A student nurse asks the RN about the clinical manifestations of a thoracic aortic aneurysm. Which of the following findings should the nurse discuss? (Select all that apply).
Shortness of breath
Difficulty swallowing
Upper chest pain
Diaphoresis
Cough
Hoarseness
Correct Answer : A,B,C,E,F
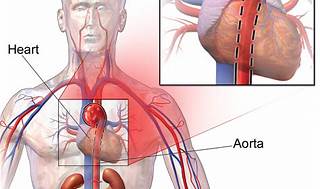
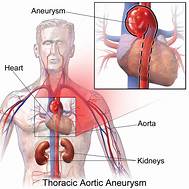
Choice A: Shortness of breath Shortness of breath can occur with a TAA due to the aneurysm compressing the trachea or the lung tissue. As the aneurysm enlarges, it can impinge on respiratory structures, leading to difficulty in breathing. A thoracic aortic aneurysm (TAA) is a bulging or dilation in the wall of the aorta as it passes through the chest cavity. TAAs can be life-threatening if they rupture or dissect and are often difficult to detect because they tend to grow slowly and usually do not cause symptoms until they become large or rupture.
Choice B: Difficulty swallowing Difficulty swallowing, or dysphagia, may be experienced if a TAA exerts pressure on the esophagus. This can happen when the aneurysm is located in the aortic arch, where the esophagus is in close proximity.
Choice C: Upper chest pain Upper chest pain is a common symptom of TAA and may be described as a deep, steady pain that can radiate to the back, neck, or jaw. The pain is caused by the stretching of the aortic wall and may be a warning sign of an impending rupture.
Choice D: Diaphoresis Diaphoresis, or excessive sweating, is not typically a direct symptom of a TAA. However, it can be associated with acute aortic syndromes, such as aortic dissection or rupture, which are medical emergencies.
Choice E: Cough A persistent cough can be a sign of a TAA, especially if the aneurysm is pressing against the trachea or bronchial tubes. The cough may sometimes produce blood if the aneurysm is causing erosion into these structures.
Choice F: Hoarseness Hoarseness can result from a TAA if the aneurysm compresses the recurrent laryngeal nerve, which controls the muscles of the voice box. This is known as Ortner’s syndrome or cardiovocal syndrome.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is D
Explanation
Choice A: Lactated Ringer’s
Lactated Ringer’s solution is an isotonic crystalloid that contains electrolytes similar to those found in blood plasma. While it is commonly used for fluid resuscitation, it does not provide a significant source of calories and therefore is not the best option to temporarily replace TPN.
Choice B: 0.9% sodium chloride
0.9% sodium chloride, also known as normal saline, is an isotonic solution that is used to expand volume and correct electrolyte imbalances. Like Lactated Ringer’s, it does not contain a significant amount of calories and is not suitable as a temporary replacement for TPN.
Choice C: 3% sodium chloride
3% sodium chloride is a hypertonic saline solution used in controlled settings to treat specific conditions such as hyponatremia. Due to its high concentration of sodium, it is not appropriate for routine fluid replacement and does not provide calories.
Choice D: Dextrose 10% in water
D10W is the preferred choice in this scenario because it provides a source of glucose, which can help maintain blood glucose levels when TPN is not available. It is important to monitor the patient’s blood glucose levels while infusing D10W to ensure they remain within a safe range. When a TPN container is delayed, Dextrose 10% in water is the most appropriate temporary solution to infuse until the next container becomes available, as it provides necessary calories in the form of glucose to the patient.
Correct Answer is D
Explanation
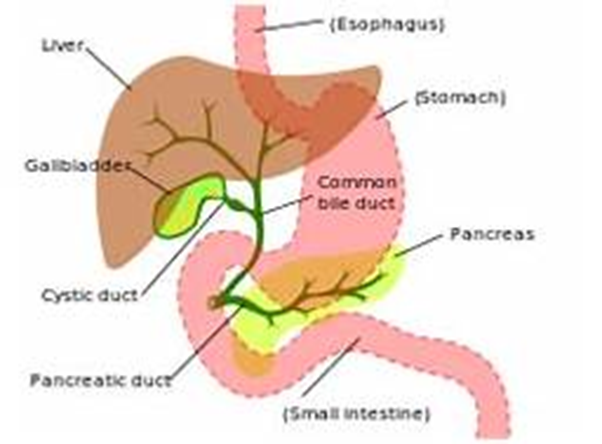
Choice A reason: Tenderness in the left upper abdomen is not typically associated with an obstruction of the common bile duct. This symptom is more commonly related to conditions affecting the stomach, pancreas, or spleen. The common bile duct is in the right upper quadrant of the abdomen, and tenderness in this area might be expected with its obstruction.
Choice B reason: Ecchymosis of the extremities is not a common finding in common bile duct obstruction. Ecchymosis, or bruising, is usually due to trauma, blood disorders, or other causes of fragile blood vessels and is not related to bile duct issues.
Choice C reason: Pale-colored urine is the opposite of what might be expected with common bile duct obstruction. Typically, the urine may become dark due to increased bilirubin levels that are excreted by the kidneys when the bile duct is obstructed.
Choice D reason: Fatty stools, or steatorrhea, are a classic finding in common bile duct obstruction. When bile flow is blocked, fats are not properly digested and absorbed, leading to stools that are bulky, greasy, and often have a foul odor. This occurs because bile is necessary for the emulsification and absorption of dietary fats in the intestine.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
