A nurse is providing education to a client who has hypoglycemia. Which of the following information should the nurse include about the regulation of blood glucose levels?
The adrenal glands release epinephrine and norepinephrine to respond to low blood glucose.
The liver releases glucagon to regulate blood glucose levels.
Glycogenesis occurs in the pancreas when blood glucose levels fall.
The brain uses protein for energy if glucose levels fall too low.
The Correct Answer is A
Choice A Reason:
The adrenal glands play a crucial role in responding to low blood glucose levels by releasing epinephrine (adrenaline) and norepinephrine. These hormones help to increase blood glucose levels by stimulating glycogenolysis (the breakdown of glycogen to glucose) and gluconeogenesis (the production of glucose from non-carbohydrate sources) in the liver. This response is part of the body’s fight-or-flight mechanism, which ensures that sufficient glucose is available for immediate energy needs.
Choice B Reason:
The liver does not release glucagon; rather, it responds to glucagon, which is released by the pancreas. Glucagon stimulates the liver to convert stored glycogen into glucose (glycogenolysis) and to produce glucose from non-carbohydrate sources (gluconeogenesis). This process helps to raise blood glucose levels when they are low.
Choice C Reason:
Glycogenesis is the process of converting glucose into glycogen for storage, and it occurs primarily in the liver and muscle cells, not in the pancreas. The pancreas releases insulin to promote glycogenesis when blood glucose levels are high, but it does not perform glycogenesis itself.
Choice D Reason:
The brain primarily uses glucose for energy and does not switch to using protein unless glucose levels are extremely low and prolonged. In such cases, the brain can use ketone bodies derived from fat as an alternative energy source. Protein is not a primary energy source for the brain under normal conditions.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
Choice A: Dietary and Fluid Restrictions
Dietary and fluid restrictions are crucial for patients with heart failure. These restrictions help manage symptoms and prevent complications. Limiting sodium intake can reduce fluid retention, which decreases the workload on the heart. Fluid restrictions help prevent fluid overload, which can lead to worsening heart failure symptoms. Patients are often advised to monitor their weight daily to detect fluid retention early. This choice is essential for managing heart failure effectively.
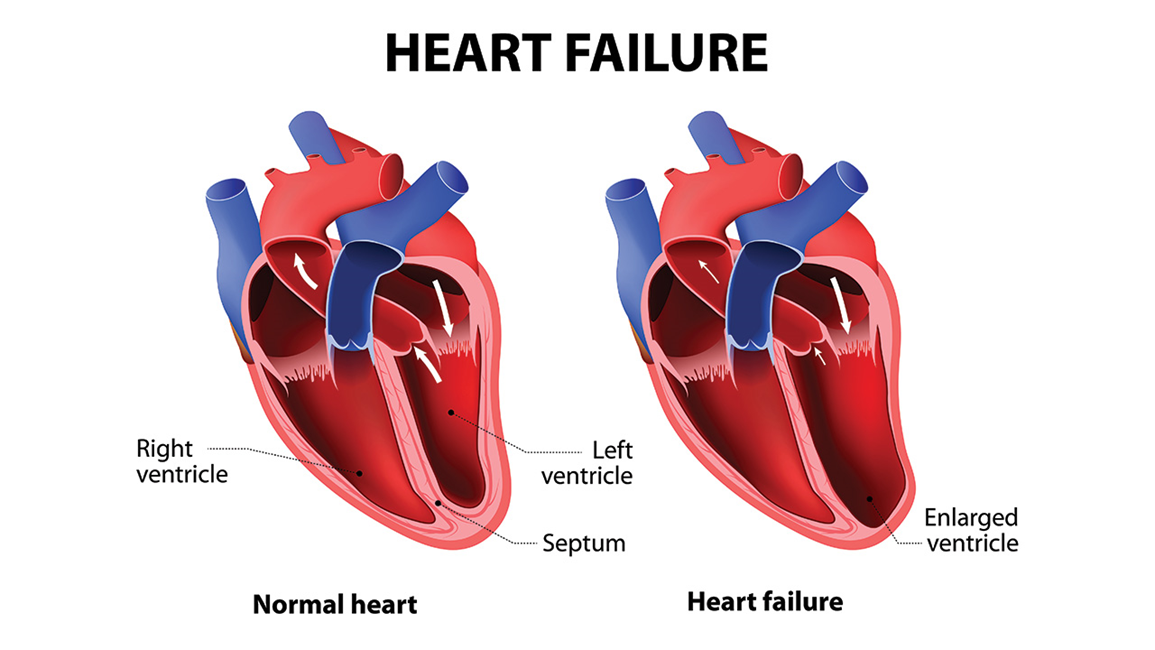
Choice B: Encouraging Increased Mobility
While physical activity is generally beneficial for overall health, it must be approached cautiously in patients with heart failure. Encouraging increased mobility without proper medical guidance can lead to overexertion and exacerbate heart failure symptoms. Exercise programs for heart failure patients should be tailored and supervised by healthcare professionals to ensure safety and effectiveness. Therefore, this choice is not as immediately critical as dietary and fluid restrictions.
Choice C: Cessation of Hormonal Supplements
Hormonal supplements can have various effects on the cardiovascular system, but their cessation is not a standard recommendation for all heart failure patients. The impact of hormonal supplements depends on the specific type and the patient’s overall health condition. This choice is less relevant compared to dietary and fluid restrictions, which have a direct and significant impact on heart failure management.
Choice D: Cessation of Intravenous (IV) Drug Use
Cessation of intravenous drug use is important for overall health and preventing infections, but it is not specific to heart failure management. While IV drug use can lead to complications that may affect the heart, it is not a primary lifestyle modification recommended for heart failure patients. The focus should be on managing fluid balance and dietary intake
Correct Answer is C
Explanation
Choice A Reason:
While monitoring the frequency of urination is important for managing diabetes insipidus, it is not the most critical aspect of discharge teaching. Diabetes insipidus causes excessive urination, and patients should be aware of this symptom. However, understanding the importance of wearing a medical alert bracelet is more crucial for ensuring immediate and appropriate care in emergencies.
Choice B Reason:
Changes in appetite are not a primary concern for patients with diabetes insipidus. The condition primarily affects fluid balance and urine output rather than appetite. Therefore, this topic is less relevant compared to the need for a medical alert bracelet.
Choice C Reason:
The benefit of a medical alert bracelet is paramount for patients with diabetes insipidus. In case of an emergency, the bracelet can inform healthcare providers about the patient’s condition, ensuring they receive appropriate and timely treatment. This can be life-saving, especially if the patient is unable to communicate their medical history.
Choice D Reason:
Weight gain or loss can be a secondary concern for patients with diabetes insipidus, as the condition primarily affects fluid balance. While it is important to monitor weight to assess fluid status, it is not as critical as ensuring the patient understands the importance of wearing a medical alert bracelet.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
