The healthcare provider prescribes penicillin 200, 000 units intramuscularly for a client with pneumonia. The available vial is labeled, "Penicillin 500,000 units/mL". How many mL should the nurse administer to this client?
(Enter numerical value only. If rounding is required, round to the nearest tenth.)
The Correct Answer is ["0.4"]
Step 1: Use the Formula
mL = units prescribed ÷ units per mL
Step 2: Plug in the Given Values
mL = 200,000 ÷ 500,000
Step 3: Simplify the Fraction
mL = 2 ÷ 5
Step 4: Convert the Fraction to a Decimal
mL = 0.4 mL
The nurse should administer 0.4 mL of penicillin to this client.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is D
Explanation
A. Eat a diet high in carotene:
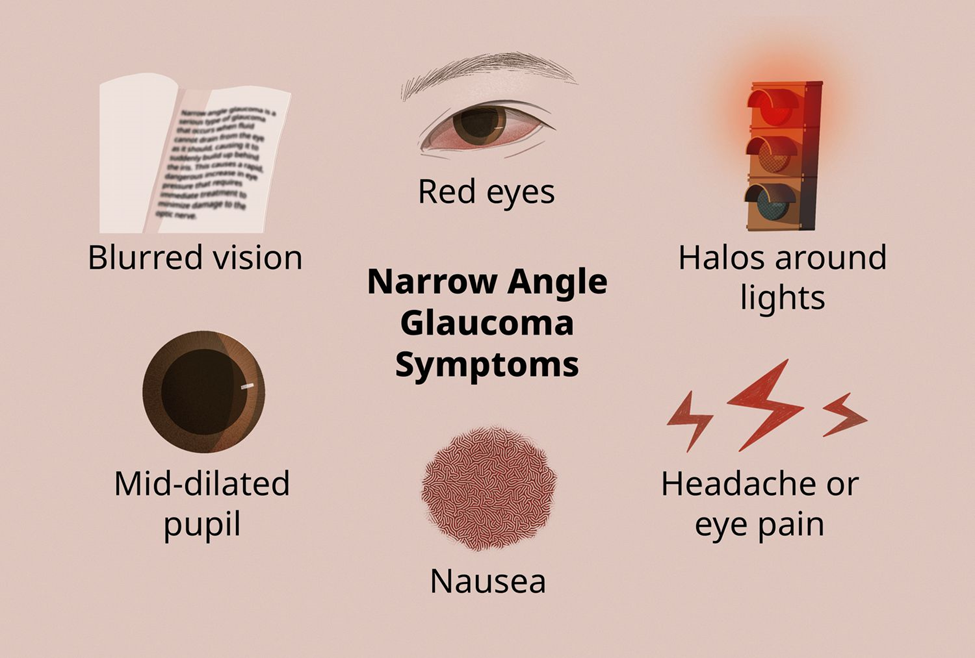
While a healthy diet is important for overall well-being, there is no evidence to suggest that a diet high in carotene specifically prevents or treats glaucoma. The focus in glaucoma management is on intraocular pressure control.
B. Wear prescription glasses:
Prescription glasses may be beneficial for addressing refractive errors, but they do not specifically address the management of glaucoma. The client's concern about driving through a tunnel is more likely related to changes in peripheral vision associated with glaucoma.
C. Avoid frequent eye pressure measurements:
This is not the most important instruction. Monitoring intraocular pressure is a crucial aspect of glaucoma management, and the frequency of measurements is determined by the healthcare provider. Regular monitoring helps assess the effectiveness of treatment and disease progression.
D. Maintain the prescribed eye drop regimen:
This is the correct answer. The most important instruction for the client is to adhere to the prescribed eye drop regimen. Medications, often in the form of eye drops, are commonly used to lower intraocular pressure and manage glaucoma. Consistent use of prescribed medications is critical for controlling the condition and preventing further vision loss.
