The nurse is doing a neurologic assessment on a 2-month-old infant after a car accident. Moro, tonic neck, and withdrawal reflexes are present. The nurse should recognize that these reflexes are:
Symptomatic of decorticate posturing
Symptomatic of decerebrate posturing
Indicators of severe brain damage
Normal Findings
The Correct Answer is D
Reflexes play a crucial role in evaluating the neurological status of infants.
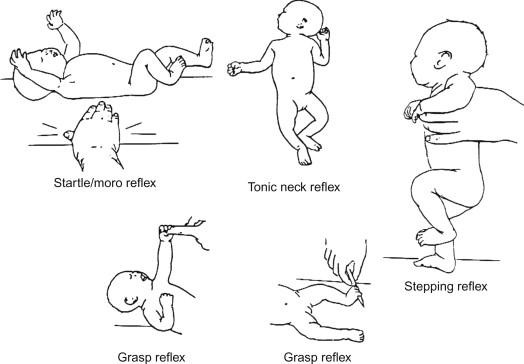
Moro reflex: Also known as the startle reflex, the Moro reflex is a normal response in infants. It occurs when an infant is startled by a sudden noise or movement. The baby responds by extending their arms and legs, followed by a quick contraction. This reflex usually disappears around 4-6 months of age.
Tonic neck reflex (fencer's reflex): This reflex involves turning an infant's head to one side, causing the arm on that side to extend and the opposite arm to flex. It's a normal reflex that typically disappears around 4-6 months of age.
Withdrawal reflex: The withdrawal reflex is a normal response to a stimulus, such as touching a baby's foot with a cold object. The baby will pull their leg away in response to the stimulus.
Symptomatic of decorticate or decerebrate posturing (options A and B):
Decorticate and decerebrate posturing are abnormal postures seen in individuals with severe brain damage or injury. Decorticate posturing involves the arms being flexed and held close to the body, while decerebrate posturing involves the arms being extended and the wrists being pronated. These reflexes are typically indicative of significant neurological dysfunction and are not expected in a 2-month-old infant after a car accident.
Indicators of severe brain damage (option C):
The reflexes described (Moro, tonic neck, and withdrawal reflexes) are not indicative of severe brain damage in a 2-month-old infant. These reflexes are normal for an infant of this age and are part of their typical neurological development.
Normal findings (option D):
The reflexes described are normal findings in a 2-month-old infant and are expected as part of their developmental milestones.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
A. Dizziness is always a sign of a concussion.
This statement is incorrect. While dizziness can be a symptom of a concussion, it is not always indicative of a concussion. There can be various causes of dizziness, and it is essential to consider other symptoms as well when assessing for a concussion.
B. Bike Helmet Safety
Explanation:
The correct answer to include as part of concussion/head injury prevention teaching to children and parents is "Bike helmet safety." This is because wearing a helmet while riding a bike or participating in other activities that involve head injury risks is crucial to prevent head injuries and concussions. Helmets provide protection to the head by absorbing impact energy and reducing the risk of skull fractures or traumatic brain injuries.
C. Normal fluid intake.
While staying hydrated is important for overall health, it is not directly related to concussion or head injury prevention teaching. This choice is unrelated to the topic.
D. Signs of autism.
Signs of autism are unrelated to concussion or head injury prevention teaching. This choice is not relevant to the topic at hand.
Correct Answer is {"dropdown-group-1":"D"}
Explanation
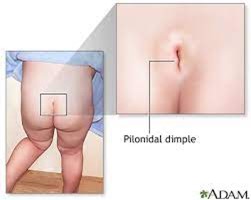
Pilonidal dimpling with the presence of an abnormal tuft of hair in or near the dimple
Explanation:
Spina bifida is a congenital condition where there is incomplete closing of the backbone and membranes around the spinal cord during early development in the womb. Pilonidal dimpling with the presence of an abnormal tuft of hair in or near the dimple is a specific sign of spina bifida. This condition is called "sacral dimple," and it can indicate an underlying issue with the spinal cord and nerves. An abnormal tuft of hair in or near the dimple suggests a neural tube defect, which is characteristic of spina bifida.
Why the other choices are incorrect:
A. complete paralysis:
Complete paralysis is a severe neurological symptom but it is not specific to spina bifida. It can occur due to various other conditions as well, such as spinal cord injuries, infections, and neurological disorders. It's not a characteristic sign of spina bifida.
B. Petechiae:
Petechiae are small, red or purple spots on the skin that are caused by bleeding under the skin. They are usually associated with bleeding disorders, infections, or other medical conditions. Petechiae are not a characteristic sign of spina bifida.
C. Abnormal Vital Signs:
While spina bifida can potentially lead to neurological complications that might influence vital signs, the presence of abnormal vital signs is a non-specific symptom. Abnormal vital signs could be caused by a wide range of medical conditions, and they are not directly indicative of spina bifida.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
