"I will use a heating pad on my feet at night to increase the circulation.": Using a heating pad on the feet at night is not recommended for clients with peripheral artery disease. The application of heat, such as from a heating pad, can dilate blood vessels and potentially worsen the symptoms of peripheral artery disease. This can lead to reduced blood flow to the affected limbs and increase the risk of complications.
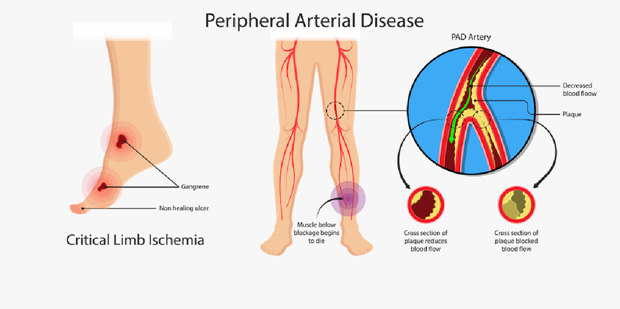
The other client statements demonstrate an understanding of peripheral artery disease management:
"I will avoid long periods of sitting down with my legs crossed over." This statement shows awareness of the importance of maintaining good blood flow and avoiding positions that can restrict circulation.
"I will walk to the point of pain, rest, and walk again for at least 30 minutes." This statement indicates an understanding of the concept of intermittent claudication, a common symptom of peripheral artery disease. Walking until pain occurs, resting, and then resuming walking helps improve circulation and increases walking distance over time.
"I will buy some loose clothes that do not bind across my legs or waist." This statement reflects an awareness of the need to wear loose-fitting clothes that do not constrict blood flow to the legs or waist area.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
