An older adult client with a long history of chronic obstructive pulmonary disease (COPD) is admitted with progressive shortness of breath and a persistent cough. The client is anxious and is complaining of a dry mouth. Which intervention should the nurse implement?
Administer a prescribed sedative
Assist client to an upright position.
Encourage client to drink water
Apply a high-flow venturi mask.
The Correct Answer is B
A. Administer a prescribed sedative:
Sedatives may depress the respiratory drive, which can be detrimental in a client with respiratory distress. It is not the appropriate intervention in this case.
B. Assist the client to an upright position.
Positioning the client upright helps improve respiratory mechanics by reducing the pressure on the diaphragm and allowing better lung expansion. This position can enhance the efficiency of breathing and alleviate symptoms of breathlessness.
C. Encourage the client to drink water:
While maintaining hydration is important, it may not directly address the immediate respiratory distress. Addressing the respiratory symptoms with an upright position is more crucial at this moment.
D. Apply a high-flow venturi mask:
While oxygen therapy may be necessary for a client with COPD experiencing respiratory distress, the first step is to assist the client to an upright position to improve respiratory mechanics. Applying a high-flow venturi mask may be a subsequent intervention based on the overall assessment, but positioning is the initial priority.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
A. Activity level of bowel sounds:
Bowel sounds are important to assess, but they may not directly influence or be influenced by the abdominal pain associated with chronic pancreatitis.
B. Eating patterns and dietary intake.
Clients with chronic pancreatitis often experience abdominal pain exacerbated by the intake of food, especially fatty meals. Monitoring the client's eating patterns and dietary intake is crucial for identifying triggers that may worsen the abdominal pain. By understanding the relationship between food intake and pain, the nurse can provide guidance on dietary modifications to help manage the symptoms.
C. Level and amount of physical activity:
While physical activity is important for overall health, it may not be the primary factor contributing to or alleviating the abdominal pain in a client with chronic pancreatitis.
D. Color and consistency of feces:
Monitoring the color and consistency of feces is important for assessing pancreatic function, but it may not be the most immediate factor to address in the context of managing abdominal pain. Dietary patterns are more directly related to pain management in this case.
Correct Answer is D
Explanation
A. Hyperaldosteronism causing an increased sodium reabsorption in renal tubules.
Hyperaldosteronism is characterized by an excess of aldosterone, a hormone that regulates sodium and water balance. In cirrhosis, however, sodium retention is often related to other mechanisms such as portal hypertension and hypoalbuminemia, rather than hyperaldosteronism.
B. Decreased renin-angiotensin response related to an increase in renal blood flow.
Cirrhosis is more commonly associated with an activated renin-angiotensin-aldosterone system, leading to increased sodium and water retention. The increased renin-angiotensin response is a compensatory mechanism to maintain perfusion in the setting of cirrhosis and does not contribute to decreased renal blood flow.
C. Decreased portacaval pressure with greater collateral circulation.
This statement is not accurate. In cirrhosis, there is typically increased portacaval pressure due to portal hypertension, which can lead to the development of collateral circulation. However, this does not explain the edema and ascites seen in cirrhosis.
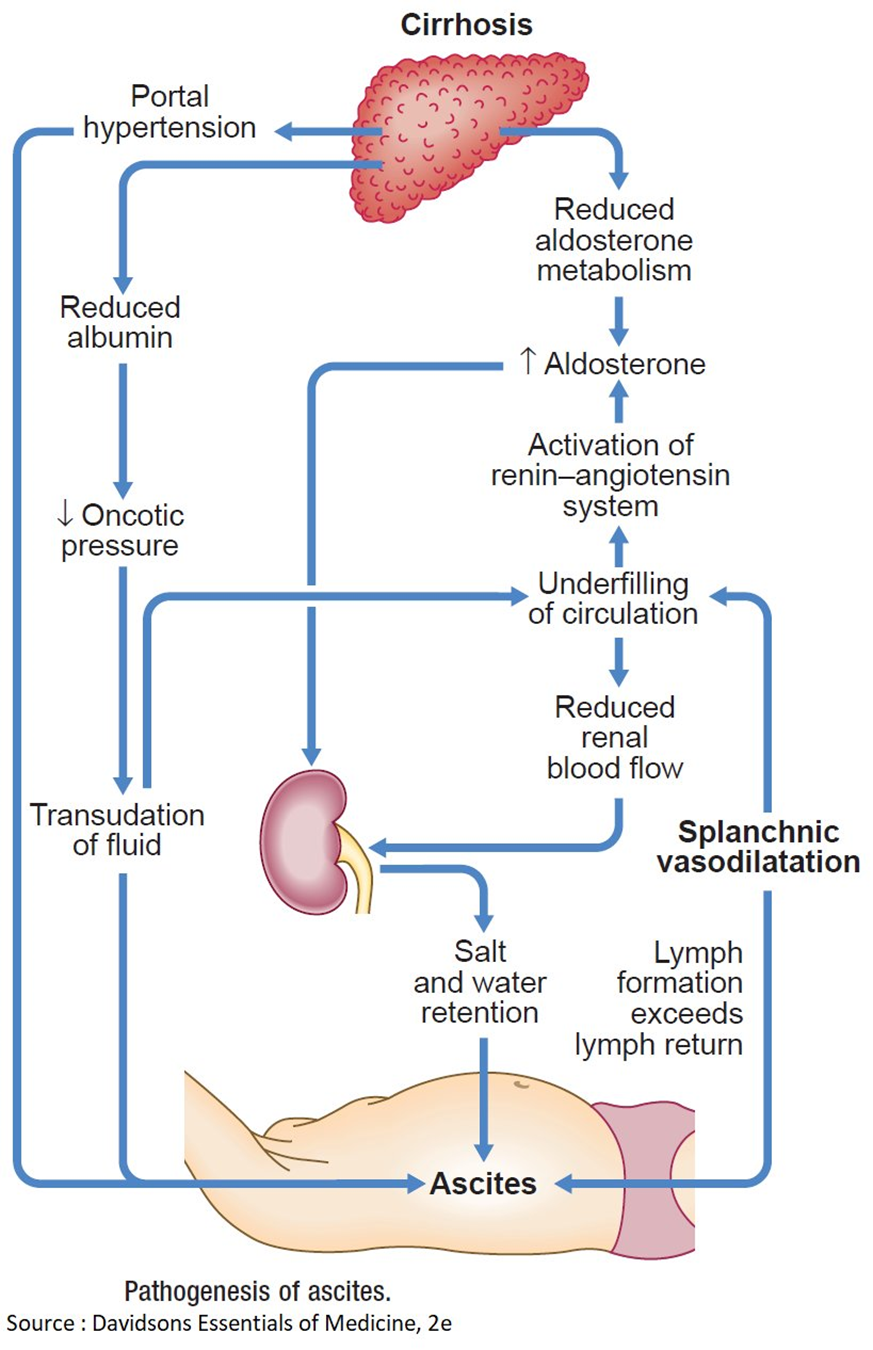
D. Hypoalbuminemia that results in a decreased colloidal oncotic pressure.
This is the correct choice. In cirrhosis, liver damage leads to decreased synthesis of albumin. Albumin plays a crucial role in maintaining colloidal oncotic pressure, and when it is decreased (hypoalbuminemia), fluid is more likely to leak out of blood vessels, resulting in edema. The same mechanism contributes to the development of ascites in the abdominal cavity.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