Correct Answer is D
Explanation
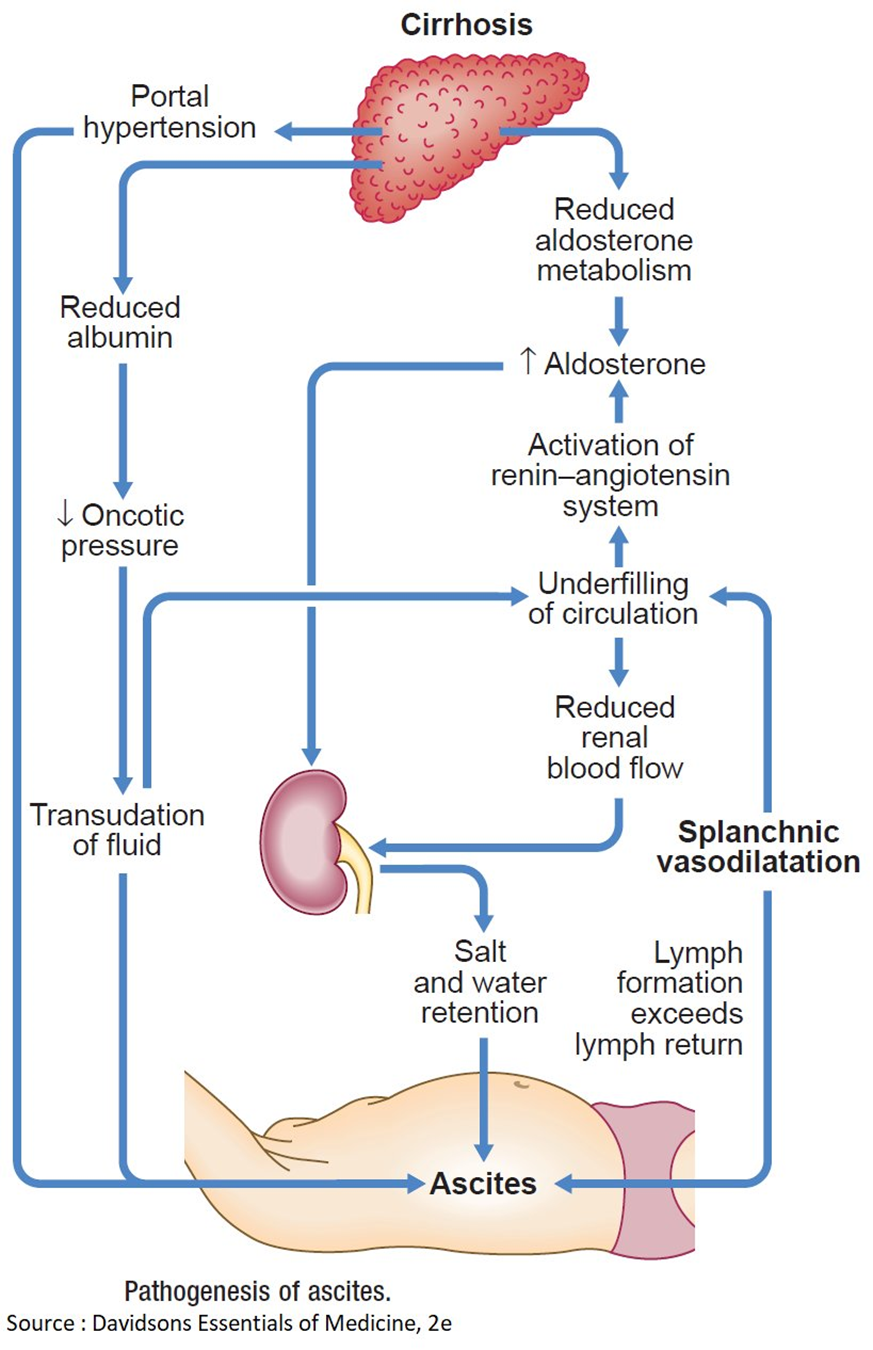
A. Hyperaldosteronism causing an increased sodium reabsorption in renal tubules.
Hyperaldosteronism is characterized by an excess of aldosterone, a hormone that regulates sodium and water balance. In cirrhosis, however, sodium retention is often related to other mechanisms such as portal hypertension and hypoalbuminemia, rather than hyperaldosteronism.
B. Decreased renin-angiotensin response related to an increase in renal blood flow.
Cirrhosis is more commonly associated with an activated renin-angiotensin-aldosterone system, leading to increased sodium and water retention. The increased renin-angiotensin response is a compensatory mechanism to maintain perfusion in the setting of cirrhosis and does not contribute to decreased renal blood flow.
C. Decreased portacaval pressure with greater collateral circulation.
This statement is not accurate. In cirrhosis, there is typically increased portacaval pressure due to portal hypertension, which can lead to the development of collateral circulation. However, this does not explain the edema and ascites seen in cirrhosis.
D. Hypoalbuminemia that results in a decreased colloidal oncotic pressure.
This is the correct choice. In cirrhosis, liver damage leads to decreased synthesis of albumin. Albumin plays a crucial role in maintaining colloidal oncotic pressure, and when it is decreased (hypoalbuminemia), fluid is more likely to leak out of blood vessels, resulting in edema. The same mechanism contributes to the development of ascites in the abdominal cavity.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
