A nurse is documenting client care. Which of the following abbreviations should the nurse use?
"OJ" for orange juice
"SS" for sliding scale
"SQ" for subcutaneous
"BRP" for bathroom privileges
The Correct Answer is D
a. "OJ" for orange juice is not recommended. While it might seem straightforward, "OJ" could be confused with "oj" or other abbreviations, leading to potential confusion. It's better to write out "orange juice."
b. "SS" for sliding scale is not recommended" could be misinterpreted or confused with other meanings. It's safer to write out "sliding scale."
c. SQ is commonly mistaken as “5 every”. Use SUBQ (all UPPERCASE letters, without spaces or periods between letters), or subcutaneous(ly).
d. This is a commonly accepted abbreviation in medical documentation, meaning bathroom privileges.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
Choice A reason:
Wearing a mask when outside of the room is not a standard practice for all patients undergoing an allogeneic stem cell transplant. The need for mask use may vary based on the patient's specific condition and the facility's infection control protocols.
Choice B reason:
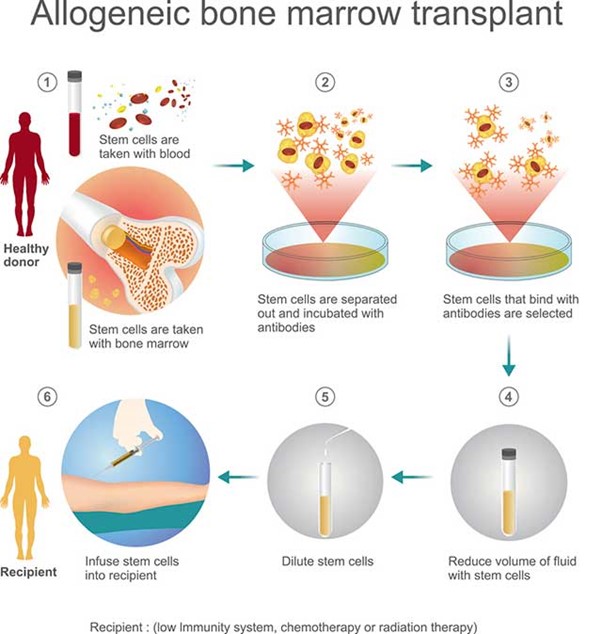
"You will be in a negative-airflow room to keep the air cleaner." This is the appropriate answer. An allogeneic stem cell transplant involves replacing the patient's damaged or diseased bone marrow with healthy donor stem cells. Patients undergoing this type of transplant have compromised immune systems due to the treatment, which increases the risk of infection. Placing the patient in a negative-airflow room helps prevent the spread of airborne infections by ensuring that air flows into the room but does not escape into other areas of the facility
Choice C reason:
Visitors wearing protective gowns is not a standard practice for all patients undergoing an allogeneic stem cell transplant. Visitor guidelines may depend on the patient's immune status and specific infection control measures.
Choice D reason:
Being placed in a semi-private room is not recommended for patients undergoing an allogeneic stem cell transplant. These patients require a controlled environment to reduce the risk of infections, and private rooms with proper infection control measures are generally preferred.
Correct Answer is C
Explanation
Choice A reason:
Placing the wasted portion of the controlled substance in the sharp container is not correct. Wasted controlled substances should be disposed of according to specific regulations and facility protocols.
Choice B reason:
Asking a second nurse to record her signature when wasting an unused portion of the controlled substance is not a standard practice. The process for wasting controlled substances usually involves following specific documentation procedures, but this does not necessarily require a second nurse's signature.
Choice C reason:
Verifying the count total of the controlled substance after removing the amount needed is the appropriate action. When administering a controlled substance, it is crucial to maintain accurate accountability of the medication. This includes verifying the count total of the controlled substance before and after removing the amount needed for administration. This step helps ensure proper documentation, prevent errors, and maintain appropriate control over controlled substances.
Choice D reason:
Reporting any discrepancy in the count total of the controlled substance after administration is important, but it should be done as a separate step from verifying the count total before administration. Discrepancies should be reported according to facility policy to ensure proper investigation and resolution.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
