After initiating a steroid nebulizer treatment for a client with asthma in respiratory distress, which intervention is most important for the nurse to implement?
Monitor pulse oximetry every 2 hours.
Teach proper use of a rescue inhaler.
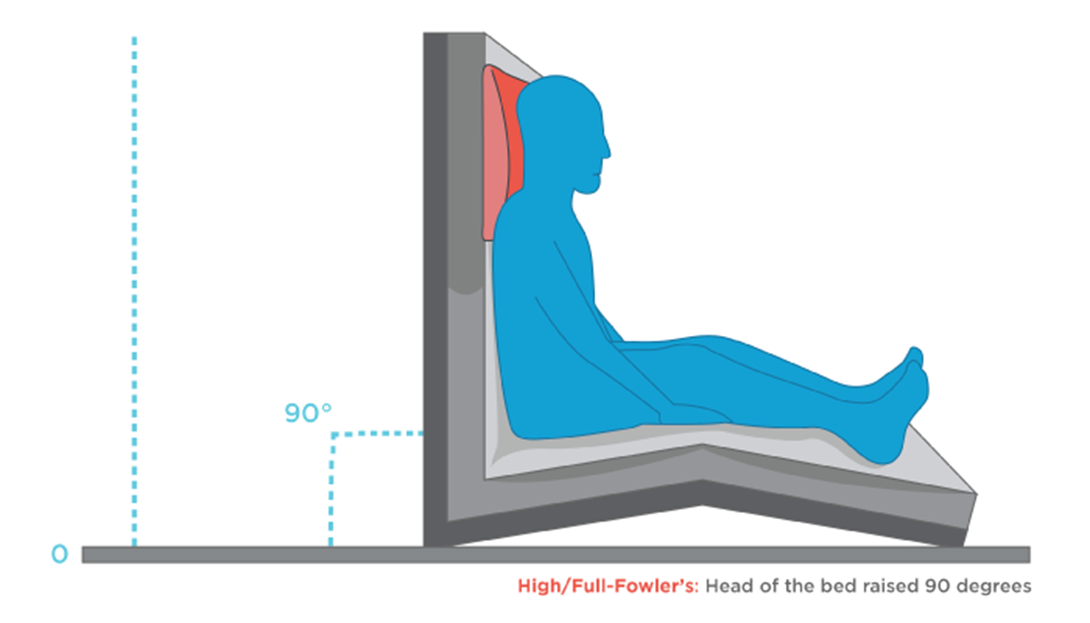
Elevate the head of bed to 90 degrees.
Determine exposure to asthmatic triggers.
The Correct Answer is C
Choice A reason: This is incorrect because monitoring pulse oximetry every 2 hours is not a sufficient or timely intervention for the nurse to implement. Pulse oximetry is a noninvasive method of measuring the oxygen saturation of hemoglobin in the blood. Normal oxygen saturation is 95% to 100%, while hypoxemia is less than 90%. However, pulse oximetry may not reflect the severity of respiratory distress or the effectiveness of nebulizer treatment in a client with asthma. Moreover, monitoring pulse oximetry every 2 hours is too infrequent for a client who is in acute respiratory distress and needs more frequent assessment and intervention.
Choice B reason: This is incorrect because teaching proper use of a rescue inhaler is not a priority or relevant intervention for the nurse to implement. A rescue inhaler is a type of short-acting bronchodilator that can be used to relieve acute asthma symptoms by relaxing the smooth muscles of the airways and improving airflow. However, teaching proper use of a rescue inhaler is not an urgent action for a client who is already receiving nebulizer treatment, which delivers a higher dose of medication directly to the lungs. Moreover, teaching proper use of a rescue inhaler is not appropriate for a client who is in respiratory distress and may not be able to focus or retain information.
Choice C reason: This is correct because elevating the head of bed to 90 degrees is the most important intervention for the nurse to implement. Elevating the head of bed to 90 degrees can help improve breathing and oxygenation by reducing pressure on the diaphragm and chest wall, increasing lung expansion and ventilation, and facilitating expectoration of mucus. This can enhance the effects of nebulizer treatment and reduce respiratory distress in a client with asthma.
Choice D reason: This is incorrect because determining exposure to asthmatic triggers is not an immediate or helpful intervention for the nurse to implement. Asthmatic triggers are substances or factors that can cause or worsen asthma symptoms by inducing inflammation or constriction of the airways. Examples of asthmatic triggers include allergens, irritants, infections, exercise, stress, or weather changes. However, determining exposure to asthmatic triggers is not a priority action for a client who is in respiratory distress and needs more urgent interventions to improve breathing and oxygenation. Moreover, determining exposure to asthmatic triggers may not change the management or outcome of an acute asthma attack that has already occurred.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
Choice A reason: Using incentive spirometer is not an information that the nurse should include in the discharge instructions for a client with BPH following a TUNA, because it is not related to the procedure or the condition. The incentive spirometer is a device that helps improve lung function and prevent respiratory complications by encouraging deep breathing and coughing. Therefore, this choice is incorrect.
Choice B reason: Monitoring urinary stream for decrease in output is an information that the nurse should include in the discharge instructions for a client with BPH following a TUNA, because it can indicate urinary retention or obstruction, which are potential complications of the procedure. The client should report any difficulty or inability to urinate, severe pain, or fever to the health care provider. Therefore, this choice is correct.
Choice C reason: Reporting when hematuria becomes pink tinged is not an information that the nurse should include in the discharge instructions for a client with BPH following a TUNA, because it is not a sign of a problem. Hematuria, or blood in the urine, is a common and expected finding after the procedure, and it usually resolves within a few days. The client should drink plenty of fluids to flush out the blood clots and debris. Therefore, this choice is incorrect.
Choice D reason: Restricting physical activities is an information that the nurse should include in the discharge instructions for a client with BPH following a TUNA, but it is not the best answer. The client should avoid strenuous activities, such as lifting heavy objects, driving, or sexual intercourse, for at least two weeks after the procedure to prevent bleeding and infection. However, this information is less important than monitoring urinary stream for decrease in output. Therefore, this choice is not the best answer.
Correct Answer is B
Explanation
Choice A reason: This is incorrect because teaching the client to wear a mask, hand wash, and social distance is not the most important action for the nurse to take. These are preventive measures that should be followed by everyone, regardless of their COVID-19 status.
Choice B reason: This is correct because isolating the client from other clients, family, and healthcare workers not wearing proper PPE is the most important action for the nurse to take. This is to prevent transmission of COVID-19 to others who may be at risk of severe complications or death.
Choice C reason: This is incorrect because reporting the COVID-19 result to the local health department according to CDC guidelines is not the most important action for the nurse to take. This is a legal and ethical obligation that should be done after confirming the diagnosis, but it does not have an immediate impact on the client's health or safety.
Choice D reason: This is incorrect because explaining to the client to inform others that they may have been potentially exposed in the last 14 days is not the most important action for the nurse to take. This is a moral and social responsibility that should be done as soon as possible, but it does not address the urgent need of isolating the client from potential sources of infection.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
