Mrs. Kalen is a 70-year-old female who has arrived at the ER due to persistent vomiting for two days now. She appears to be lethargic and weak and has myalgia. She is noted to have dry mucus membranes and her capillary refill takes >4 seconds. She is diagnosed as having gastroenteritis and dehydration. Measurement of arterial blood gas shows pH 7.5, PaO2 85 mm Hg, PaCO2 40 mm Hg, and HCO3 34 mmol/L. Based on the acid-base interruption from Mrs. Kalen, what can the nurse anticipate the treatment will be for correcting this imbalance?
administration of antiemetics
administration of diuretics
Possible Electrolyte replacement if warranted
Administration of IV 0.9 Saline Solution infusion
Have the patient go home and rest. It will resolve itself shortly.
The Correct Answer is D
Mrs. Kalen is diagnosed with gastroenteritis and dehydration, and the arterial blood gas results indicate metabolic alkalosis (elevated pH and HCO3-). This suggests that there is an excessive loss of gastric acid and chloride ions from vomiting, leading to an imbalance of electrolytes and an increase in bicarbonate levels.
To correct the imbalance and treat dehydration, the primary intervention is fluid replacement. Administration of IV 0.9 Saline Solution, also known as normal saline, is commonly used for fluid resuscitation and rehydration. This isotonic solution helps restore fluid balance and electrolyte levels in the body.
Administration of antiemetics may help control vomiting, but the primary treatment focus in this case is fluid and electrolyte replacement to correct dehydration and the associated metabolic alkalosis.
Administration of diuretics, which increase urine output, would not be appropriate in this case as the patient is already experiencing dehydration.
Electrolyte replacement may be necessary if there are specific electrolyte imbalances identified, but the primary treatment is fluid replacement with IV saline solution.
Having the patient go home and rest without addressing the underlying dehydration and metabolic alkalosis would not be appropriate as it can lead to further complications.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
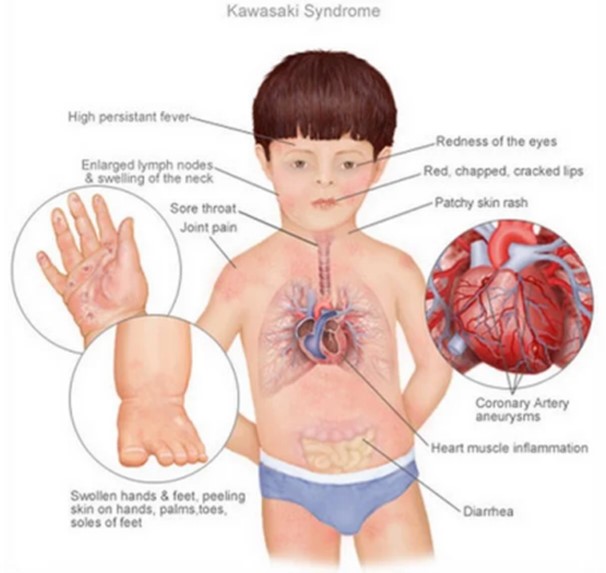
Correct Answer is A
Explanation
Correct Answer is D
Explanation
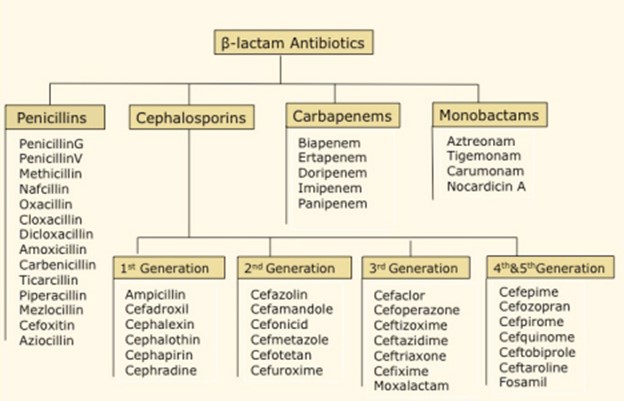
Cephalosporins are similar to another group of beta-lactam antibiotics called the Penicillins. Both cephalosporins and penicillins belong to the beta-lactam class of antibiotics, which share a similar structure and mechanism of action. They inhibit bacterial cell wall synthesis by binding to specific proteins called penicillin-binding proteins (PBPs), leading to bacterial cell death. This shared mechanism of action makes cephalosporins and penicillins similar in their antibacterial effects.
On the other hand, macrolides, fluoroquinolones, and aminoglycosides are different classes of antibiotics with distinct structures and mechanisms of action. They work through different mechanisms to inhibit bacterial growth and have different spectrums of activity compared to beta-lactam antibiotics like cephalosporins and penicillins.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
